Opioids are the only way he can manage his cancer pain. Stigma creates more problems
Before opioids started being so widely prescribed for so many reasons, they were universally regarded as appropriate for the pain of cancer. But now, the "opioid epidemic" is a phrase that gets thrown at me, and I am certain other cancer patients, even by medical professionals.
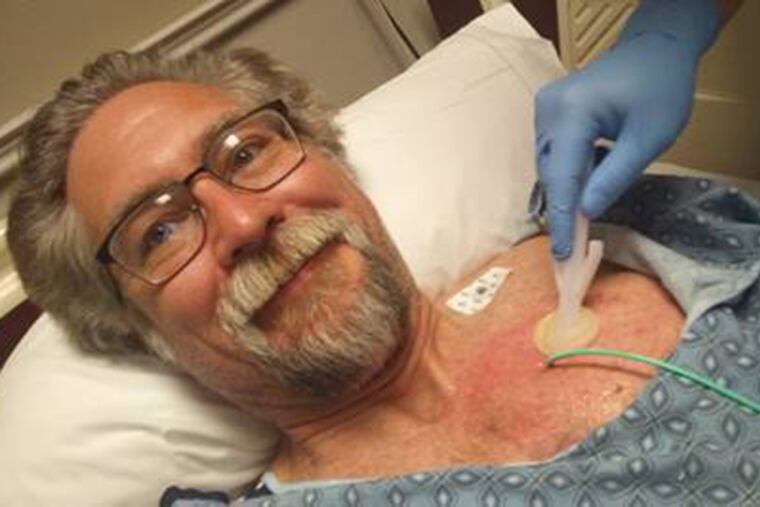
As a lung cancer patient since 2014, I am familiar with stigma. I have a disease many people assume is my fault.
And I have pain — a lot of pain — and other symptoms that can be managed in only one way: opioids.
Before opioids started being so widely prescribed for so many reasons, they were universally regarded as appropriate for the pain of cancer. But now, the "opioid epidemic" is a phrase that gets thrown at me, and I am certain other cancer patients, even by medical professionals.
If we are going to discuss epidemics at all, it is essential to look at the estimated 433 people who die every day as a result of lung cancer. That's more than 158,000 a year, compared with the 64,000 who died in 2016 from overdoses of all kinds of drugs.
Yet lung cancer is never called a crisis, patients are often marginalized, and research into lung-specific treatments receives a small fraction of overall cancer research funding.
Yes, there has been a huge amount of abuse and negligence with regard to over-prescribing these medications to patients who may not truly need them. But this can be said about drugs and doctors throughout modern history: There have always been those who abused the system, even when the vast majority do not.
>> READ MORE: Opioid prescribing guidelines frustrate cancer doctors as well as their patients
‘So unfair’
I have Stage IV adenocarcinoma, a disease with a historically poor prognosis. Yet chemotherapy worked well for me, keeping the cancer from spreading for more than 2½ years. By then, the science of cancer treatment offered fresh hope with targeted drugs.
To begin a new clinical trial last month, I was required to get a needle biopsy of the primary tumor growing in my left lung.
In the recovery room, a quick X-ray showed that the biopsy had gone as planned. But then I coughed.
Not just any cough, either. For nearly four months, I had been struggling with a reactive cough brought on by the progression of my cancer. The fits could be so violent that I might vomit, or be left panting for breath.
The only sure-fire way to deaden these coughs was using an opioid medicine. Opioids suppress respiration — deadly in an overdose, life-giving in a lung cancer patient with uncontrollable coughing.
One of these coughs struck about 10 minutes after my first post-procedure X-ray, before the tiny hole in the lining of my lung had completely healed up. Air was forced through that opening, filling a pocket of space in my chest cavity, causing a pneumothorax — putting me at imminent danger of a collapsed lung.
I asked for cough syrup containing codeine, and the fit soon subsided. I then had a new tube inserted into my chest wall with a balloon vent at the end to allow the air to dissipate faster. And I was admitted for further observation.
As the shifts changed, a new nurse came to get my details. I told her that I was in to get my lung cancer biopsied, but there was a pneumothorax. She stopped and asked the question:
"So, were you a smoker?"
The question was inappropriate. Smoking history makes no difference to a patient's medical path beyond factoring into what specific mutations to look for or what kind of drugs might be more effective. But I was so used to the question that I answered almost without thinking: "No, I never smoked."
"That's so unfair," came her response.
Her effort at sympathy just made me bristle. Would my cancer have been fair if I had been a smoker? Bladder cancer does not carry this stigma, even though it — like other cancers, heart disease, and other fatal conditions — is disproportionately linked to tobacco use.
She was the least of my problems that night. X-rays continued periodically showing slow improvement in my pneumothorax. I asked for more cough syrup, knowing that it wore off quickly. Cough syrup without codeine was delivered, and, with no alternative, I took it.
>>READ MORE: For these patients, opioids mean relief — and humiliation.
I also asked for a prescription for cough syrup with codeine to be called into my pharmacy, in case I needed it at home as I recovered.
Instead, to the confusion of my pharmacist, they called in an order for an over-the-counter medicine, Mucinex DM. No one had the courtesy to tell me they were not honoring my request for the only medicine that has controlled my violent coughing.
Jumping through hoops
Here's the irony: All my adult life, I avoided prescription painkillers. I dealt with chronic pain from sports injuries, a car accident, migraines, and cluster headaches using exercise, meditation, and as many non-medicinal means as possible, which mostly meant toughing it out.
Cancer is a whole new situation.
For the first couple of years after I was diagnosed at age 46, and I responded to chemotherapy, I dealt with my discomfort pretty well.
Then, in December 2017, came the excruciating pain in my back that left me barely able to walk, and unable to lie down for more than a minute or two.
An MRI showed that a new metastasis had formed in my back, pressing against the nerve. I stopped taking the cancer drug that clearly was not working, and got a prescription for hydromorphone. It was the first time in my life that I could say the pain was too strong for me to take.
But when I went to the pharmacy, I was devastated to discover that because it was a Schedule II narcotic, it would take another full day to get the prescription approved and filled. I got through the night with my last two Norco pills from an old rotator cuff injury, only to learn the next day the insurance company rejected my prescription. It would be days until my physician could appeal the decision.
I wept. Right there in the store, overwhelmed by pain I already was in, and the fear of even more to come. That weekend, while I was consumed by a constant urge to scream or cry, the cough grew more prominent, but I barely noticed it over the pain.
Once I began taking the hydromorphone at night, the cough stopped bothering me while I slept. Radiation therapy in February reduced the tumor pressing on my nerve and I stopped taking the opioids at night. Almost immediately, the cough was back.
After jumping through more hoops, I got the oxycodone my oncologist recommended to suppress my cough, and again could sleep.
But I still could not take the oxycodone with me to the hospital when I went in for that lung biopsy, and stayed overnight with the pneumothorax.
Recovery
After a night of my coughing at the hospital, the pulmonologist on duty called. I asked him why he didn't give me the cough syrup with codeine I requested.
As I might have heard, he explained, there is an opioid epidemic in this country, and he simply did not feel comfortable giving me codeine.
I told him that my cough was again heavy, and getting worse. He would not budge. Instead, he told me to go to the ER if my cough made the pneumothorax worse.
Fortunately, I still had enough oxycodone at home to keep the cough at bay while recovering from the pneumothorax. I have also been fortunate enough to get a new cocktail of drugs working on my cancer and symptoms, and these seem to have started off well enough.
My cough is almost completely gone, and I have not needed the opioids in nearly a week. But if I do need them, I am vastly relieved to know that they are available. And I shudder at the thought that someday they might not be.
Jeffrey E. Poehlmann is a writer and filmmaker based in Los Angeles. After a mass was discovered in an X-ray following his treatment for a torn rotator cuff, it took nearly three months to receive a final diagnosis. He began chemotherapy toward the end of 2014 and completed 40 rounds in August 2017. He is in a clinical trial for a targeted drug designed for a mutation that was not treatable four years ago. Read his blog at justbadforyou.com/blog, and his writing on LungCancer.net. This column appears through our partnership with Inspire, an Arlington, Va., company with condition-specific online support communities for more than a million patients and caregivers.