The Eagles’ DeSean Jackson has a core muscle injury. What might that mean?
William C. Meyers, founder of Philadelphia's Vincera Institute and a pioneer in the diagnosis and treatment of core injuries, talks about his new book and the latest breakthroughs in his field.
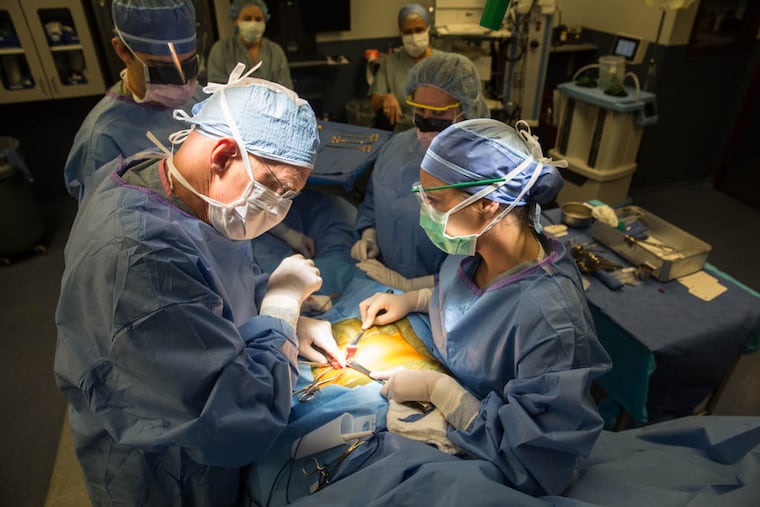
Editor’s note: The Eagles confirmed Monday that wide receiver DeSean Jackson will have surgery to correct a core muscle injury. Core injuries in athletes — once called sports hernias — are the specialty of renowned physician William C. Meyers, founder of the Vincera Institute, located in Philadelphia’s Navy Yard. Here is an interview with Meyers published in the Inquirer in June, after publication of his book, ‘Introducing the Core: Demystifying the Body of an Athlete.’
Bull riders. Long jumpers. Runners. Tennis pros. Football, baseball, basketball, hockey, and soccer players. Weekend warriors.
William C. Meyers has treated them all. What they shared were injuries that used to be called sports hernias. But Meyers has transformed the care of these afflictions, which now are referred to as core injuries.
In 2013, he established the Vincera Institute, located in the Navy Yard – near major sports facilities, it just so happens – dedicated to prevention, diagnosis and treatment of core injuries, plus the rehabilitation of patients and further research in the field. All of Philadelphia’s medical schools, plus the Hospital for Special Surgery in New York City and the Duke University Health System in Durham, N.C., participate.
His recent book, Introducing the Core: Demystifying the Body of an Athlete, distills what he has learned over the decades. We recently spoke to him about the body’s core and core injuries.
What is our core? Why is it important?
The core is defined as midthigh to midchest. It’s the trunk. It also just so happens to be the same as the strike zone in baseball, at least the way American League umpires call strikes these days. The core includes everything in there. It’s a network of muscles, tendons, ligaments, and joints. It’s major organs and large blood vessels.
It’s important because it’s our engine room. It’s where the center of our body is in terms of athleticism, in terms of movement. It has a tremendous amount to do with controlling the upper extremities and lower extremities.
It’s also the most misunderstood area of the body. This gets to the point of why medicine has not focused on the core. Physicians are looking at their areas of specialty, not the whole. So urologists think of the bladder and kidneys. Gynecologists think of a woman’s reproductive organs. The orthopedic surgeons are the ones who should be in there working with the muscles and bones, but they’re hesitant because of the organs and large blood vessels. No one is looking at the whole. The core seems complicated when you think of it as a unit, but it’s not.
What is a core muscle injury?
In terms of sports injuries, most of them occur in the core. Everyone is susceptible to them. Like most of us, as you progress in life, you get occupied by your profession, your children. You get out of shape. Then you try to get back into shape. If you get too vigorous, and you haven’t been using those muscles for a while, you rip them apart.
There are 35 different muscle groups in there. Any one of those can be injured. Most of the injuries don’t require surgery, but a bunch of them do. It really comes down to use, overuse, and understanding that you’ve got to apply these muscles together.
If you injure one of the muscles, if you get a shredding injury, then you start to compensate with the other muscles, and you wind up with a compensatory tug-of-war. The cartilage rubs, and it hurts. The whole art of treating these injuries is figuring out where the primary problem is, and where the secondary, compensatory injuries are. It’s usually a matter of repairing the primary, and then loosening the secondary ones.
When I was growing up, the coach would be the team doctor. He’d make a diagnosis in terms of whether someone could play, based on how tough he thought the guy was. Eventually, the athletic trainers were the ones who came to me. The team doctors had ignored these injuries. There had been no studies. Mark Price, the athletic trainer of the New York Jets, came to me and said: “Look, I’m convinced this guy has an injury. We just don’t know where it is.” We saw the fellow, and he had a distinct core injury, and we were able to help him.
How did you discover a new way of dealing with core injuries?
My overall background is that I went to Harvard and played a couple of sports, and then played professional soccer in Brazil. Then I went to medical school at Columbia University in New York and to Duke University, where I specialized in liver and gastrointestinal surgery. While I was there, I was asked to help take care of the athletic teams. I started seeing a lot of people with mysterious pain in the pelvis. The term sports hernia was used then. People were trying to repair them by putting mesh in, treating them like hernias. It just didn’t work. None of the injuries had anything to do with hernias.
It turned out that I was in a position to study this. We had just seen three athletes with pain in the pelvis. The common denominator was that the pain would migrate. It would start in one place, like the belly, and go to the thigh. This would happen over weeks or months. Doctors were looking for these little protrusions, which might be hernias. But that wouldn’t explain why the pain would migrate.
In the late 1980s, we were just starting a fresh cadaver lab, so we did an experiment. The cadaver was an athletic young male. He was on his back. I had my medical student put her index finger behind three of the muscles in the thigh and right on top of an edge of bone that is sharp. I wanted her to see if she could feel any change in pressure when I cut an abdominal muscle about a foot or so above her finger. As soon as I cut it, the whole bony pelvis abruptly shifted forward. The sharp bone rammed against her finger. She was hurting, but we were all excited. We had shown anatomically that even a relatively small cut in the muscle really affected the anatomy below. It was a eureka moment. That led to a lot of other experiments. The key to what we were doing was seeing that everything – the thigh muscles, the hip, everything – was all connected. That led us to the answers — how to fix a lot of the injuries.
Are any new developments on the horizon?
There are some important ones. They all have to do with understanding the far-reaching nature of these injuries. It turns out that a lot of pelvic pain in women actually comes from hip and muscle injuries in the pelvis instead of from gynecological problems. They manifest themselves through gynecological examinations, but they are hip and muscle injuries that are fixable. The appreciation of all that is a huge part of the future.
Another thing is that there is a connection between core injuries and cognition and the brain. It’s demonstrable. You have an injury in the pelvis, and you actually lose things like reaction time — reflexes, basically — and portions of your visual field. These things return to normal when the injury is fixed. In terms of athleticism, this has significance with return-to-play. It also is important when it comes to concussions. It also has to do with balance. In older people, falls are a concern. The more you can keep yourself fit in terms of core function, the longer you can have a good quality of life.
What does all this mean for weekend warriors?
Most people like the concept of staying in shape and equate longevity with fitness. But the weekend warriors are tremendously susceptible to these injuries because their fitness is so variable. We are seeing more and more people who have hurt themselves by engaging in occasional fitness. On the other hand, there are many people who have stopped staying in shape because they have injuries and they have just accepted it.
Knowing if you’re overdoing it is an important question. You really don’t, until you get injured. But there’s an old term in sports — playing within yourself. Not going to the extreme. You also want to vary what you do. Don’t work on just one muscle. Do planks, where you’re making all the muscles work together. And do things in a sequential way, so you’re not working out one muscle vs. another too much. Everything you do — even just getting up from the dinner table — involves a logical sequence of muscle contractions. You have to learn when you work out to have all those muscles function.