A new frontier in ICU research: Postintensive care syndrome
One woman left Johns Hopkins' intensive-care unit believing her husband and nurse had been plotting to kill her. Another ICU patient had flashbacks of hospital walls covered in blood.
One woman left Johns Hopkins' intensive-care unit believing her husband and nurse had been plotting to kill her. Another ICU patient had flashbacks of hospital walls covered in blood. A third had visions of big spiders riding bicycles in her room. Suddenly, a favorite hobby, gardening, felt creepy.
Doctors used to think patients returned to normal after the delusions and hallucinations of ICU delirium stopped. They're learning instead that some leave the hospital with terrifying false memories, often of being assaulted or imprisoned. The horrible visions help explain why a recent Johns Hopkins study found that one in four patients had post-traumatic stress symptoms two years after going home.
Now that ICU doctors have gotten better at saving patients' lives, they are asking what comes next. The answers are disturbing.
Researchers are finding that months - even years - after patients leave the hospital, many struggle with physical weakness, thinking problems, anxiety, depression, and PTSD. Even younger patients often cannot return to work.
Last year, the Society of Critical Care Medicine gave the constellation of problems a name - postintensive care syndrome - and ICU doctors around the country are revamping care in hopes that the lives they save will be less troubled.
Many of the changes - less sedation, more exercise, 24-hour visitation, dark rooms at night to encourage more normal sleep - are meant to reduce delirium. About 75 percent of ICU patients develop delirium, which is associated with poorer survival and more long-term problems.
"This is one of the . . . biggest issues in critical care in the United States right now, understanding why this happens and figuring out how we can mitigate it," said John Hansen-Flaschen, chief of the University of Pennsylvania's pulmonary, allergy, and critical care division.
Patients often look normal after they've been home a while, and family and friends expect them to bounce back. "That's very hurtful for people who are broken, and no one believes they are broken," Hansen-Flaschen said.
One reason it has taken ICU doctors so long to notice the problem is they often do not see patients who recover enough to be moved to another floor. Now critical care doctors are wrestling with how to spread the word to primary-care colleagues and others who see the patients after discharge.
"There's a potential for errors in diagnosis and assessment if you don't really know about this," said O. Joseph Bienvenu, a Johns Hopkins psychiatrist among the pioneers of ICU survivorship research.
Experts on post-ICU problems concede even their own hospitals are not doing an ideal job of informing patients and families about the future they may face or of coordinating follow-up care.
"They essentially are sent off to fend for themselves," said James Jackson, a psychologist at Vanderbilt University Medical Center, which opened an ICU follow-up clinic six months ago.
Each year, about a million Americans are hooked to a ventilator in an ICU. Studies of survivors often have focused on those with serious lung problems or sepsis, a serious infection. Doctors believe their findings likely translate to a broader group and even to delirious patients who were not in ICUs.
Half or more of ICU survivors have trouble with basic living activities a year after discharge. Of ICU patients with severe lung problems, 55 percent had cognitive impairment and 36 percent had depression a year out, a Penn study found last year.
Hansen-Flaschen said a typical patient with ongoing problems was treated for a "pneumonia from hell" that would have been universally fatal 40 years ago. Now, most survive.
But long after they go home, they may be weak and tired. They have trouble concentrating, making decisions, and remembering, he said. They may cry or laugh too easily and are plagued with the kind of upsetting memories that define PTSD.
In a study last month in Psychological Medicine, Bienvenu and Hopkins colleague Dale Needham found that a third of patients who survived an ICU stay for acute lung problems had symptoms of PTSD three months later, often due to false memories. "People are really upset by these experiences," Bienvenu said. "They don't know how to incorporate them into their real memories."
Patients often understand that the things they remember probably did not happen, but doctors said the memories feel real in a way that nightmares do not.
Patients may fear telling anyone about the rape or assault they recall. One patient thought he left Hopkins nightly to visit a sushi bar where he had to swim through a pool of man-eating fish before he could dine.
Another thought that his penis had been cut off and that doctors would not sew it back on unless he paid $8,000.
Needham said the most common delusion is that "a nurse is trying to kill you." It turns out that is even more upsetting than almost dying.
Doctors think many delusions are loosely tied to real things staff do to save patients' lives, such as placing catheters and breathing tubes.
Jackson said one Vanderbilt patient thought he was on a conveyor belt feeding into an oven. (He had gotten an MRI.)
The recollections are not always terrible. A Penn patient believed he had awakened in heaven. Susan Gregory, a director of the medical ICU at Lankenau Medical Center, had a patient who could not stop talking about the Pointer Sisters when he woke up. She said a nurse resembled one of the singers.
In the past, ICU doctors were often unaware of what patients were imagining. Patients could not talk with breathing tubes down their throats. Once those were out, doctors knew the most combative patients had problems. "That's really the tip of the iceberg," said David Oxman, a critical care doctor at Thomas Jefferson University Hospital.
Staff at Jefferson and other ICUs now screen patients for delirium daily, even those on ventilators. One of the questions: Can a stone float on water? Patients with delirium will say yes.
Some amount of delirium may be unavoidable. ICU patients are deathly ill. Even with mechanical breathing help, their brains may not get enough oxygen. Inflammation may also play a role.
ICU doctors used to think they were doing their patients a favor by keeping them heavily sedated. They now know that that worsens delirium. Patients still need sedation, but most ICUs have cut back on a class of sedatives called benzodiazepines - drugs such as Valium and Ativan - that up the odds of hallucinations.
They also administer sedatives intermittently, so patients are sometimes more awake. "We need them to touch reality," said William Schweickert, a critical-care doctor at Penn.
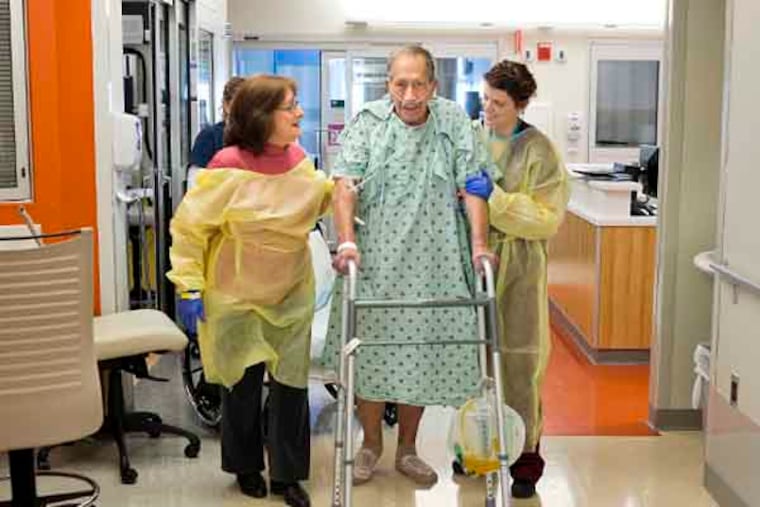
Another key strategy is starting physical therapy earlier. It is now not unusual to see ICU patients on ventilators walking in the hall. Penn and Hopkins have motorized, recumbent bicycles patients can use in bed. Schweickert, an early advocate of the practice, said it speeds recovery.
Sleep has also become a priority. Leading ICUs are no longer noisy and bright 24 hours a day. They turn off the lights at night. Hopkins reported this month that changes meant to improve sleep quality raised the odds patients would be delirium-free by 54 percent.
Penn now encourages families to bring objects from home and visit any time. Hearing a familiar voice is not only "vocal anesthesia," Schweickert said, but also anchors patients in reality.
Hospitals even consider their art. Abington Memorial Hospital took a painting of a yellow daisy off the wall after many patients said it was moving.
Penn and Hopkins are now considering adding ICU diaries, a tool pioneered in Europe that has reduced PTSD after intensive care. Relatives and nurses record what occurs in the ICU. Later, they share it with the patients.
"They allow patients to process what happened," Bienvenu said, "and recognize that their memories were distorted."