Health care lacking in Philadelphia's low-income areas
Philadelphia is well-known as medicine central, with one of the nation's highest concentrations of hospitals and specialists. But a new University of Pennsylvania study finds that in health care, as in so many other realms that intersect with economics, there are two Philadelphias.
Philadelphia is well-known as medicine central, with one of the nation's highest concentrations of hospitals and specialists.
But a new University of Pennsylvania study finds that in health care, as in so many other realms that intersect with economics, there are two Philadelphias.
In certain low-income neighborhoods, the Penn researchers counted close to 3,000 adults for every primary-care provider. That translates into some residents having to wait months for an appointment.
But in some sections of Center City, the ratio is below 300 adults for every provider - a tenfold difference.
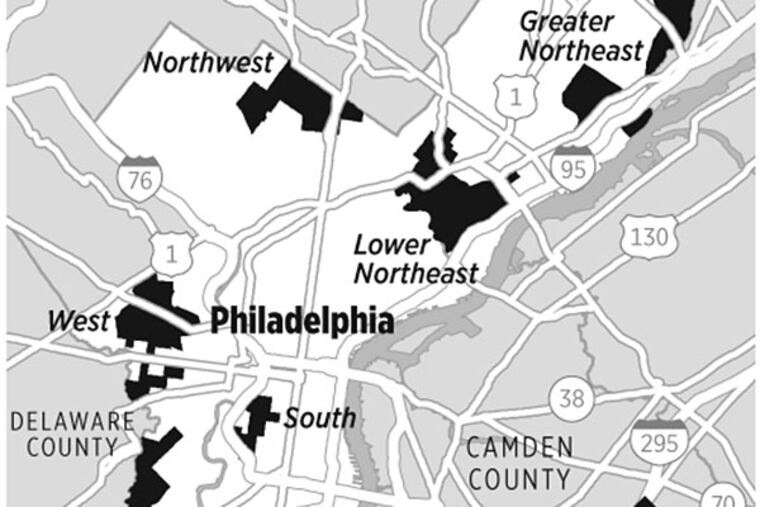
Primary-care deserts tend to occur in broad clusters, in Southwest, West, Northwest, Lower Northeast, Greater Northeast, and South Philadelphia/Grays Ferry, said the authors, of Penn's Leonard Davis Institute of Health Economics.
The researchers also estimated the number of primary-care providers who accept Medicaid, the government health insurance program for the poor, and found shortages in the same general regions of the city.
The researchers said that further study was needed but that their report, commissioned by the city Department of Public Health and funded by the nonprofit Independence Foundation, could serve as a guide when health-care systems and clinics make decisions about where to expand.
City Health Commissioner James W. Buehler agreed.
"What the real value of this report is, is that it provides a starting point for thinking about where is there a need for expanding primary care capacity," Buehler said.
The Lower Northeast was already well-known as a place that needs more primary-care doctors and nurse practitioners. At the city-run Health Center 10 on Cottman Avenue, new patients have to wait up to five months for an appointment, Buehler said.
Later this year, the city hopes to reconfigure existing space at the center to add exam rooms, he said.
Similar expansions are underway elsewhere as clinics prepare for an expected increase in patients, brought on by the expansion of the Medicaid program. The expansion is enabling more people to access health care - if they can find a provider. According to the U.S. Centers for Disease Control and Prevention, Medicaid beneficiaries on average use emergency rooms more frequently than other people do. Some researchers point to a lack of primary-care providers as one reason for people using emergency rooms.
The Family Practice and Counseling Network recently added six exam rooms at its clinic in Southwest Philadelphia, at South 61st Street and Woodland Avenue, allowing providers to take care of 3,000 more patients per year, up from 6,000, said executive director Donna Torrisi.
And they need every bit of that space, and every one of the nurse practitioners who see patients in it, she said. Going simply by the number of primary-care providers is misleading, as many lower-income patients have chronic diseases, mental illness, and other complex problems that require more personnel, she said.
"We're pretty flooded," Torrisi said. "It's not like seeing your upper-middle-class person with an upper respiratory infection."
A similar expansion is planned for a sister clinic in North Philadelphia that is operated in partnership with Drexel University, she said - provided they can find nurse practitioners to work there.
The federal government has a program to pay off the education loans for practitioners in such clinics, but once the loans are paid, some move on to more lucrative positions, she said.
The study suggests many community health clinics are in appropriate locations, in areas with lots of people who are on Medicaid, said the Penn study's lead author, Elizabeth J. Brown.
Some underserved areas, such as the Lower Northeast, have few clinics, but that does not mean existing clinics should be moved, said Brown, a family physician and also a research fellow funded by the Robert Wood Johnson Foundation.
"If we moved any one of those health centers, it may create a pocket that is underserved," Brown said. "It's just that we don't have enough. We shouldn't be taking away the health centers that are already there."
The researchers determined the number of primary-care providers - including physicians, nurse practitioners, and physician assistants - by comparing several data sets and following up with phone calls.
They then calculated a ratio of adult residents to providers within a five-minute drive of each census tract. The authors acknowledged that many residents would rely on public transit, and urged further study of whether clinics are accessible in that manner.
215-854-2430 @TomAvril1