10 things a cardiologist wants you to know about new blood pressure guidelines
The point is not to put more people on medication, which can come with side-effects, but to get more Americans to reduce their numbers through lifestyle changes.
The dust is still settling after a sweeping new definition of high blood pressure was recently released, which let us know that almost half of all Americans are now classified as having hypertension.
Are these new directives helpful, or another step on the road to everyone being on prescription medications? As one of my patients said, "First you lowered the cholesterol numbers and now blood pressure, do you want us all on medication?"
To answer that question, here is a top 10 list of what you need to know about the new guidelines.
The new "normal" blood pressure now is a systolic (top) limit of 120 mmHg, and diastolic (bottom) limit of 80. If your systolic is more than 130, and diastolic is more than 80 mmHg, you have a diagnosis of hypertension.
Medications are never indicated if your blood pressure is within 10 points of this new normal; instead the treatment is to work on lifestyle changes.
Losing weight, restricting salt, increasing the potassium in your diet, and exercising is the way to go, not medications, unless your blood pressure remains high.
If you have other no medical problems, you should not be on medication unless your systolic pressure is more than 140. But, if you have other issues that increase your long-term risk of having a heart problem (such as smoking, diabetes or a family history of heart disease), 130 is your threshold for medication. This is the most controversial recommendation, because these medications may have side-effects, including lightheadedness, fainting, or worsening kidney function.
The way blood pressure is taken is very important. A single elevated reading in a doctor's office simply suggests that more readings are needed.
The correct way to take blood pressure is to sit in a quiet room in a comfortable straight-backed chair, without having had coffee or alcohol recently, and having rested quietly for at least five minutes. It should be repeated twice more, five minutes apart, and the three readings should be averaged. Otherwise, you should not be labeled as having hypertension.
The DASH diet, which is similar to a Mediterranean diet — rich in fruits, potassium, nuts, vegetables, and low in saturated fats — has been shown to reduce the top blood pressure reading by more than 11 mmHg. Regular exercise can lower it another 4 mmHg.
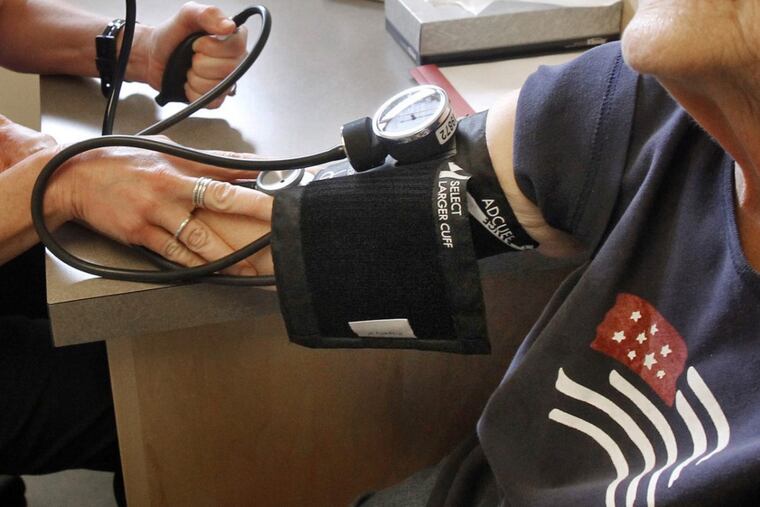
The type of cuff that is used can make a big difference. If someone has a large arm, and a small BP cuff is used, the numbers may be artificially elevated.
Use an arm cuff, not a wrist cuff. A good home device that automatically takes your pressure usually does not cost more than $50, and may be covered by your insurance
If you need medication, usually the best way to start is with a water pill (diuretic), medications called ACE inhibitors/Angiotensin receptor blockers, or calcium channel blockers. If you experience any negative side-effects from a new medication, stop taking it and let your doctor know right away.
The new guidelines are helpful because for the first time, there is a careful roadmap illustrating the importance of lifestyle change and the correct way to take blood pressure readings before we consider medications.
It is always better to have a lower reading, ideally with a top number below 120, but getting there with medications can lead to lots of unpleasant side-effects. Because of this, I will not be starting more of my patients on medications as a result of these guidelines.
The take-home message should not be that half of the adult population should be on medication for high blood pressure, but that more adults should be exercising regularly, following a DASH diet, not smoking, and not be overweight. Sadly, only about 3 percent of Americans presently accomplish all four of those goals. If these guidelines can bump up that woeful percentage, they will be worth their weight in gold.
David Becker, M.D., is a board-certified cardiologist with Chestnut Hill Temple Cardiology in Flourtown, Pa. He has been in practice for 25 years.