How doctors are reducing opioid use after surgery
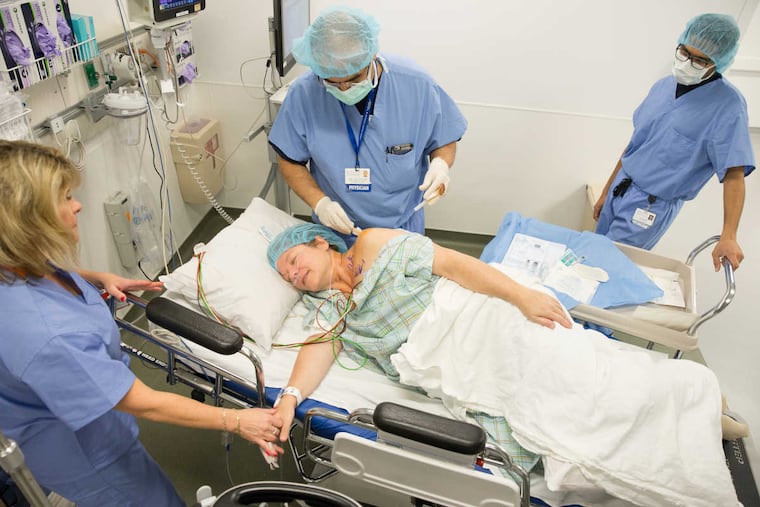
Well before orthopedic surgeon David Glaser made the first incision to repair Jenifer Zeller's torn rotator cuff, her medical team at Penn Medicine was working to reduce the number of opioid pills she would need when she went home a few hours later.
Opioid addiction is now a national crisis, and doctors worry that abuse too often begins when surgical patients are given prescriptions for large numbers of pain pills. Orthopedic teams are rethinking how they manage pain, often employing a cocktail of drugs designed to reduce pain and inflammation in the crucial first days after surgery. If patients can keep opioid use to a minimum then, the thinking goes, they'll use fewer of the pills in total and switch to less dangerous medications faster.
While waiting in the pre-op area, Zeller took doses of Tylenol and gabapentin, an anti-seizure drug also used for nerve pain, with a sip of water.
Just before surgery, anesthesiologist Nabil Elkassabany threaded a catheter the diameter of fishing line between nerves in Zeller's neck with the help of ultrasound imaging. The catheter would bathe the nerves around her shoulder with ropivacaine, a local anesthetic that would numb her arm so completely that she could stay awake during surgery if she wanted to. (She did, but only long enough to see just how badly her muscles were torn.)
Glaser would also inject some numbing medicine directly into the surgical site.
The catheter for the regional pain block went home to Rumson, N.J. with Zeller, keeping her shoulder and arm numb for 2½ days. She was instructed to take Tylenol, gabapentin, and ketorolac for the first few days.
She also got a prescription for low-dose oxycodone — an opioid — and was told she could take it if needed, but she didn't have to. For longer-term pain, she was to take over-the-counter drugs such as Tylenol or ibuprofen.
Two days after her surgery, Zeller's pain was well under control. The pump was still working and she had taken only a few of the 5 mg oxycodone pills. Her goal matched her doctors': to take as few opioids as possible. "My best friend died because she became addicted to this kind of stuff," said Zeller, 53, a home companion who was hurt during a fall in February. "I miss her every day, so this stuff scares the living daylights out of me."
Zeller's care was typical of a trend sweeping surgery: "multi-modal" pain control that de-emphasizes opioids. Orthopedic surgeon Richard Rothman, founder of Philadelphia's Rothman Institute, now also injects a combination of Marcaine, an anesthetic; ketorolac; and epinephrine, which controls bleeding, directly into the surgical site after he replaces a knee or hip. That "greatly improves" pain after surgery, he said. Lewis Kaplan, section chief for surgical critical care at Philadelphia's Michael J. Crescenz VA Medical Center, said intravenous Tylenol is commonly used during surgery at his hospital. Spinal-numbing agents are also helpful in abdominal surgery.
Using small doses of several medicines that work in different ways allows some surgical patients to avoid opioids altogether. Doctors are also prescribing fewer opioid pills at a time, so patients are not left with dozens of unused pills or given the idea they should finish all those Percocets as if they were antibiotics. Doctors are resetting expectations, telling patients how many pills most people need — not very many — and they are asking more questions when patients want to take opioids for weeks instead of days.
At the Philadelphia VA, all surgical patients meet with a pharmacist before picking up their medicines at the pharmacy and going home. Richard Bright, 66, of Ardmore, talked with pharmacist Andrew Rogalski after surgery to clean and repair blood vessels needed for dialysis. Bright had prescriptions for Tylenol and oxycodone. Rogalski told him he could break the oxycodone pills in halves or quarters. "Use only what you need, because the more you take, the more side effects you get," he said. He pointed out that Bright could put any unused pills in a drop box near the VA Center's police office.
Doctors are also talking about pain itself differently. Many pain experts now think it was a mistake to call pain a "vital sign" and lead patients to think they could avoid it entirely. That led to greater use of addictive medicines. Doctors now are more likely to tell patients to expect some pain, but also to expect that the worst of it will be gone within a few days.
Kaplan finds it helpful to talk to patients about how pain is affecting them, not whether they're having it. He has had multiple surgeries himself. "I wake up with a pain score of six," he said. "This is an acceptable pain score for me." If it reaches eight, he said, he takes a Tylenol. At nine, he soaks in a hot tub. His patients may not be that hard-core, but talking this way dramatically changes the discussion. "Your expectation will not be zero pain," he said.
When he was a resident in the early 1990s, patients whose colons were removed would go home with 45 to 60 oxycodone pills. Now they get about 15.
Eugene Viscusi, director of pain management at Thomas Jefferson University, said American surgeons are "generous" with opioids compared with doctors in the rest of the world. Elsewhere, he said, "you will not get a big bottle of opioids when you leave." Patients do fine with Tylenol and anti-inflammatory drugs such as ibuprofen or Alleve. "Their pain control is not inferior," he said.
Like other pain specialists, he said that some drugs are better than opioids for many kinds of pain. Patients should not think they're being "shortchanged" if doctors don't give them opioids. Some think over-the-counter medications are weak. "Most patients still want the good stuff," he said. "There's still this pro-opioid bias."
Ira Kirshenbaum, chair of orthopedic surgery at Bronx Lebanon Hospital, has encountered that reaction, too. "Some of this good stuff is other stuff," he tells patients.
His knee was replaced last year, and he took a total of three 10 mg oxycodones. "I saw firsthand. I was very well-controlled with anti-inflammatories and Tylenol," he said, "and I was not being a hero."
Over the last five or six years, many hospitals have begun making greater use of regional blocks such as the one Zeller got, both in surgery and after patients go home, Elkassabany said. Ed Mariano, an anesthesiologist based at the VA in Palo Alto, Calif., says he thinks the blocks, which reduce opioid use, and allow patients to sleep better and start physical therapy faster, have proven their value and should be used more often. Insurance coverage of home pumps, which cost about $400, is spotty, a problem he and Elkassabany say should be remedied.
"It is really important for hospitals to think much more broadly, beyond the cost of a pump," Mariano said. "For the cost of a readmission [for pain], you can buy a lot of pumps."
Elkassabany said that if he had shoulder surgery, he would want the nerve block at home for four or five days. "I'm not taking anything else," he said.
Zeller took oxycodone during the first six days after surgery, but was doing fine on Tylenol and gabapentin after that. Her biggest problem was boredom. She'd been ordered to keep injured arm completely still and was eager to get out and enjoy the spring weather.
