COVID-19 related deaths are rising. Do you know all of your life-saving options? | Expert Opinion
Physicians know ECMO can be a COVID-19 miracle. But we simultaneously wonder if simpler, low-tech solutions such as masks and social distancing could have prevented the need for life-saving equipment.
The phone rang for the fifth time that morning. The caller ID displayed a number we recognized as coming from a nearby hospital.
The attending physician briefly hesitated to pick up, knowing what the caller would be asking him.
Sure enough, the caller was a physician who had run out of options. He described a patient who was only 50 years old and a single mother of two young children. She was dying from COVID-19.
Earlier calls that day had been disturbingly similar. They portrayed the dire circumstances of a 58-year-old teacher, and a 62-year-old nurse. All three patients were rapidly dying despite having received every possible therapy available at their hospitals. All were on ventilators, all receiving maximum oxygen levels. They were not getting enough oxygen in their blood to stay alive and heal.
The 50-year-old woman’s physician, like the others, asked us whether we could provide the only remaining therapy to try to save his patient’s life: ECMO.
While most people who come down with COVID-19 recover with time, some develop symptoms severe enough to require being placed on a ventilator, in some cases for weeks to months.
However, for some, even the ventilator is not enough. These patients require a more aggressive degree of life support called ECMO, which stands for extracorporeal membrane oxygenation.
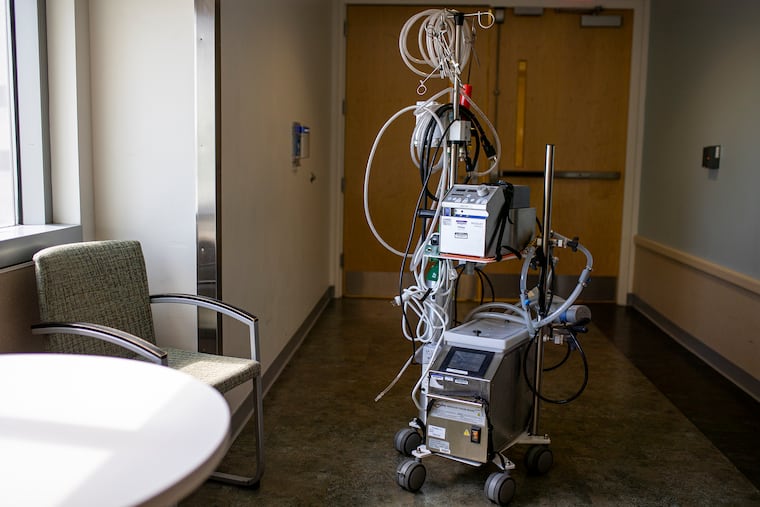
Similar to a heart-lung machine, ECMO is a pump that runs the patient’s blood through an artificial gas-exchange device before returning it to the patient’s body. It is a form of life-support that essentially takes on the work of the patient’s own heart and lungs until they are healed enough to function normally.
» READ MORE: When a ventilator is not enough, some COVID patients are placed on ECMO. It is far from a sure thing.
While the technology has existed since the late 20th century, ECMO began to be utilized more widely in 2009 during the H1N1 influenza pandemic. To date, more than 100,000 people who would have died from a wide array of cardiopulmonary diseases have been treated with ECMO. More than half of these patients have recovered.
During the COVID-19 pandemic, ECMO has been used to treat more than 3,000 patients worldwide. But it is by no means a certain lifesaver. According to a recent study reported in Lancet, fewer than one in three of these patients survived and was discharged from the hospital.
Sometimes, physicians are thought too fond of high-tech interventions. We know ECMO can be almost a miracle.
But every time our phone rings, we simultaneously wonder whether far simpler, low-tech solutions such as masks and social distancing could have prevented this call.
As COVID-19 surge continues, so, too, will awareness of potential life-saving therapies.
This list includes anti-inflammatory medications, such as steroids, as well as more invasive tools such as ventilators and even ECMO. It is unfortunately no longer an ultra-rare intervention that most people will never encounter.
Successful use of ECMO requires nuance, expertise, open communication and, at times, luck. Its intricacies can take years, if not decades, to learn. But since so many have become too sick too quickly, we know there’s more interest in ECMO than ever before.
The first thing we wish people knew is this: As sophisticated a medical tool as ECMO is, it should never be viewed as a panacea. Due to its highly invasive nature, its potential to harm can be just as significant as its potential to heal.
For as long as patients are on ECMO, which can be months, they generally need to be in a medically induced coma and cannot move. They also have increased risks of having infections, strokes, and other bleeding- or clotting-related complications.
Second, that’s why patient selection is of utmost importance. Not everyone who is desperately ill can be helped by ECMO. That is because while ECMO can keep people alive, it does not cure the underlying disease, in this case, COVID-19.
For patients too sick to recover and get off ECMO, this amazing technology becomes a “bridge to nowhere,” a state where one is artificially kept from death without any hope of recovery.
Given what a scarce resource ECMO is, it is crucial for experienced providers to make the tough choice of who gets an opportunity to even try it.
Yet as the pandemic keeps soaring and our phone keeps ringing, that’s exactly the kind of life-or-death-decision we are facing at a scale that medicine has never seen before.
As physicians, we can only hope to offer our best efforts with humility, knowing we may fall short at times.
Jason Han is a cardiac surgery resident in Philadelphia. Jacob Gutsche is the director of the lung rescue (ECMO) program at Penn Medicine.