Medical mystery: Why did a healthy woman develop bleeding ulcers?
As soon as our patient mentioned her self-medicating, we cracked the case.
A 50-year-old woman went to the emergency department complaining of abdominal pain that had been getting worse for several weeks.
During her exam, she said the trouble started with a dull, aching pain in her upper belly, as well as nausea, right after eating. The pain lasted up to an hour afterward.
She visited her primary-care doctor. He suspected gallstones and ordered an ultrasound of her abdomen, which appeared normal. When her symptoms were no better, she went back to the doctor, who diagnosed her with gastroenteritis, an inflammation of the intestinal lining, most often caused by a virus. He told her that in time, her symptoms would resolve.
Her pain, however, worsened, progressing from an after-meal problem to an all-day misery. Her bowel movements appeared almost black. She felt lightheaded and weak for three days, and then realized she needed help right away.
In the ED, she had low blood pressure and a high heart rate. Her rectal exam showed her stool was black, a clear sign of blood. Laboratory tests revealed extremely low blood counts, a sign that she had been bleeding.
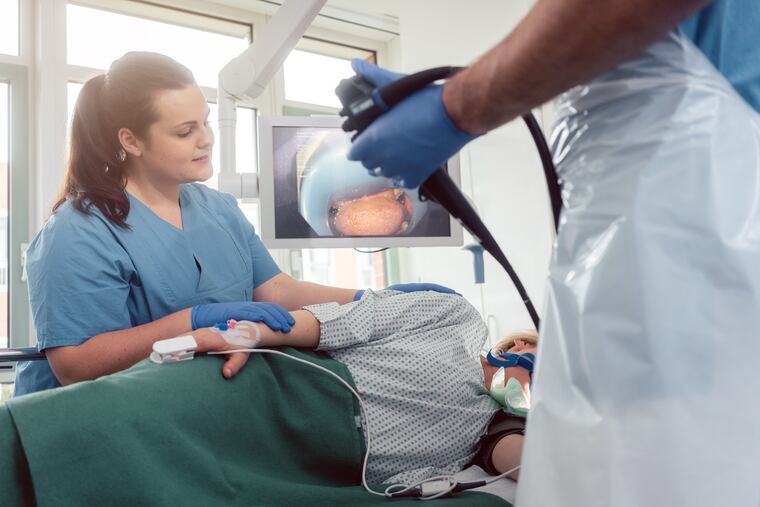
These additional clues led to the ED doctor’s summoning a gastrointestinal specialist to evaluate the patient. After she was given blood products and intravenous fluids, an endoscopy was performed to examine her digestive tract from the inside. Result: an actively spurting blood vessel inside an ulcer.
The diagnosis was made, but the bigger question was, why did she have an ulcer?
Solution
Before her gastrointestinal problems, the only health problem the patient reported was arthritis in her knees. Normally, she kept her pain in check with a daily ibuprofen tablet. But lately, we discovered, she was taking it as often as three times a day to keep up with increasing pain.
The mystery was solved.
Ibuprofen is a nonsteroidal anti-inflammatory drug (NSAID), one of the most widely used classes of medications. NSAIDs serve to improve inflammation, pain, and fever. Most of these medications are sold over the counter. You may know them as aspirin, Motrin, Aleve, or the generic ibuprofen, to name a few. They’re inexpensive too – you can get a bottle of 500 ibuprofen at Walmart for less than $8.
But just because these drugs are easy to get, it does not mean they are risk-free.
All NSAIDS inhibit the synthesis of prostaglandins, hormonelike substances involved in numerous functions, including contributing to the protective barrier in the mucosa of the stomach, and regulating blood flow to the kidneys and gastrointestinal tract. Lack of these prostaglandins coupled with ibuprofen pills irritating the GI tract lining leads to erosions and ulcerations, which can cause life-threatening bleeding.
Symptoms, usually abdominal pain and nausea, could mean so many different things, diagnosis often happens only after patients progress to vomiting or pooping blood. Additionally, because these are over-the-counter medicines, their use is underreported to doctors. Patients simply don’t think they count as serious medicine.
The consequences of excessive NSAIDS are well-known among medical providers, but we see so many cases!
So, what do we do?
In an ideal world, we would encourage elimination of all NSAIDs. But if that’s not a realistic goal, use the smallest effective dosage for the shortest possible time to minimize risks. Add acid-suppressing medications while taking NSAIDs to help guard against bleeding. Arthritis-strength Tylenol or topical NSAIDs like diclofenac may be safer alternatives.
Let your doctor know if you take any of these medications. Better yet, check first with your health-care provider before taking any medications.
Keerthi Shah is a gastrointestinal fellow at Temple University. You can follow her on Twitter at @KeerthiShahDO or Instagram at @Digestivedoc.