Penn expert says whether to take antidepressants during pregnancy is a ‘risk-risk conversation’
A Penn researcher found the risk of a mental health emergency nearly doubled in women who discontinued their SSRIs or SNRIs, compared to those who stayed on their medication.
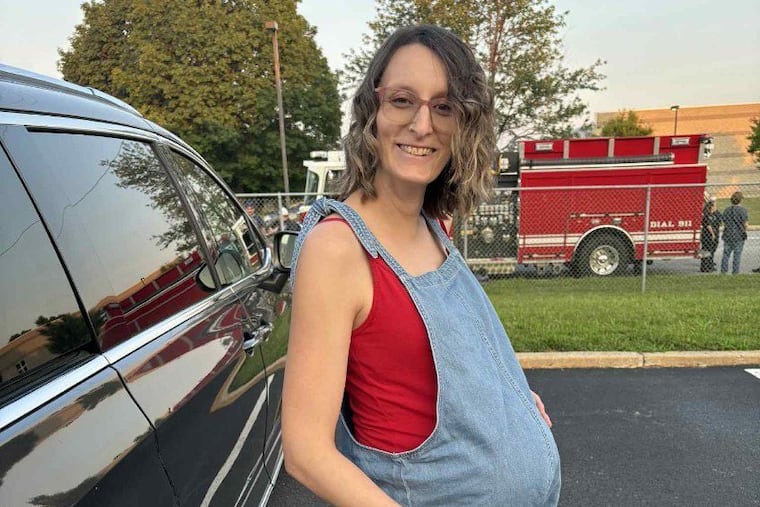
When Sarah Bynum was pregnant with her first child in 2017, her primary care doctor suggested she stop taking her antidepressant.
He told her there wasn’t enough research to justify staying on the medication.
By the time she delivered her daughter, the Delaware County woman’s anxiety was so bad that she decided never again to go through a pregnancy without her antidepressant.
Bynum, who has taken medication for anxiety since she was a teenager, is one of the nearly 18% of women in the U.S. on an antidepressant. She takes a drug known as an SSRI, the most common class of antidepressants, which medical societies generally consider safe to use during pregnancy.
Still, roughly half of women taking an antidepressant discontinue their use of the medication while pregnant, according to a 2025 study in the medical journal JAMA Network Open.
Kelly Zafman, an OB-GYN at the Hospital of the University of Pennsylvania, decided to research the issue that has also recently been under discussion on the federal level. She’s observed that patients often get mixed-messaging from providers.
“The other side of the conversation that gets missed is this risk of not continuing medications,” said Zafman, who is in her final year of fellowship training in maternal-fetal medicine.
Preliminary findings from her research showed the risk of a mental health emergency nearly doubled in women who discontinued SSRIs or SNRIs (another popular type of antidepressant), compared to those who stayed on their medication. She presented the unpublished results this month at the meeting of the Society for Maternal-Fetal Medicine.
The analysis used data from 1,462 privately insured Pennsylvania women with active antidepressant prescriptions who gave birth between 2023 and 2024. While pregnant, 81% of them stopped or interrupted usage.
Zafman said the highly personal decision comes down to factors such as the patient’s prior pregnancies, mental health history, and how well-controlled their symptoms are.
Ultimately, the potential risks have to be weighed against those of untreated depression or anxiety.
“It’s really a risk‑risk conversation," Zafman said.
Evolving research
The American College of Obstetrics and Gynecologists discourages discontinuing antidepressants based on pregnancy alone, highlighting the risks of untreated mental health conditions. Studies have linked uncontrolled depression during pregnancy with preterm birth, low birth weight, higher suicide risk, and impaired mother-infant attachment.
Research on the safety of antidepressants in pregnancy continues to evolve. Some potential risks identified in older research appear overstated when compared with more recent, better-designed studies, Zafman said.
She cited as an example a rare but serious condition called persistent pulmonary hypertension — which causes a breathing issue — for which scientific evidence remains conflicting.
“There’s definitely an association, but it’s not totally clear how causative it is,” Zafman said.
Another concern, neonatal adaptation syndrome, tends to involve mild difficulties with feeding and breathing that resolve within days. Medical intervention is rarely required, and the treatment essentially is to cuddle and feed your baby, Zafman said.
While antidepressants potentially pose risks in pregnancy, she said, overall, the risks of long lasting effects are “extraordinarily low.”
A personal decision
Bynum, a patient at Penn Medicine, was not on antidepressants during her first pregnancy. (She was not part of this particular study but has participated in other research with Zafman.)
Five months into the pregnancy, she learned her daughter would be born with a congenital heart defect that would require monitoring, and later, surgery.
Family and friends tried to help her, but they weren’t able to calm her heightened anxiety the way her medication usually would.
When she became pregnant with her second child, she knew she wanted to have a “more mentally healthy pregnancy.”
“I needed to be mentally and physically present not just for myself, but my daughter,” she said.
She asked her OB-GYNs if she could continue on her antidepressant, Paxil. They weren’t sure.
She turned to the fetal heart experts at Children’s Hospital of Philadelphia, who looked into the medical evidence and told her it was fine to continue taking her antidepressant.
Bynum has since had three healthy pregnancies while taking the antidepressant.
She felt it was the right decision.
“I need to focus on having a healthy pregnancy with as minimal stress as possible,” Bynum said. “And if that means taking a medication, that’s what’s gonna work.”
Editor’s note: This story has been updated to clarify a quote by the researcher.