What it takes to get patients over 65 through surgery
Geriatricians are helping older patients thrive after surgery. Age is less important than how well people are functioning.
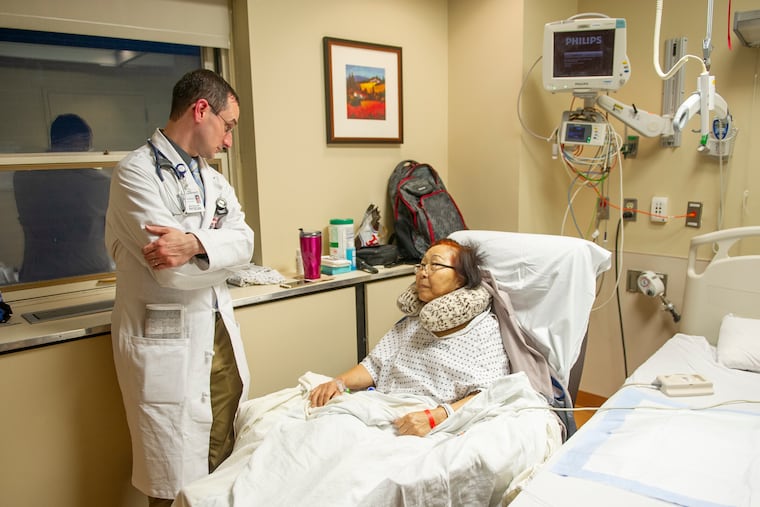
For months, Ann Chun, a 75-year-old retired casino game dealer from Galloway, N.J., had a horribly painful infection in her knee.
Last month, she wound up at Penn Presbyterian Medical Center, where a new member of the orthopedic trauma team made sure Chun, who needed surgery for her infection, got the kind of special attention that helps prevent major complications among seniors. Geriatrician Mark Simone specializes in helping patients whose age puts them at higher risk for delirium and a host of other postsurgical problems that can reduce quality of life and increase overall costs.
Teams where geriatricians work with surgeons and anesthesiologists to “co-manage” older patients are still unusual, but the trend is growing along with the recognition that the elderly are not, as one expert put it, just more “wrinkled 45-year-olds.” They need different care than younger patients, such as closer attention to nutrition, hydration, pain control, vision and hearing problems, vital-organ functioning, and mental orientation. This is especially true of patients in their 80s and above, but even younger seniors like Chun don’t bounce back from injury or illness the way they would have in midlife.
Getting older patients up and moving soon after surgery is especially important. "The muscle wasting and deconditioning can happen much more quickly in an older person, even someone in their 60s and 70s, than when they were in their 20s,” Simone said.
Figuring out how to provide better surgical care for the elderly is taking on more urgency as the vast baby-boom generation ages. While people over age 65 make up 15 percent of the population, they represent a third of surgical patients. Many people are living longer, more vigorous lives. They want more aggressive care and can do well with surgery if managed properly.
Others have multiple chronic illnesses and can falter without care attuned to their diminished reserves. Increasingly, doctors talk to such patients and their families about what they hope surgery will accomplish. For some, the risks of cognitive problems or lingering disability are too high. “Just because we can do things doesn’t mean we should do things,” said Lisa Walke, Penn’s chair of geriatrics.
Meanwhile, insurers are paying for surgery in “value-based” ways that reward hospitals for efficient stays without complications or readmissions. That’s an incentive to think about care of the elderly in a more global way.
Carrie Sims, a trauma surgeon at Penn Presbyterian, said Simone’s involvement with the surgical team has been valuable. “He raises a lot of really important issues that we might not think about,” she said. He has more time to dive deeply into medical histories, so he has a better idea of patients’ baselines before their injuries. He also tends to initiate conversations about patient goals faster than the surgeons.
Sims said Simone suggested taking an elderly patient off an anti-diarrheal medicine that contains atropine because it can make delirium worse. Sims, who had not had trouble with the medication with younger patients, was skeptical. “Sure enough,” she said, “it actually significantly improved her delirium.”
Walke is now working to include geriatricians in pre- and postsurgical care for older elective-surgery patients, not just those with emergencies. Health systems like Duke University’s are already doing that and have made “pre-habilitation” a priority.
Making sure elderly patients are eating enough protein and getting some exercise before surgery, even if it’s only for a couple of weeks, can make a difference in how well they heal, said Shelley McDonald, a geriatrician who runs the eight-year-old surgical co-management program at Duke that sees about 500 patients a year.
Orlando Kirton, chair of surgery at Abington Hospital-Jefferson Health, hopes to make geriatric pre-hab part of his program later this year. The American Society of Anesthesiologists launched its Perioperative Brain Health Initiative for seniors in 2015. The John A. Hartford Foundation and the American College of Surgeons have been working to create geriatric surgery guidelines that take the physical, cognitive, emotional, and social needs of seniors into account. After being piloted in seven health systems, those standards, which encourage pre-surgical cognitive testing, are ready to roll out nationally in June, said Marcus Escobedo, senior program officer for the foundation.
"There are pockets of excellence around the country," he said. "It's not widespread yet."
Many doctors have assumed they already know how to take care of older patients because so many of their patients are over 65. The data, he said, told another story.
What studies show is that surgical teams that include geriatricians in hip-fracture care have lower mortality, plus fewer complications and readmissions, lower delirium and infection rates, and lower costs, said Daniel Mendelson, co-director of the geriatric fracture center at Highland Hospital in Rochester, N.Y. A common feature of such programs — asking patients what they hope surgery will achieve — also leads to a small percentage (about 8 percent at Duke) deciding that surgery is not for them.
Simone, who started at Penn in January, paid special attention to Chun’s vital signs since the margin for error is smaller in older bodies. When he met her, she was having trouble with simple thinking tests, so he lowered her pain-medicine dose. Chun also has diabetes, and wasn’t eating much in the hospital. Simone lowered her insulin dose, as too much can lead to confusion and even coma. He adjusted her intravenous fluids when her kidney function worsened.
How patients are functioning matters more than chronological age
Newer practices and procedures have improved surgical outcomes for older people in recent years. Now there is an added emphasis on what their lives will be like after surgery. To predict that, chronological age matters less than how healthy and independent people are. “Function trumps everything for older operative patients,” Walke said.
Patients who already have signs of cognitive decline have a much higher risk of developing delirium, a form of mental confusion that is associated with longer, tougher recovery. Frailty, a set of problems that can include muscle weakness, fatigue, and unintentional weight loss, is another red flag, no matter the age. But even an 85-year-old who is playing tennis and chess is vulnerable.
“In an emergency situation, a lot of people begin to show their age,” Kirton said.“There are just so many ticks you have on the clock.”
Doctors said many older people, especially the ones who feel pretty good, don’t understand how vulnerable they are. After age 65, our lungs and kidneys don’t work as well, Mendelson said. Blood vessels become stiffer and less responsive. All these factors affect healing, even without chronic conditions like diabetes and heart disease.
Older patients “have a tendency to not ask as many questions as some of our younger patients,” McDonald said, “and they often think they’re going to get better faster than they do.”
Cognition, however, is always a concern, doctors said.
“The one organ system they really want to make sure works well is their brain,” said Roderic Eckenhoff, vice chair for research in the department of anesthesiology and critical care at Penn Medicine.
This is one reason why delirium is getting so much attention. Eckenhoff said there are also patients who report that they’re just not as sharp after surgery, perceptions that studies support. For most, the symptoms abate in two to three months. While there’s still a “fairly intense” debate, he said, studies so far point to the trauma of the surgery itself rather than anesthesia as the cause of cognitive problems.
Don’t forget the glasses and hearing aids
He said Penn surgeons have begun warning patients that they may experience decline and might want to forgo major life decisions for a few months after surgery. The doctors also try not to over-sedate elderly patients and are extra-careful with opioids and certain antianxiety drugs, which seniors don’t handle as well as younger people do.
McDonald’s team at Duke likes to talk with patients well before they come to the hospital to get an idea of how well they’re functioning and whether they have social support. Nutrition is a frequent problem, with a third of older people malnourished. “It’s amazing how many people just eat like one meal a day and a few snacks,” she said.
Ideally, patients are seen in person two to four weeks before surgery. A nurse sees how fast they can walk and how many times they can sit down and get up from a chair — without hands — in 30 seconds. “If someone can’t get out of a chair, they’re not going to do well after surgery,” McDonald said, “because getting them up and moving is the number-one way to prevent lots of complications from surgery.”
She makes sure they or a caregiver understand which medications to stop and when. She sets reasonable expectations. If they’re going to need a walker, she tells them. She knows older women resist drinking enough because of bladder leakage, so she explains the importance of staying well-hydrated for at least the three days before surgery.
After surgery, geriatricians say older patients need family members nearby. During the day, their window shades should be open and they should be kept awake and engaged as much as possible, and allowed to sleep at night without interruption. They should be wearing their glasses and hearing aids because poor vision and hearing raise the risk for delirium.
Helping older patients thrive, especially after surgery, requires attention to small details, Mendelson said. “It’s a lot of very little things.”