When malpractice occurs at community health centers, taxpayers pay
Settlements and judgments nationwide involving community health centers totaled $410 million from 2018 through 2021, according to federal data.
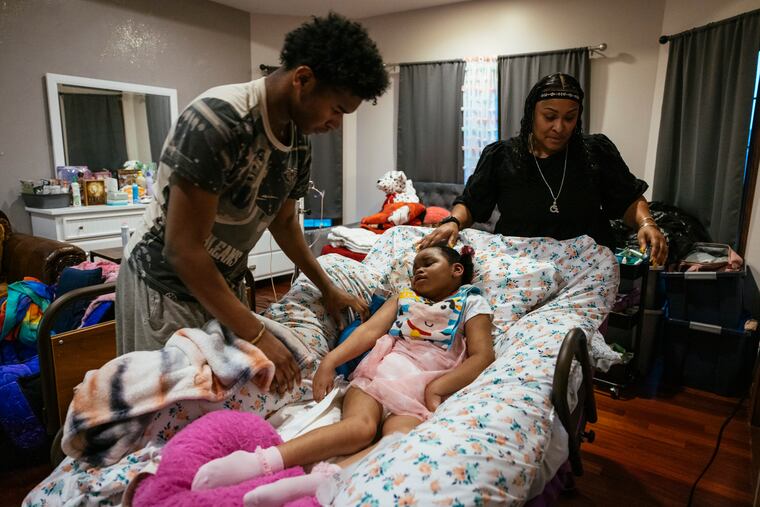
Christina Late’s son has permanent brain damage, struggles to communicate, can’t walk, and will never live independently because a Pennsylvania doctor crushed part of his skull with forceps during delivery.
Akimbee Burns had a Pap smear at a community health center in Georgia that showed abnormal cells. But she was not told of the results. About eight months later, she was diagnosed with cervical cancer that had spread to her lymph nodes. She died within two years, at age 38.
Rhonda Jones’ baby was left brain damaged after her Chicago-area medical team, which included community health center doctors, failed to perform an emergency cesarean section quickly enough, even though Jones was at high risk for labor complications.
These three cases — alleged in court documents as part of malpractice lawsuits that were settled without admission of wrongdoing — are among 485 payouts made nationwide involving community health centers from 2018 through 2021. The settlements and judgments totaled $410 million, paid to the patients or their families, according to federal data released to Kaiser Health News through a public records request.
But none of those health centers, and none of the doctors, paid anything. U.S. taxpayers picked up the tab.
The nation’s 1,375 federally qualified health centers, which treat 30 million low-income Americans, are mostly private organizations. Yet they receive $6 billion annually in federal grants, and under federal law their legal liabilities are covered by the government, just as those of the U.S. Department of Veterans Affairs and the Indian Health Service are. That means the centers and their employees can receive immunity from medical malpractice lawsuits and the federal government pays any settlements or court judgments.
As a result, the public is often unaware of malpractice allegations against those centers. The health centers and their employees are not named as defendants in the lawsuits, and the government does not announce when it pays to settle cases or court judgments.
In addition, lawyers who have represented plaintiffs in lawsuits against health centers say federal rules handcuff patients with a short statute of limitations — two years — and do not allow punitive damages.
“It doesn’t matter how bad the doctor’s care is,” said Regan Safier, a Philadelphia lawyer who won a $41.6 million court judgment in Late’s birth injury case in 2017. Yet the doctor still practices in Pennsylvania, she noted.
Tragedies hidden from view
From 2018 through 2021, the median payment for malpractice settlements or judgments involving health centers was $225,000, according to the data from the Health Resources and Services Administration, which oversees the community health centers. In 68 of the 485 payouts, the total was at least $1 million.
Many of the lawsuits against health centers involved allegations of misdiagnosis or dental errors. Most large awards were for birth injuries or cases involving children.
The $41.6 million awarded to Late, Nathan Armolt and their son is the largest between 2018 and 2021, according to KHN analysis.
In February 2012, when she was 40 weeks pregnant, Late went into labor and was admitted to Chambersburg Hospital in south central Pennsylvania. Her labor was long, but nurses and the on-call obstetrician monitoring all night reported in their notes that she was progressing normally, with no concerns for her or the baby’s health, according to court documents.
The next morning, a new doctor took over. Thomas Orndorf, who worked for the federally funded Keystone Women’s Center, let her push only once, then made two unsuccessful attempts to deliver the baby using forceps — against hospital guidelines that call for such aided deliveries in emergencies or after the mother has been pushing for hours, according to court documents.
Late eventually delivered the baby by pushing. But the forceps had crushed parts of the baby’s skull, causing permanent brain damage and lifelong disabilities. Her son will never be able to live independently, and will need to be moved to an assisted living facility when he is an adult, and his parents are unable to manage his care alone, according to court documents.
In 2017, when a federal judge ordered the government to pay nearly $42 million, Keystone Health CEO Joanne Cochran said Keystone was “saddened by the outcome of this delivery and for the hardships this child and family have experienced and will continue to endure.”
“Keystone has taken all the necessary quality assurance steps so that this does not happen in the future. Each and every patient is important to us and a part of our Keystone family, and we strive to treat them as such,” she told local media outlets.
The award will ensure that Late and Armolt can afford the advanced medical care their son will need the rest of his life, but did little to legally hold the doctor or health system accountable, Safier said.
Protected from malpractice
Federally qualified health centers differ from other clinics because they receive federal grant funding annually. They also receive higher reimbursements from Medicaid and Medicare than do private doctors. In return, the centers are not allowed to turn anyone away, and charge low-income patients on a sliding scale. Nearly half of the centers’ patients are covered by Medicaid, and 20% are uninsured.
Community health centers pushed for — and won — government malpractice protection in the 1990s. They argued that their revenues were limited and that malpractice insurance would divert money that could better be used for patient care.
Immunity means that most federally qualified health center providers are not named as defendants in malpractice suits and, as a result, there is no judgment against them.
Malpractice lawsuits are a risk for all health care providers and are just one barometer of quality of care. The settlements and court judgments against the health centers don’t measure the clinics’ overall performance.
Even lawyers who have sued on behalf of health center patients acknowledge the importance of the facilities. Rhode Island plaintiff lawyer Amato DeLuca said that the health centers serve a vital role in the health industry and that he had found “a lot of really wonderful, extraordinarily capable people that do a really good job” at the centers.
Yet everyone must be held accountable for mistakes, DeLuca said.
Akimbee Burns’ case is an example of a missed diagnosis, according to the lawsuit she filed against the U.S. government. Burns, who made $11 an hour at a utility company, had a Pap smear in 2016 at South Central Primary Care Center, a community health center in Ocilla, Ga. The test results showed abnormal cells, but she was not informed of the results, according to the complaint. She inquired about the test several times in the following months but still was not informed about the results, she alleged.
About eight months later, the staff at a different health care facility diagnosed advanced cervical cancer. She filed a lawsuit alleging that the community health center had been negligent. She underwent radiation and chemotherapy. But she died in April 2019, leaving behind two children, including one minor.
After her death, the government and her estate settled for $2.1 million.
South Central Primary Care Center did not respond to requests for comment, and the government denied any wrongdoing.
Roadblocks for patients
A patient alleging medical malpractice by a health center must first submit claims to the U.S. Department of Health and Human Services for review. The government can make a settlement offer or deny the claim. If the claim is denied or not settled, or a six-month review period expires, the patient may sue in federal court under the Federal Tort Claims Act, or FTCA.
To get that federal protection, health centers must have quality improvement and risk management programs and must show regulators that they’ve reviewed the professional credentials, malpractice claims, and license status of their physicians and other clinicians.
Ben Money, a senior vice president for the National Association of Community Health Centers, said the process improves care and directs scarce operating dollars toward the needs of patients vs. costly malpractice coverage.
“There are rigorous safeguards in place to ensure that health center grantees are in compliance and that patients are getting the very best care,” he said. “FTCA makes health centers more vigilant on quality and not less.”
About 86% of community health centers were covered under the FTCA for medical malpractice coverage as of September, said Christy Choi, a spokesperson for the Health Resources and Services Administration.
She said the government has implemented “robust quality improvement and patient safety efforts” as part of the program.
The system makes collecting damages more difficult for patients than if they went to state courts for malpractice suits, said lawyers involved in cases against health centers. In addition to the prohibition against punitive damages, such cases are decided by federal judges instead of juries. The lack of a jury is important, they added, because judges are less likely to be swayed by emotion and that can mean lower dollar amounts in the awards.
Plaintiffs are also at a disadvantage because the federal government has unlimited resources to defend cases, unlike the patients and their lawyers, said Christopher Russomanno, a Miami lawyer.
“These cases cost hundreds of thousands of dollars for us to get ready for trial,” said Jack Beam, the Illinois lawyer who represented Rhonda Jones. “Our record was $900,000 in case costs.”
All these factors can make finding a lawyer an obstacle for patients.
Deborah Dodge, a Missouri lawyer, said some lawyers are reluctant to take the cases because the government caps their fees at 25% of the settlement amount. In contrast, plaintiff lawyers often take about 40% in successful state court malpractice cases.
Rhonda Jones was one of those who received a settlement. Her baby was taken to a children’s hospital soon after being born by emergency cesarean section at West Suburban Medical Center in the Chicago area in December 2016, according to her lawsuit. The baby, Alayna, was treated for brain damage from a lack of oxygen, and she now has cerebral palsy.
Jones showed signs of a high-risk delivery when she arrived at the hospital nearly 39 weeks pregnant: She was 40 years old, this was her 11th child, and she had severe preeclampsia and possibly gestational diabetes.
Her lawsuit alleged that she was not adequately monitored at the hospital and that surgery was not performed in time to prevent injury to Alayna.
Jones agreed to a $21 million settlement, $15 million of which was paid by the federal government because some of the doctors involved were employed by PCC Community Wellness Center. The health center and the hospital declined to comment. In court filings, the government and hospital denied wrongdoing.
The money — most of which is in a trust overseen by the court — provides for Alayna, who will require care throughout her life.
“Before what happened to Alayna, I loved them,” Jones said of the health center where she had gone for several of her previous pregnancies. “They were great for me because they would be open late at night when I was working.”
“I still would tell someone to go to PCC because maybe they will get the right doctors when they go to have their baby,” Jones added.
Inquirer reporter Sarah Gantz, KHN intern Alander Rocha and KHN reporter Colleen DeGuzman contributed to this article.
Kaiser Health News covers health issues.