Medical group takes aim against fires during surgery
An anesthesiologists society plans guidelines against the rare but increasing problem.
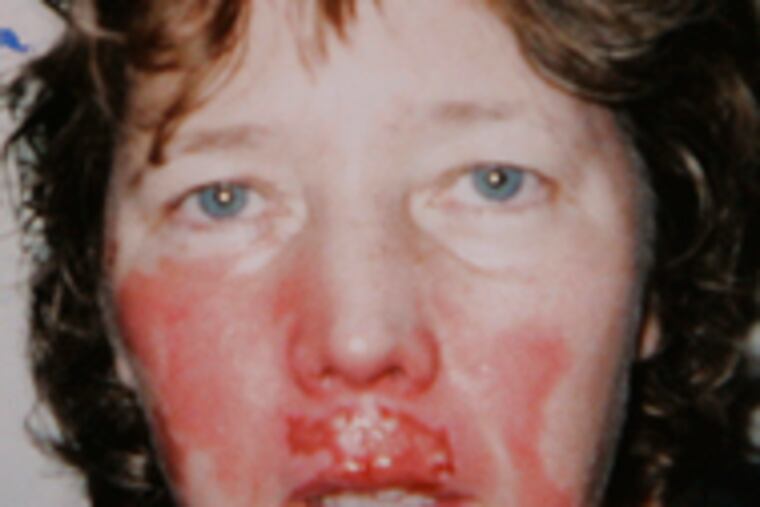
Flames engulfed Kathleen Osberger's face as she lay sedated on a Chicago operating-room table during what was supposed to be a simple procedure to remove two moles from her face.
Now, seven years and 18 corrective operations later, the 54-year-old clinical social worker is still on disability leave because of the severe burns to her upper lip, nose and nasal passages.
She says that doctors had never told her what they think went wrong but that she believed oxygen collected under surgical drapes and fed a fire sparked by surgical tools. She sued and settled with the hospital where she had the surgery, which denied negligence.
Surgery fires are rare but serious enough that the American Society of Anesthesiologists plans this fall to issue its first guidelines aimed at preventing them. Health officials are not required to report surgery fires, but the medical group says they have increased over the last two decades with the use of lasers and tools that use electric current.
"We think there is a lot of underreporting and a lot of near misses," said Jan Ehrenwerth, a professor at the Yale University School of Medicine and a member of the society's task force on the issue.
ECRI Institute, a nonprofit health research agency in Plymouth Meeting, estimates that there are 50 to 100 fires out of the more than 50 million operations performed in the United States each year. Such fires kill one to two people annually, and 20 percent of patients suffer serious, disfiguring injuries, according to ECRI, which investigates medical procedures and devices.
Most fires are caused when oxygen builds up under surgical drapes during the use of electric surgical tools that cut or remove tissue or control bleeding, the institute says.
ECRI's Mark Bruley said too many anesthesiologists were using 100 percent oxygen instead of only what the patient needed.
The proposed guidelines include lowering the concentration of oxygen given during surgery by diluting it with room air when surgical tools that could ignite a fire are in use. Other suggestions are to reconfigure drapes to minimize oxygen buildup and use suction devices to remove excess oxygen.
Ehrenwerth disputes suggestions that anesthesiologists are administering unnecessarily high concentrations of oxygen.
"We have to look at the patient and see what's safe for the patient," he said. "We don't want them to have decreased oxygen to their heart or their brain."
Richard Greco, a plastic surgeon in Savannah, Ga., had a patient catch fire in 1991 during an eyelid procedure.
"I was absolutely astonished that the fire occurred while I was doing everything I was trained to do," he said. "There was obviously a flaw in the system. People weren't considering the risk of fire."
He said patients can be kept stable with an oxygen levels of 30 or 40 percent during the use of electrosurgery tools.