HPV vaccine effective in reducing strains of the virus over 10 years
A new study confirms the why teens should receive the HPV vaccine.
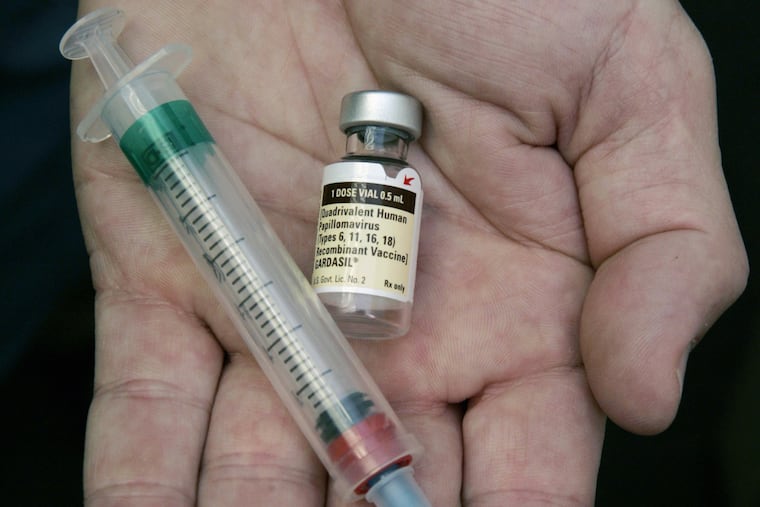
The old adage “An apple a day keeps the doctor away” could be changed to “A vaccine TODAY, can help keep cancer away” when it comes to new findings about the effectiveness of the Human Papillomavirus (HPV) vaccine.
A study in Pediatrics released online today found the HPV vaccine reduced strains of the virus and prevented its spread over a 10 year period. Young women 13 to 26 years of age were recruited from hospital-based and community health clinics for four studies, 1580 participants in total, from 2006 to 2017.
The promising results indicated that since the introduction of the HPV 4-valent and HPV 9-valent vaccines (4-types and 9-types of HPV respectively), there has been a significant decrease in the various covered strains infection rates. Also, prevalence of these same types of HPV have also decreased in women who were not vaccinated. More specifically, the HPV-4 vaccine showed a decrease of 80 percent in various strains for the vaccinated, and prevalence of these same types of HPV also decreased by 40 percent in women who were not vaccinated—implying a herd immunity.
In other words, as others are becoming vaccinated, the amount of circulating disease decreases, allowing non-vaccinated people to have a lower chance of being exposed to the disease. Estimated HPV-4 vaccine effectiveness was 90 percent the third study from 2013-2014 and 80 percent in the fourth study from 2016-2017. Researchers said further study is needed on the HPV 9-valent vaccine once there are higher rates of vaccination.
So why should we care?
HPV is the most common sexually transmitted infection in the United States and around the world.
Once infected with HPV the virus can lead to genital warts and various types of cancers in the cervix, other reproductive organs, head, neck, and anal regions.
Annually, 300,000 women die of cervical cancer caused by HPV.
Therefore, if you receive the vaccine, which has been shown to decrease infection rates, you are improving your chances of not becoming infected. In turn, decreasing your chance of developing the genital warts or cancers associated with it!
With all this in mind, some may ask “Should my child receive this vaccine?” The short answer is YES. However, it is natural to have a few questions and concerns about any type of vaccine. Below are a few common questions and answers to help explain the need for this vaccine:
Can you contract HPV from the vaccine? No. The vaccine is make from a surface protein from the virus. This in no way can infect the person with the actual virus. It is just enough to allow your body to make an immunity to the disease.
What are the most common side effects of the vaccine? The most common side effects of the vaccine are redness and tenderness where you were injected. A slight fever can also occur.
Who is recommended to receive the vaccine? Both males and females can receive the vaccine between ages 9 and 26, with the recommended initial vaccination occurring between ages 11 and 12.
What if I need more information before I decide to give the vaccine? A lot of information is published concerning vaccines, and HPV particularly. The CDC and Children’s Hospital of Philadelphia have wonderful resources for both parents and clinicians.
Very few vaccines have been proven to decrease your risk of certain cancers. Luckily, this is one of them. Have a conversation with your healthcare provider concerning the HPV vaccine so you can make an informed decision and have you and your family benefit from these advances.