What to know about the spread of Candida auris, the drug-resistant fungal infection, in Pennsylvania
A new CDC report noted that clinical cases of Candida auris tripled between 2019 and 2021 nationwide. In 2022, Pennsylvania identified 33 clinical cases of the fungus in patients around the state.
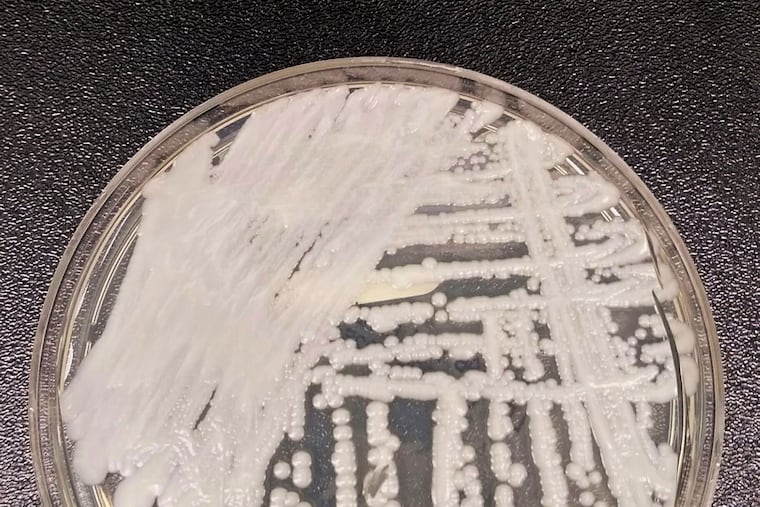
Researchers at the Centers for Disease Control and Prevention this week sounded the alarm on the spread of Candida auris, a fungus affecting mainly hospitalized patients that can be resistant to the medications typically prescribed for fungal infections.
The CDC report noted that cases of Candida auris tripled between 2019 and 2021 nationwide. In 2022, Pennsylvania identified 33 cases of the fungus in patients around the state.
The fungus is also likely drawing more attention because of the popularity of The Last of Us, the HBO series set in an America ravaged by a fungus-induced zombie apocalypse. That fungus is based on Ophiocordyceps unilateralis, or cordyceps, which, in the real world, affects only insects.
Says Eric Sachinwalla, a Philadelphia physician specializing in infectious diseases and a fan of the video games the show is based on: “Candida auris shouldn’t make anyone into a zombie, so that’s a good thing.”
Here’s what to know about the fungus in Pennsylvania, who is at risk, and what local hospitals are doing to protect patients:
What is Candida auris, and why are health officials concerned about it?
C. auris is a type of yeast organism, although it’s not responsible for the yeast infections commonly seen in women. “It’s related to other, more common yeasts that many of us have in our body naturally. They live in our intestinal tract, oral flora, and vaginal flora — yeast infections are caused by another species of Candida,” said Sachinwalla, the medical director for infection prevention and control at Einstein Medical Center Philadelphia, a division of Jefferson Health.
But C. auris is a newer species of yeast that was identified only in 2009, according to the CDC. It’s mostly found in hospital settings, and people who have spent long periods in hospitals, been treated with antibiotics, or have lines and tubes such as catheters or tracheostomy tubes are particularly at risk.
“This one tends to be more resistant to our typical antifungal medications,” Sachinwalla said.
The CDC says most C. auris infections are treatable with a certain class of antifungal medication. But for resistant cases, doctors might need to administer several different antifungal medications at the same time.
Why does C. auris affect patients who have spent a long time in the hospital?
The people at highest risk for Candida auris are people who have spent significant amounts of time in hospitals or long-term care facilities, Sachinwalla said.
Many such patients are treated with powerful antibiotics that, while successful in fighting bacterial infections, can also target “good” bacteria that help prevent fungal infections such as C. auris, he said.
“One of the things that healthy bacteria do is crowd out bad organisms,” Sachinwalla said. “When your body is exposed to more and more antibiotics over time, the chances of becoming colonized or infected with resistant organisms are greater.”
Patients who require long hospital stays or long-term care are also generally frailer and suffer from other conditions that may make them more vulnerable. But, the CDC says, C. auris has been detected in patients of all ages, and more research is needed on its risk factors.
What are the symptoms of a Candida auris infection? Can it be fatal?
That depends on where the infection presents. People with urinary catheters who develop an infection might get a fever or pain around the bladder. Tracheostomy patients might see more mucus buildup in their trach tube, develop a fever, or have difficulty breathing. People with catheters in their veins could get a blood infection, fever, a high heart rate, or low blood pressure, Sachinwalla said.
Candida yeasts can cause fatal infections, the CDC says, but the rate of death is still unclear. “We don’t know if patients with invasive C. auris infection are more likely to die than patients with other invasive Candida infections,” CDC officials wrote in a Q&A on the agency’s website.
“Based on information from a limited number of patients, 30% to 60% of people with C. auris infections have died,” the CDC noted. But many of those people also had other illnesses that increased their risk of dying.
What is the prevalence of Candida auris in Pennsylvania?
Pennsylvania saw 33 clinical cases of Candida auris in 2022, according to the CDC. That’s up from 12 cases in 2021, and just four cases in 2020. The CDC draws a distinction between a clinical case, where a patient is displaying symptoms of infection and doctors determine that Candida auris is causing them, and a “colonization case,” where a patient is found to be carrying the fungus but isn’t sick.
CDC data don’t specify how many people were found to have been colonized with the fungus. But according to data from the state Health Department, between March 2020 and August 2022, health officials identified 144 total cases of people who either had become sick from the fungus, or were colonized with it, mostly concentrated in Southeastern Pennsylvania. The state data did not specify how many patients had symptoms, and how many were only colonized.
At Einstein, Sachinwalla said, staff have treated one to two patients who were known to be colonized with C. auris. “They came to our hospital for unrelated issues,” he said. “We addressed that, kept those patients isolated, and used appropriate disinfectants to clean their rooms.”
It’s possible that shortages of personal protective equipment during the pandemic, as well as an increase in patients who needed ventilators or longer-term nursing care because of COVID-19, contributed to the increase, Sachinwalla said.
Most cases, though, are found in hospitals, Sachinwalla said: “I don’t think there are many people walking around in the community who have it.”
How can hospitals prevent Candida auris?
Hospitals and health-care facilities typically disinfect rooms where patients have stayed. Now, with the rise of C. auris, hospitals should ensure that the disinfectants they use are effective against the fungus. Einstein has updated its own cleaning processes to that effect, Sachinwalla said.
Hospitals and long-term care facilities can also use antibiotics “judiciously” to lessen patients’ risk of contracting a fungal infection, he said.
“For the vast majority of people, this isn’t anything to be alarmed about,” he said.