The Biden administration lifts the barriers to prescribing buprenorphine to treat opioid addiction
New guidelines announced Tuesday mean doctors and other health workers will no longer need extra hours of training to prescribe the drug.
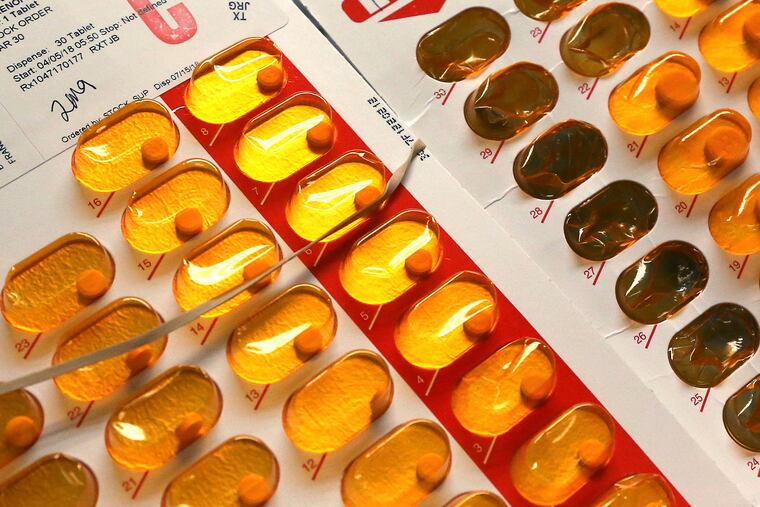
The Biden administration is easing decades-old requirements that made it difficult for doctors to treat opioid addiction using medication.
New guidelines announced Tuesday mean doctors and other health workers will no longer need extra hours of training to prescribe buprenorphine, a gold standard medicine that helps with cravings. And they no longer have to refer patients to counseling services.
Under the loosened guidelines, prescribers will be able to treat up to 30 patients at a time with the drug. It comes in a pill or film that dissolves under the tongue. It costs about $100 a month. A common version of buprenorphine is Suboxone.
Because of how opioids act on the brain, people dependent on them get sick if they stop using. Withdrawal can feel like a bad flu with cramping, sweating, anxiety and sleeplessness. Cravings for the drug can be so intense that relapse is common.
Buprenorphine helps by moving a patient from powerful painkillers or an illicit opioid like heroin to a regular dose of a legal opioid-based medication.
Besides doctors, nurse practitioners, physician assistants, certified nurse midwives and some other types of nurses will be able to prescribe buprenorphine without first getting special training.
The Trump administration tried to make a similar change in its final days but it would have applied only to doctors.
The Biden administration put the matter on hold for a legal and policy review, ultimately deciding to expand the easier guidelines to more prescribers.
“What it does is provide more on-ramps to treatment,” said Brendan Saloner, an addiction researcher at Johns Hopkins Bloomberg School of Public Health. “This will help in health centers, hospitals, jails and prisons — places where these folks sometimes show up for treatment.”
» READ MORE: Fatal overdoses among Black Philadelphians soared during the pandemic, new data show
Stricter requirements will remain for prescribers who want to treat more than 30 patients at a time.
The American Medical Association welcomed the change and urged Congress to remove other roadblocks to prescribing buprenorphine.
“Patients are struggling to find physicians who are authorized to prescribe buprenorphine; onerous regulations discourage physicians from being certified to prescribe it,” said Dr. Patrice Harris, who leads the AMA’s opioid task force, in a statement.
The prescribing requirements date back to legislation in 2000 meant to prevent too-easy access to a medicine with its own potential for misuse. But only a small number of doctors went through the steps and, in many parts of the country, patients couldn’t find a prescriber. Ironically, doctors could prescribe buprenorphine for pain without the extra training.
U.S. drug overdose deaths have climbed during the coronavirus pandemic. The Centers for Disease Control and Prevention reported 90,000 drug overdose deaths in the 12 months ending in September, the highest number ever recorded in a one-year period. There is not yet data for all of 2020, and the figures are preliminary.
The change “will increase the number of prescribers and the number of patients who receive prescriptions,” said Assistant Health Secretary Dr. Rachel Levine.