The fix for foot pain could be a surgery you didn’t know about
Foot problems are among the most common complaints of middle and older age. And they are not trivial. When people’s feet hurt, they’re less likely to exercise and more likely to fall, doctors say.
Brian Adams was born with very flat feet.
They didn’t stop him from playing a variety of sports — volleyball, baseball, basketball — in his youth. He grew to be a 6-foot-3-inch man who loved to “run, not jog.” Those flat feet served him well.
Until they didn't.
In the last few years, Adams, now 50, started having shin splints. The odd out-toed positioning of his feet compressed a nerve in his leg. “It felt like a burning poker behind my left ankle,” said Adams, a state property management specialist who lives in Edgewater Park, N.J. The pain grew so intense that he started dragging his foot “like Igor.” Neither a special orthopedic boot nor physical therapy helped. His knees started hurting, too. The inside of his foot was numb.
“I was worried that this one issue was going to disrupt the balance and structure of everything,” Adams said. “I thought I was just doomed, to be honest with you.”
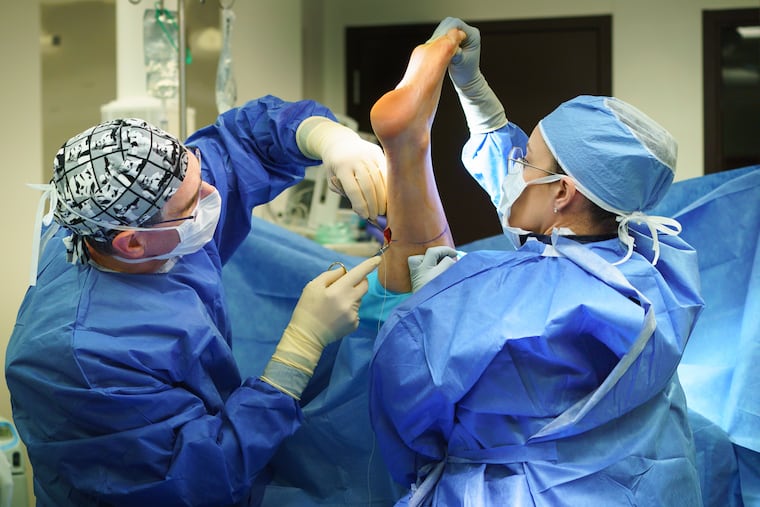
But he wasn’t, Steven Raikin, director of the foot and ankle service at Rothman Orthopaedic Institute, told him. That is how Adams ended up in an operating room in Bensalem recently, his bare left foot held high in the air as Raikin prepared to surgically repair its fallen arch. Like many people, Adams had not even known that the procedure existed.
It would not be easy. Raikin would make multiple incisions and then cut, hammer, saw and sew the foot into a more normal shape. Full recovery will take a year, but Raikin said most patients wind up with about 80 percent of normal function, far better than they had before surgery.
Foot problems are among the most common complaints of middle and older age. They are not trivial. When people’s feet hurt, they are less likely to exercise and more likely to fall, doctors said. About a third of people over 65 have foot pain, stiffness or aches. Almost everyone will have it at some point.
“It’s incredibly prevalent,” said Casey Jo Humbyrd, chief of the foot and ankle division at Johns Hopkins Medical Center and head of health policy for the American Orthopaedic Foot and Ankle Society. It’s harder, she said, to find older people who don’t have foot problems.
‘You should only be having surgery for pain’
Many of us take our feet for granted, but we quickly learn how much they matter when they hurt. Surgeons, Raikin said, often tell patients, “You take 10,000 steps a day and you never think about your feet until they hurt. Then that’s all you think about.”
Later-life problems with bones and tendons stem from a combination of unfortunate genes, wear and tear, old injuries, and more controllable risk factors such as obesity and diabetes. Women who cram their feet into too-small, too-pointy, too-tall shoes may pay for their fashion consciousness with bunions, hammer toes, and arch problems.
Though they can happen at any time, the deformities become more common as people reach their 50s and increase from there. You just have to live with some conditions, such as thinning fat pads on the ball of the foot and the heel. The pain from others can be controlled with orthotics, physical therapy, and better-fitting, lower-heeled shoes with arch support.
When none of those work, surgery is a last-resort fix for several of the most common complaints: flat feet, bunions, arthritis, and hammer toes.
Surgeons said the test for whether you should go under the knife is never how your feet look. “You should only be having surgery for pain,” Humbyrd said.
The foot is made up of 28 bones that are supported and moved by multiple muscles, tendons and ligaments. They absorb three to five times more force than the hips, Raikin said, one reason they are stressed by extra body weight.
You might expect that the arch of the foot is a hard structure like a bridge, but the primary support is ligaments that, over time, can become stretched or torn.
“I tell patients it’s like a rubber band,” Raikin said. “Once a rubber band has been in the sun too long and lost its elasticity, it can never get its elasticity back.”
Older patients also often have severe arthritis in joints that affect the arch. Every foot is different, and repairs involve a tapas menu of small steps that may replace and reroute tendons, free constricted muscles and nerves, realign the heel and, in the case of arthritis, fuse painful joints. Each patient may need a different combination of four to six surgical steps, said Kate O’Connor, a Penn Medicine orthopedic surgeon.
To watch short videos of a surgeon explaining the biomechanics of flat feet, bunions, arthritic ankles and hammertoes and surgery to repair them, click on the arrow below.
The surgery begins
In Adams’ case, Raikin began by releasing the calf muscle. It had been compressing the tibial nerve, causing the foot numbness.
Compared with orthopedic surgeons who replace big joints such as hips and knees, he used more delicate tools, a small scalpel, and long-handled tweezers. He made two more incisions along the side and back of the foot. He found the posterior tibial tendon, which runs underneath the arch. It was about twice the normal size -- bloated and riddled with tears.
Raikin explained that the tendon enlarged as it tried, futilely in this case, to heal itself. He cut away about 2¼ inches of the damaged tendon. He pointed out a yellow, Y-shaped structure, a nerve that had been compressed by the awkward position of the foot, which tends to roll outward when feet are flat.
He cut away bands of tissue that were constricting it. Then he pulled out the flexor digitorum longus, a tendon that normally moves the toes. This one was healthy. It was stretchier, thinner and shinier than the one Raikin had removed. He would reroute it to take the place of the damaged tendon.
Tendons, he said, travel on specific tracks, like trains. He moved this one from the toe track to the arch track. Other tendons would allow Adams to keep moving his toes but not as well as before. He pulled the tendon until an arch formed — “Right now, that’s a normal arch,” he said — and attached it to a bone with a special screw.
Raikin was not done. In severe flat footedness, the heel bone tilts outward “like a banana falling on its side.” Fixing that required yet another incision. Then Raikin inserted a slim, rectangular saw blade that cut the 1.5-inch heel bone in half laterally. He shifted the back piece half inward about 3/8 inch and screwed the two pieces together with a long, titanium screw. He sawed off some extra bone and tamped the heel in place with a hammer.
He pressed the foot against a clear piece of plastic to make sure the arch on the inside looked right. It did. It was noticeably thinner and more shapely.
In less than an hour, Raikin was done. Next it would be Adams’ turn to work, but first he would have to go home and do nothing for two weeks.
Help for other common foot problems
Surgical procedures are also available to help people with unremitting pain from bunions, arthritic joints, and hammer toes.
Hammer toes, which generally affect the second, third and fourth toes, become more common from the 50s on. Toes get locked in a bent position that is painful in shoes. Surgeons release the locked joint and pin or fuse it straight.
Arthritis can affect any of the 33 joints in the foot and ankle. Ankle replacement surgery is growing in popularity, but patients should know that replacement parts don’t last forever, O’Connor said. Some may prefer fusion surgery, which affects mobility but lasts longer than artificial joints.
In the big toe, another common arthritis site, doctors can now replace damaged cartilage with a cushion that preserves toe movement. Fusion is an option there, too, and it is the most common solution for pain in other joints, O’Connor said. The pain comes from the bones rubbing against each other. That stops when they are fused.
Fixing bunions is a bigger deal — requiring longer recovery time — than many people realize. Bunions look like a growth on the inner edge of the front of the foot, but they actually are a malformed joint.
Some combination of genetics and too-tight shoes makes the big toe migrate toward the outer edge of the foot. This puts pressure on the metatarsophalangeal joint — the place where the toe joins the foot — and makes it bow outward. To fix the bunion, surgeons cut and realign bones leading to the big toe. Many people with bunions also have hammer toes.
A year of recovery
Recovery takes time, no matter what the surgeon has done. After arch repair, patients such as Adams are told to stay still with the leg elevated most of the time for two weeks. “For the first two weeks, I tell patients they’re going to jail,” Raikin said. “They’re pretty much going home and doing nothing.”
As Adams soon learned, that’s boring. But he was pleased to learn that his foot, which was in a cast, was no longer numb. He had pain, but wasn’t complaining about it. So far, there’s no need for surgery in the other foot.
He would start physical therapy at about six weeks. One goal is to teach the transferred tendon its new job. “It’s a whole new tendon reeducation program,” Raikin said.
It will be a long road to recovery. Patients, the surgeon said, “have different types of pain on and off for a year.”
