The pandemic saw an exodus of health-care workers. Here’s how to win them back. | Expert Opinion
After 18 months on the front lines of the fight against COVID-19, hospital workers have become exhausted and cynical. They are showing their frustration by quitting in large numbers.
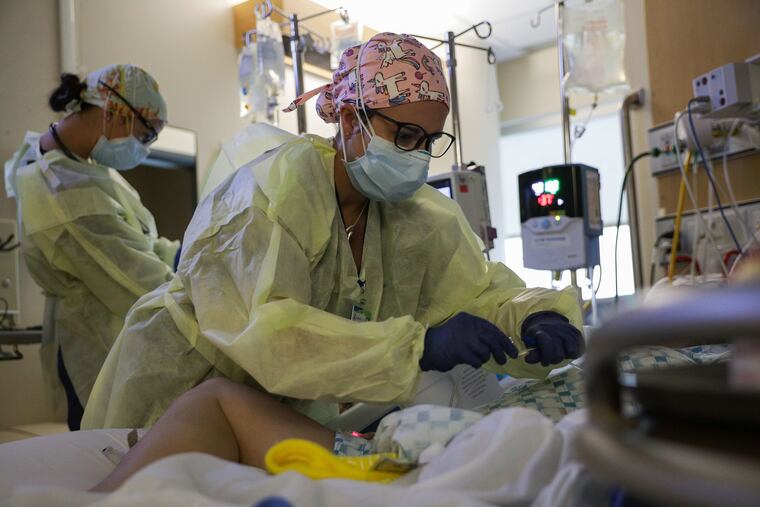
After 18 months on the front lines of the fight against COVID-19, hospital workers have become exhausted and cynical. They are showing their frustration by quitting in large numbers. This is especially true of nurses. A clear crisis of burnout is upon us. But there are ways to mitigate this crisis. Here’s how to win back health-care workers:
Create a plan
The COVID-19 pandemic laid bare the fact that we have an inadequate plan for responding to medical disasters at the federal, state, county, city, and hospital levels. The federal government futilely scrambled to increase the supplies of lifesaving masks and ventilators. Individual states faced varying degrees of health-care worker shortage: Doctors and nurses were in short supply in some areas, but in other areas they stood idle.
Crisis response at every level of government needs to be clearly outlined. What is the plan for another respiratory disease crisis? What other medical crises are possible, and what plans are in place to address them? These comprehensive preparations should be described to all hospital staff on a yearly basis to send a clear message to front-line workers that we are ready and that we have their back.
Address inequality
Health-care workers have been significantly affected by the extreme racial and economic inequality endured by patients who contracted, suffered with, and died from COVID-19. We like to think that everybody should have similar access to basic life-sustaining resources and care. But the pandemic exposed the raw inequality that exists in the United States.
Black Americans were almost four times more likely than whites to die from COVID-19. Black and Hispanic Americans were more likely than whites to both contract and be hospitalized with the disease. This sharp disparity in health outcomes is not new, but I hope the pandemic’s lessons will inspire us to enhance equality in health insurance, health outcomes, and health-care access, especially at the primary care level. This will need to happen at the federal level with the cooperation of the states, the government being vested with the power and the money needed to effect appropriate change.
Staffing shortages
A nursing shortage had been going on for a decade, but its extent has been accentuated by the pandemic. During the most recent wave of the virus’ spread, hospitals facing nurse shortages began eliminating beds and refusing surgeries. There are 6,000 nursing vacancies in Louisiana today, and there are 2,000 fewer nurses in Mississippi today than at the start of 2021.
A 2019 public opinion poll by the Association of American Medical Colleges revealed that 35% of people had difficulty finding a doctor, up 10 percentage points from 2015.
Doctors are also often tied to a single state due to licensing, hampering their ability to see telemedicine patients and to respond to a crisis. We need to establish a plan to use telemedicine more effectively. We also must suspend state-level restrictions on medical practice during pandemics. Perhaps most important, we need to graduate more nurses, and we need to value them more.
Limits of medicine
COVID-19′s rapid virulence also has made it clear that we need to better understand the limits of medicine and what the human body can and should endure. In a 1957 declaration, Pope Pius XII makes a very important distinction between ordinary and extraordinary measures. Ordinary measures include bandaging a cut or taking an antibiotic for pneumonia. Extraordinary measures include being placed on a ventilator or undergoing experimental chemotherapy. These extraordinary interventions place a tremendous burden on the patient, often with only vague assurances of success.
In his address, Pope Pius XII stated that there is no spiritual obligation to undergo extraordinary measures if they are fruitless. Understanding this distinction and having each patient define in a living will a level of comfort with extraordinary measures would go a long way to relieve a patient’s end-of-life burdens, often thrust upon caregivers and hospital staff. Discussions of end-of-life care, although difficult, should take place with family or close friends — and with your primary care physician at least once a year.
Kindness first
This final recommendation is the least concrete, but perhaps the most important. Recently, there appears to be a general decline in civility in hospitals. We need to focus on kindness and hope when interacting with caregivers in the hospital. Medicine is an imperfect science, practiced by people, who we know to be imperfect. There are too many stories today of doctors — and nurses — facing abuse. Doctors often hear, “You are treating my relative like a guinea pig,” or “You are ignoring my mother and not giving her good care.” For nurses, physical abuse is common.
Understand that health-care workers have dedicated their lives to a giving profession. Your struggle is our struggle. When we go home at the end of the day, we judge ourselves according to how much healing we were able to effect. Consider the hospital for what it is: a place where healing should occur in a collaborative and organized way.
Michael J. Stephen is an associate professor of medicine at Thomas Jefferson University and head of the Adult Cystic Fibrosis center. He is also the author of the recently published book “Breath Taking: The Power, Fragility and Future of Our Extraordinary Lungs.”