Palliative care comes to the emergency department
When Joseph Morelli's medical history popped up on her computer screen early one Sunday this month, Meg Greene, a nurse case manager in Bryn Mawr Hospital's emergency department, immediately recognized that he might benefit from her specialty: palliative care.
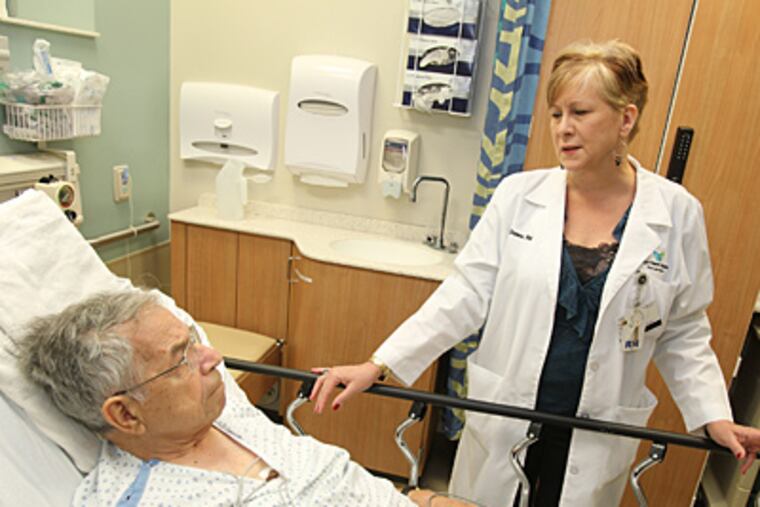
When Joseph Morelli's medical history popped up on her computer screen early one Sunday this month, Meg Greene, a nurse case manager in Bryn Mawr Hospital's emergency department, immediately recognized that he might benefit from her specialty: palliative care.
Greene is part of a small but growing group of medical providers who say many patients in emergency departments are not appropriate for the all-out rescue medicine these units are designed to deliver. Instead, they are suffering from the pain and inexorable decline of cancer and chronic illness or old age, and may be better served by care aimed at comfort, not cure.
Morelli, 88, had been in the hospital five times since March. The single-spaced list of his admissions in 2010 filled a full computer screen. He had chronic lung disease, and had been treated for bladder and prostate cancer. He had been in a nursing home since June.
That morning, the nursing home had called Morelli's wife of 60 years, Anna Marie, and told her he was in distress. Did she want him to go to the hospital? He had Do Not Resuscitate and Do Not Hospitalize instructions, but she said yes, in case this was a new problem.
By the time Greene met Anna Marie Morelli outside the emergency department, her husband had already been given intravenous fluids and antibiotics for sepsis, a blood infection. Orders had been sent to move him to a telemetry room, where he would be monitored by high-tech equipment and receive more antibiotics and fluids.
Anna Marie Morelli and Greene would decide whether he stayed on that path. It would probably make him well enough to return to the nursing home, but he would be back at Bryn Mawr soon for more of the same. The alternative was to focus on drugs that would help him breathe more easily - and let him die.
Palliative care, which focuses on treating the symptoms of diseases either fatal or curable, has become increasingly common in U.S. hospitals. According to the Center to Advance Palliative Care, the percentage of hospitals with palliative-care teams jumped from 24.5 percent in 2000 to 63 percent in 2009. But emergency departments are a new frontier for a specialty more commonly seen in intensive care or oncology units.
"I would say, over the last five years, the conversation and growth around palliative care in the emergency department has been exponential," said Tammie Quest, an Emory University doctor who is board-certified in emergency medicine and palliative care.
It is still rare for hospitals to have a staffer such as Greene who specializes in palliative care on-site in the emergency department. Mark Rosenberg, chairman of the emergency department at St. Joseph's Regional Medical Center in Paterson, N.J., said he was one of only 37 emergency physicians nationwide who were also board-certified in palliative care.
Several local hospitals, including Abington Memorial, Cooper University, and Thomas Jefferson University Hospitals and Albert Einstein Medical Center, said their palliative-care teams do consultations for emergency patients.
The National Institutes of Health has supported a program that teaches medical professionals ranging from doctors to chaplains how to train coworkers about palliative care in the emergency department.
The emergency department is a focal point because it is where most patients who are admitted start out and "the final common pathway of a broken system," said Diane Meier, director of the palliative-care center at Mount Sinai School of Medicine. By that, she means that many people go to the emergency department because they have not gotten good primary care or chronic-disease management.
Also, she and other experts said, many patients have not been told explicitly that they are dying, do not understand the symptoms of dying, or have caregivers who feel unable to handle those symptoms at home.
"A lot of the time, the problem is that no one has sat down and asked patients and families if they'd like to know what to expect," Meier said.
Rosenberg said he treated a woman with end-stage kidney disease who had chosen to quit dialysis. Yet her family called 911 when they found her unresponsive, and paramedics resuscitated her.
Many patients also have been given poor pain treatment. "Most doctors don't know how to manage pain," Meier said. "It's not taught in medical school. The general public finds this frankly unbelievable. . . . It's just unfortunately a fact."
Palliative care can be a tough sell - to other medical staff - in the emergency department.
"It's very difficult for physicians who are trained in saving lives to come to a point where they say, 'There's nothing I can do and it's time to stop,' because it's part of their culture to offer that help," Greene said. "It's part of who a lot of them are. They went into medicine to save lives."
But palliative-care advocates say most patients prefer to die at home and, given a choice, many opt for comfort care if it spares them what Meier calls the "brutal shuttle" between home and hospital.
Can it be financially good for a hospital to ask patients if they want less care? Advocates say it can. Many medical staffers are already so busy that they do not need patients who really should not be there. Insurers often pay by the episode and type of illness, so lots of machines and tests could just add to the cost. And the government and insurance companies are increasingly interested in efficiency, so hospitals that keep expenses down may have a competitive advantage.
Palliative-care experts say they do not think about the money. They help patients get what they want and need, letting them, as Rosenberg said, manage their death as they would manage their life.
"All I'm pushing is that we're honest with patients," he said. "We give them the information they desire. . . . Isn't it my job as a health-care professional to understand your goals and help you get there?"
Greene, who thinks that 20 percent to 30 percent of patients in emergency departments could benefit from palliative care, says her job is fostering relationships with families that lead to long-term loyalty. "Part of my philosophy is, these events in people's lives are monumental. They're the things that they'll remember for always," she said. "Making sure that families have a good transition is really important. Not only will they remember their family member that way, but it's also important for the hospital."
Greene started her conversation with Anna Marie Morelli that Sunday by asking about the white-haired man who lay in bed breathing oxygen-enriched air. She asked about the man, not his illness.
Greene learned that Joseph Morelli was a plumber who had lived in West Philadelphia. He was a former smoker, the survivor of a plane crash in Burma during World War II, the chaplain of his VFW group, the father of four children, and a lover of dirty jokes.
His wife, who was 85 and looked remarkably together and calm, had visited him at the nursing home every day. They talked. They fought - just as at home. She watched him suffer. She could see he was giving up.
"He's just been getting disgusted the last month," she said. "He's had it."
Anna Marie Morelli did not like the word hospice, but thought he would have liked the idea of palliative care.
"I would like to be kept comfortable for a bit," he had told her, "but if anything happens, I don't want that stuff on me."
Eventually, Anna Marie Morelli told Greene and the hospital doctor who would care for her husband that comfort was the goal. She preferred that her husband stay at the hospital, so he would go to a room on the sixth floor. The doctor ordered that the heart monitor be removed. The antibiotics and fluids would be stopped. Joseph Morelli would stay on oxygen and receive medicines to help his breathing and dry up secretions.
He died two days later.