War with Iran is testing the U.S. military health system
We must reappraise the Military Health System to align with the Pentagon's goal to restore a “warrior ethos,” including integrating military medical teams into civilian health systems.
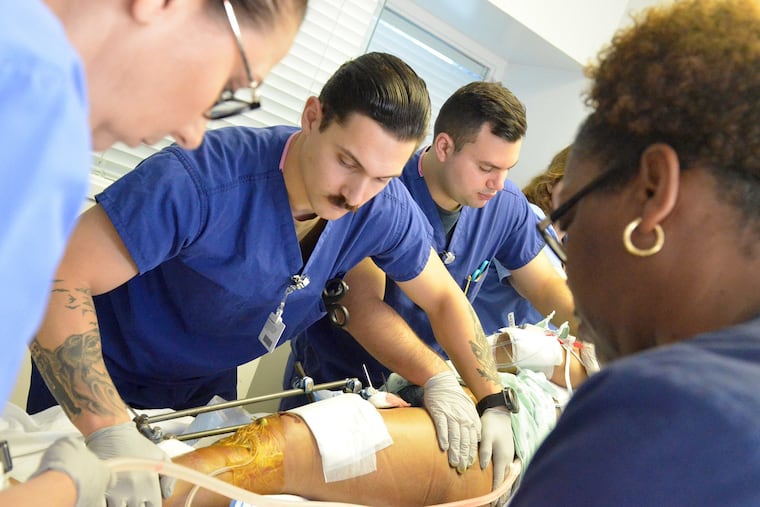
The United States has entered a war with Iran. And its Military Health System is ill-prepared for battle.
Aging facilities, empty operating rooms, eroding clinical readiness, and staffing shortages now strain a system that only recently set a global standard for combat casualty care. In a protracted, high‑intensity conflict, these weaknesses will directly impede our ability to sustain combat operations and to care for those in the fight.
The individual service member is often hailed as the most important weapon system in the American military arsenal — more important than tanks, aircraft, ships, missiles, or drones. Defense strategies once limited to the domains of land, sea, air, space, and cyber now increasingly recognize a sixth: the human domain.
Warrior ethos
This new domain emphasizes achieving peak performance, instilling mental resilience, and enabling quick recovery in our warfighters. These elements determine battlefield effectiveness — and align with the Pentagon’s emphasis on restoring a warrior ethos across the armed forces.
Within this framework, the Military Health System is more than just a support function. It represents a strategic capability that sustains the readiness, morale, and lethality of the armed forces.
Unlike earlier generations that relied on conscription, today’s service members all volunteer to serve, often knowing they may be called upon to undertake dangerous missions. At the core of the implicit agreement between our nation and those who volunteer lies this guarantee: If wounded, they will receive the best care modern medicine can provide.
During the wars in Iraq and Afghanistan, this agreement was largely fulfilled. Through a coordinated system of forward surgical teams, rapid patient evacuation, and specialized trauma care, the United States achieved historic success. Survival rates surpassed all previous conflicts, and casualties with even the most grievous injuries were restored to high levels of function. Central to this achievement was the military’s Joint Trauma System, which integrated battlefield care, clinical data, and continuous performance improvement across a global chain of combat casualty care.
Staffing shortages now strain a system that only recently set a global standard for combat casualty care.
These advances were driven by military surgeons, physicians, nurses, and medics who gained hard-earned experience treating large numbers of severely injured casualties during wartime deployments. Over the past two decades, insights from these experiences has also reshaped civilian medicine. Modern bleeding control, novel surgical techniques, and trauma system design have since transformed trauma care in civilian hospitals across the United States.
Yet these wartime successes often prove difficult to sustain in peace. Military medical leaders have long warned of the “peacetime effect,” a gradual erosion of vital trauma skills between major conflicts. Historically, this leads to a painful reality: Survival at the start of a new conflict fails to meet the standard set at the end of the last one.
Military planners, congressional leaders, and civilian advocates have all sounded the alarm — we have fallen prey to the peacetime effect. As one example, Walter Reed National Military Medical Center’s trauma center verification recently lapsed while debates over its role in the Maryland trauma system have continued.
Sharing expertise
To remedy this concerning trend, we must prioritize integrating military hospitals into civilian trauma systems where feasible and embedding military trauma teams in busy civilian trauma centers like Penn Medicine and the Mayo Clinic. Immersing our military medical personnel in high-volume, high-acuity, and high-complexity clinical settings will ensure we honor our commitment to every service member whenever or wherever they deploy.
Looking ahead, a protracted conflict with Iran and any future conflict with a peer enemy will severely strain our healthcare system. We must plan for high casualty volumes and contested evacuation routes in the face of a determined enemy. Preparing for these realities requires that we preserve the expertise in trauma care developed over the past two decades while adapting and improving our entire medical system — both military and civilian — to care for those who serve our nation.
The stakes extend well beyond battlefield medicine. Morale is a major beneficiary of outstanding medical care or an early casualty of substandard quality. Confidence in the Military Health System clearly influences recruiting, retention, and especially the willingness of service members to undertake dangerous missions.
Our warfighters go into battle knowing that, if injured, they will be cared for by a system committed to and capable of rescuing and restoring them to good health and a high level of function. That confidence bolsters morale and strengthens the bond between the nation and those who serve.
As the United States enters a new conflict, the strength of its Military Health System deserves renewed attention. Maintaining a world-class system capable of healing and restoring wounded service members represents more than a moral obligation — it’s a strategic necessity.
Todd E. Rasmussen is a professor of surgery at Mayo Clinic and a retired U.S. Air Force colonel. Jeremy W. Cannon is a professor of surgery at the University of Pennsylvania and a retired U.S. Air Force colonel. Both served multiple combat tours during the Global War on Terror and are past presidents of the Excelsior Surgical Society of the American College of Surgeons.

Inquirer Opinion Newsletter