Simulator training helps parents care for kids with complex needs
High-tech human simulators have been a fixture of training for doctors and nurses for years. Bayada Home Health Care is among those that are going a step further.
High-tech human simulators have been a fixture of training for doctors and nurses for years.
Bayada Home Health Care is among those that are going a step further.
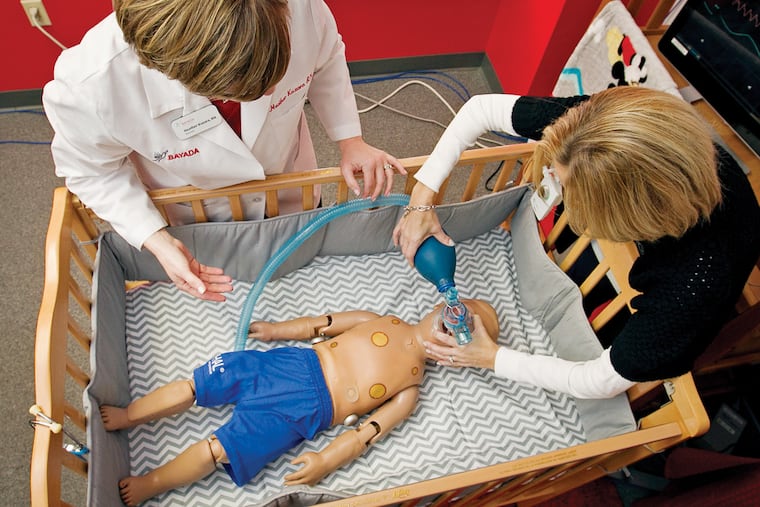
It is using childlike mannequins that simulate breathing and bowel sounds and can even turn blue during respiratory distress to train the parents of very sick or disabled children who need complex medical care at home.
A grant from Cure SMA (spinal muscular atrophy) allowed the home-care agency based in New Jersey to train 11 parents during the last half of 2015. Feedback was positive enough that Bayada now plans to expand the training program to about 100 other parents in 2016.
Though hospitals do teach parents about the care their children will need after they're discharged, those who must deal with ventilators, feeding tubes, and other medical equipment often still feel ill-prepared, said Michael Ward, a nurse who is Bayada's area director for pediatric simulation. Plus, needs change over time, particularly in children with progressive illnesses like SMA.
Two parents with years of caregiving experience recently went to Bayada's Mount Laurel office for training that would prepare them for emergencies. Both said they learned from the simulation.
"I wish that I was able to come in and do something like this when this first happened," said Stacy Tuttle, whose son Nikolas started having seizures at 3 months. Now 9, he has epilepsy with severe seizures and cannot talk or walk. Tuttle worries that he will stop breathing.
Her session with Heather Kuzara, director of pediatric-simulation operations for Bayada, helped her practice what to do if Nikolas, who has severe reflux, began vomiting during a seizure.
Kuzara introduced both mothers to what the $28,000 mannequin, meant to simulate an 18-month- to 2-year-old child, can do. There are multiple places to feel its pulse. The brown eyes can blink, and the pupils dilate or constrict. Its chest rises and falls with breathing. The skin around the mouth turns blue to simulate cyanosis. The simulator can make vomiting and gagging sounds. Kuzara can control all this with her computer.
She often manipulates medical scenarios from behind a screen so nurses or parents feel alone in the room as they would at home.
Bayada has 28 high- and medium-fidelity simulators now. The company, which operates in 22 states, plans to have them in all 70 of its pediatric offices within five years. It has also been using them to train nurses.
Erin White's 16-month-old daughter, Cameron, has a feeding tube and gets extra oxygen through a tracheotomy. The Greensboro, N.C., woman thinks she and her husband were well-trained by the hospital before Cameron could go home. However, White's parents are also caregivers for their grandchild, and they had not been trained before Bayada let them learn with the simulator. "For them," White said, "it was great."
She was impressed by all that the simulator could do. "It's a pretty incredible little dummy."
Tara Montague, who works for Bayada as a community liaison, shouldn't have needed much education. Her daughter Mary is 18 and has been on a ventilator almost since birth. Her SMA is progressing, and she now communicates with eye rolls and eyelid flutters.
Montague was obviously familiar with all the equipment she and Kuzara laid out in preparation for changing parts of the mannequin child's ventilator. It's a job that Montague can usually do at home without a hitch. Kuzara threw her some big simulated challenges, though. The change didn't work. The mannequin's blood oxygen saturation dropped precipitously. Montague had to pump oxygen manually into the mannequin's tracheostomy, a hole in the neck.
Montague kept her cool but admitted the whole thing made her anxious.
"That's the most traumatic trach change I've done in like forever," she said when it was over.
"Then I've done my job," Kuzara answered.
"The heart rate went up. My stomach dropped," Montague said. She told herself, "It's just a doll. It doesn't matter. Once the alarms start going off, I feel like I do when the alarms go off at home."
Kuzara, who lives in Charlotte, N.C., starts off much slower with parents new to caregiving. She teaches them how to use a stethoscope and listen for lung wheezing, a sign of constriction, and crackles, which signal too much fluid.
She has found that hospitals sometimes misjudge how well-prepared parents are or whether Mom or Dad has the cooler head. She has had nurses and parents freak out. That's a sign she needs to make the scenarios less intense.
Children's Hospital of Philadelphia also uses mannequins to teach parents how to do things like give enemas and care for tracheostomies, but it uses computerized simulators only to teach parents how to care for a child with a tracheostomy tube.
Nemours/Alfred A.I. duPont Hospital for Children in Wilmington will be using the more advanced simulators to teach families "in the very near future," said Maria Carmen Diaz, a pediatric emergency-medicine physician.
She became convinced that was a good idea after being asked to write a textbook chapter on pediatric simulation. Studies showed simulation training has led to improved technical skills and understanding about why caregivers should react in a certain way, she said.
Currently, parents are training on hospital equipment and, sometimes, with their own children, but that's no way to practice what to do when things go wrong.
"This is their opportunity to make mistakes," Diaz said of the simulators.
Though simulators are used to make staff extremely proficient, that's not necessarily the goal with parents.
"You may never get the mastery learning," Diaz said. "It may be fine that they recognize the seizure and call 911."
215-854-4944
@StaceyABurling