Medical Mystery: A knee replacement and a major infection
Cultures taken around the knee didn't give up their secrets in the lab. Time for a novel technology.
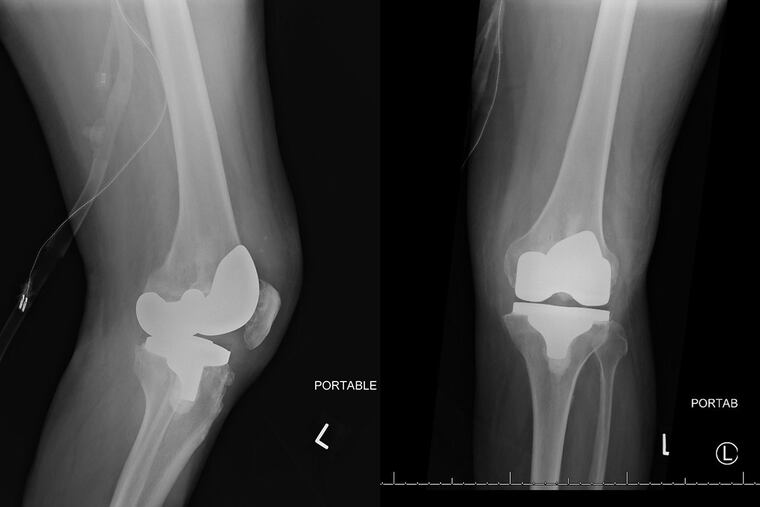
A 62-year-old man, who had a knee replacement three years earlier, developed signs of a serious illness, including fever and swelling in the knee.
When he got to Jefferson Hospital, his left knee — which had the joint replacement — was warm and red, and it was painful for him to bend and straighten it. By now, our patient was so ill that he had to be transferred to the intensive-care unit. Radiographs showed severe soft tissue swelling, though the implant was where it should be, and there was no evidence of it loosening.
Blood tests showed elevated markers of infection. The erythrocyte (red blood cell) sedimentation rate was higher than normal, and so was his C-reactive protein, also a sign of inflammation. A sample of knee joint fluid was promptly obtained by needle aspiration and examined in the laboratory. Under the microscope, we could see that his white blood cells were elevated, along with other signs of underlying infection.
The decision was made to take him into surgery so we could wash out the knee, and remove the joint replacement components. During the procedure, tissue samples were sent to the lab to try to identify what caused the knee infection, and the joint replacement was reimplanted.
But all efforts to find the organism were inconclusive. Culture results were all negative, even after 14 days of keeping them in the incubator.
The underlying cause was a real surprise and required the use of an innovative test.
Solution:
As part of a study we have undertaken, samples were also sent during the knee operation for a novel method of meta-genomic DNA analysis. This novel technology, known as Next-Generation Sequencing (produced by MicroGen Dx, based in Texas) is able to analyze all of the microbial DNA present within a sample. Antibiotic sensitivities can also be provided by the assay based on the presence of antibacterial resistance genes.
In this case, the analysis revealed Streptococcus canis, an oral pathogen found in the mouth of dogs and cats.
It was later discovered that the patient sustained a scratch from his pet dog a few days earlier, which was repeatedly licked by the dog. This had led to the knee infection.
Based on the sequencing results, we started more precise and targeted antibiotic treatment. Our patient made an excellent recovery, and was discharged from the hospital a few days later.
This case highlights the potential of this technology to isolate organisms. Traditional cultures fail to detect bacteria in up to half of implant infections, leading to guesswork in deciding on the appropriate treatment.
We coauthored a recently published study in which we found that the sequencing technology could identify infective organisms in almost 90 percent of cases vs. only 61 percent with culture. Furthermore, we could detect the pathogen in 81 percent of the cases that were negative for pathogens by the standard culture method, and which would have been missed otherwise.
Javad Parvizi is chairman of research and professor of orthopedic surgery at the Rothman Institute at Thomas Jefferson. Karan Goswami is a research fellow and doctoral candidate affiliated with the Rothman Institute.