Forget anti-vaxxers. Bring vaccines to parents who desperately want them. | Opinion
Eradication in any given country is a temporary condition, because the virus isn’t going to respect borders.
With all the outrage aimed at so-called anti-vaxxers for causing the current U.S. measles outbreak, it’s easy to overlook the fact that the vast majority of measles deaths worldwide happen to children whose parents desperately wanted to get them vaccinated but couldn’t. By focusing efforts on developing countries where the outbreaks are many times bigger and deadlier, some scientists think it might be possible to eradicate the virus soon, as they did 40 years ago with smallpox.
Smallpox was an easier target because the virus is less contagious, so doctors didn’t have to get nearly as big a fraction of the population vaccinated to drive it to extinction, said Justin Lessler, an epidemiologist at Johns Hopkins University. But what we have now is better technology to track the virus around the globe and more precisely target vaccination strategies. In a recent issue of the journal Science, he and colleagues describe outbreak patterns they observed in global data from 1980 to 2017, and they discuss how to use them in an ongoing effort to eradicate the virus.
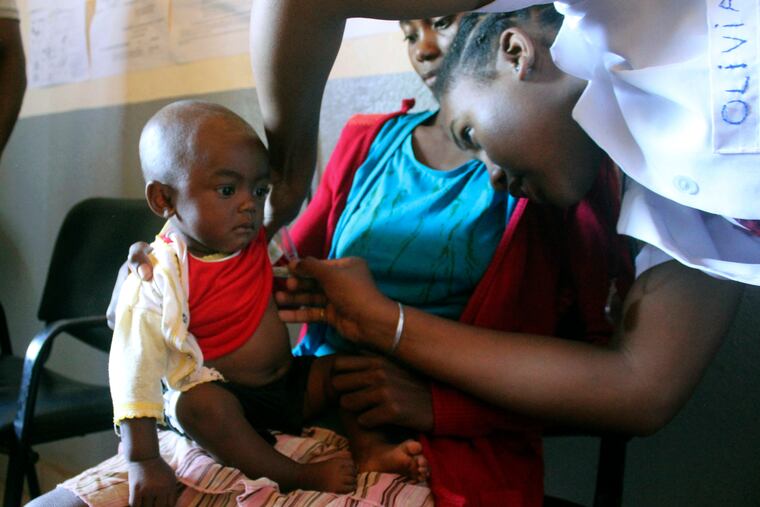
The quest deserves whatever support it needs to get the job done. In years when the U.S. was virtually measles-free, the disease was cropping up in outbreaks around the world, killing thousands every year. This year, a huge outbreak in Madagascar has killed more than 1,200 children. In developing countries, the same problems with the medical infrastructure that prevent high vaccination rates also make the disease much deadlier. In Madagascar, many people can’t afford to get infected kids to a hospital, and malnutrition is also increasing the death rate from measles.
Madagascar saw just a handful of cases in the years before the 2019 outbreak, which seemed to come out of nowhere. But this is actually part of a typical pattern. In a country that starts a vaccination campaign, rates of disease initially go way down, because vaccinations are helped by natural immunity among members of the community who’ve had the disease. But over time, the natural immunity helps less, and the country depends more and more on the vaccine. When there’s a high birthrate, the population of unvaccinated, susceptible people can start to grow.
“It can seem like they have elimination for a while, but it’s just a matter of time for a susceptible population to develop like fuel for a fire, and then there’s a spark,” said Lessler.
While each smallpox case infected four to six others, each person with measles can infect around 20. Because it's so contagious, countries need to achieve a very high vaccination rate — around 90 to 95% — to avoid future outbreaks.
In Madagascar and a number of other countries around the world, the vaccination rates had fallen to less than half of children — much lower than the near 91% rates that are achieved in the U.S. despite all the anti-vaccination rhetoric.
The initial decrease followed by irruptions of disease is what the scientists call a canonical pattern. By tracking where countries are on that trajectory, Lessler said, doctors can concentrate vaccination campaigns where they're most needed. And in some cases, they can do more good targeting older kids.
Eradication in any given country is a temporary condition, because the virus isn’t going to respect borders. While it’s easy enough for people in the U.S. to get their kids vaccinated, medical misinformation on the dangers of standard childhood vaccines, sometimes combined with religious objections, has created pockets of vulnerable kids in the U.S. Fighting the misinformation can help, but the only way to ensure that outbreaks don’t return is to eradicate the virus from the globe.
Faye Flam is a Bloomberg Opinion columnist. She has written for the Philadelphia Inquirer, Economist, the New York Times, the Washington Post, Psychology Today, Science, and other publications. She has a degree in geophysics from the California Institute of Technology.