New hope for rising tide of boomers with hepatitis C
Michael Secreto has no idea where he picked up hepatitis C. Tattoos made with India ink and needles passed among 12-year-old friends in South Philly? Hard drugs as a teenager? Blood from dialysis patients when he drove paratransit vehicles in the 1990s?
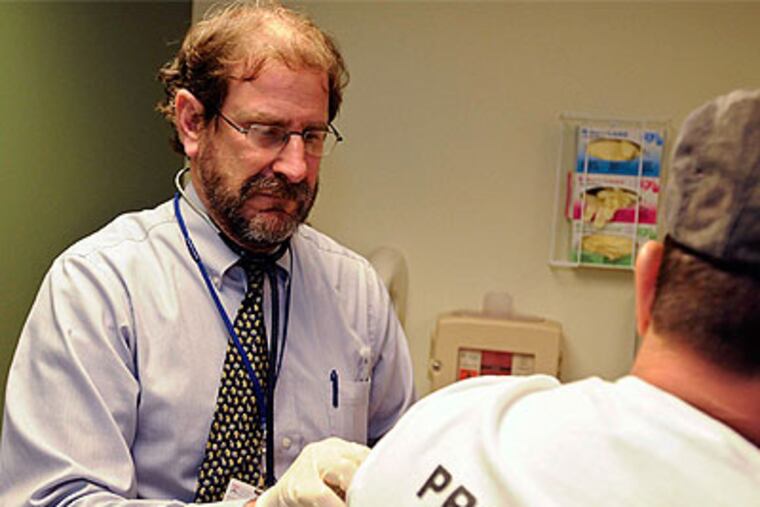
Michael Secreto has no idea where he picked up hepatitis C. Tattoos made with India ink and needles passed among 12-year-old friends in South Philly? Hard drugs as a teenager? Blood from dialysis patients when he drove paratransit vehicles in the 1990s?
The infection was a surprise, discovered after Secreto's wife heard about hepatitis and suggested he get tested a decade ago. Back then, the treatment didn't work for him. Now, midway through a new drug regimen, the virus is down to undetectable levels. It likely saved his liver, and perhaps his life.
At 56, Secreto is squarely in the middle of a generation that once again is playing an outsize role: Baby boomers are five times as likely to be infected with hepatitis C as other age groups. The chronic infections, largely from risky behavior that caused no symptoms for 20, 30, or 40 years, are now leading to liver disease in increasing numbers. And, as boomer luck would have it, the first treatments that work for most people are just now becoming available, with more in the pipeline.
"Patients are coming from everywhere," said Jonathan Fenkel, director of Thomas Jefferson University Hospital's new Hepatitis C Center. Some had tried to give blood and were rejected. Others had elevated liver enzymes in lab tests ordered for unrelated reasons, often the first clue to having the disease.
An estimated three million to five million Americans have the virus. Though the number of new infections is relatively stable, disease caused by chronic infections is steadily rising. Hepatitis C is the top cause of liver transplants. It contributed to more than 16,000 deaths in 2009, the most recent year available - 5,000 more than died of HIV.
Many boomers have long forgotten dabbling with injection drugs. With no symptoms and no Magic Johnson or ACTUP to make the disease a household word, between 50 percent and 75 percent have no idea they are infected.
The result is "an age wave of persons progressing through time who are at increasing risk for severe liver disease," the Centers for Disease Control and Prevention said last month as it proposed recommending testing for every person born between 1945 and 1965.
Hepatitis means inflammation of the liver. There are various causes, including heavy alcohol use, but most cases are caused by viruses.
One of those viruses, hepatitis B, can circulate in various bodily fluids and be transmitted through sex, birth, and contaminated needles. It can cause chronic illness and serious liver damage. Researchers reported last month that more than two million U.S. residents may be infected. Most were born in foreign countries. Babies born here are routinely immunized against hepatitis A and B, the only types for which there are approved vaccines.
Hepatitis C is transmitted through contact with infected blood. Widespread screening to protect the blood supply began in 1992, four years after the virus was identified. Before then, some people were infected via transfusions; dialysis and high-risk sexual behavior also raised the risk.
Contaminated needles were the main source, however, and were the primary way the 3 percent to 4 percent of boomers were infected. Experts say dirty-needle use also helps explain why men's rates are twice those of women, and why cities have high rates.
Drug use also seems to explain a near-doubling of new infections from 2003 to 2010 in adolescents and young adults. They are the one demographic in which infections are rising, said Sameh Boktor, adult viral hepatitis prevention coordinator for the Pennsylvania Department of Health, who presented state data at a March conference.
"The biggest increase is in rural areas," Boktor said. Local liver doctors said they were seeing more young patients from the suburbs and beyond whose infections were found through tests at drug programs.
Although some will never get sick, without treatment, more than 60 percent of infected people will develop chronic liver disease. Up to 5 percent will die of cirrhosis or liver cancer - one million deaths over the next 40 to 50 years, the CDC projected.
The problem is, treatment can be a nightmare.
The standard combination of two old therapies - the daily antiviral pill ribavirin and weekly injections of immune-boosting peginterferon - works in just 40 percent of cases, takes almost a year, and has horrible side effects.
Two new drugs approved in May 2011 each nearly doubled the rate of what is known as a sustained virologic response, driving levels of the virus so low it is often described as a cure.
Boceprevir (marketed as Victrelis by Merck) and telaprevir (sold as Incivek by Vertex Pharmaceuticals) are protease inhibitors. Like HIV drugs, they work by blocking an enzyme, known as protease, that the virus needs to replicate. Incivek also reduces treatment time to 12 to 24 weeks in some cases and has taken the bulk of their combined $1.5 billion in sales so far, according to IMS Health.
Unfortunately, each is given in addition to the old drugs, not in place of them.
"It is like oral chemotherapy in terms of side effects," said Jay Kostman, associate director of the Center for Viral Hepatitis at the University of Pennsylvania Health System. He has patients come into the office for their weekly interferon shots partly so he can monitor them for depression and other problems.
"It plays with your head," said Michael Secreto, the South Philadelphia patient, who said he lost 17 pounds in the first 12 weeks of what is expected to be a 48-week course. "The wrong person on this medicine I wouldn't recommend them having a gun. It makes you crazy."
People with certain medical conditions are ineligible for the regimen, as are one-quarter of those with hepatitis C other than genotype 1.
Other protease inhibitors are coming soon. And then there's the holy grail of hep C treatment: daily pills without interferon or its side effects. Dozens of drugs are in the pipeline, with the first approvals perhaps three to five years off.
Researchers say the new drugs will attack different parts of the virus' life cycle, and will likely be given in combination cocktails, like HIV drugs, to prevent the virus from developing resistance to any single drug.
"There are billions of dollars that can be made by hepatitis C therapy," said Stacey B. Trooskin, an infectious-disease fellow at Penn who will move to Drexel in July.
Like many of her colleagues, Trooskin supports the idea of widespread screening. She worries, however, that many patients will not be able to afford treatment that currently costs $50,000 to $100,000.
Many state correctional systems, including New Jersey's, avoid routine screening, a step that reduces their obligation to treat one of the highest-risk populations. In Pennsylvania, which screens all inmates, 17 percent are infected. Treating just a small portion of them with the latest drug regimen is expected to cost more than $6 million a year, a Department of Corrections spokeswoman said.
For those outside prison, private insurance typically covers treatment, but studies have found that more than 30 percent of infected people are uninsured.
"The baby boomers are aging, and, finally, their silent disease is going to start talking and they are going to get sick," Trooskin said. "I think as a health-care system, we are really unprepared."