Hospitals work to cut deadly ICU infections
The patient was on a ventilator at Cooper University Hospital, and his head was positioned so that saliva dribbled down one side of his neck - a common result of having a breathing tube in your mouth.
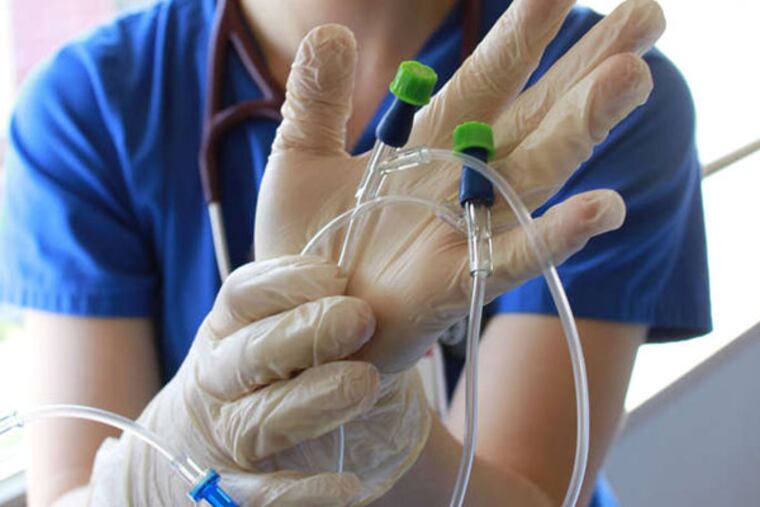
The patient was on a ventilator at Cooper University Hospital, and his head was positioned so that saliva dribbled down one side of his neck - a common result of having a breathing tube in your mouth.
But intensive-care nurse Karen Fluehr-Heinkel noticed a problem: the saliva was landing right where a catheter had been inserted into the man's jugular vein.
So she did something that once would have been unheard of: she immediately got a doctor to fix it.
"We've been empowered to speak up," said the nurse, a 25-year veteran of the Camden hospital.
Another blow struck in the national war on germs. Fluehr-Heinkel was worried that microbes could travel into the man's bloodstream, leading to a type of infection that kills an estimated one in five patients who get it - thousands nationwide each year.
These "central line-associated" infections - along with a less serious, but more common variety that arises after the insertion of a urinary catheter - were once seen as an inevitable consequence of being in the hospital. Now the goal is prevention, amid evidence that a mix of common-sense sanitary measures can make a difference.
An Inquirer analysis of data from intensive-care patients on Medicare suggests that area hospitals are making progress.
Of the 42 facilities for which data were available, 11, including Cooper, did better than predicted at preventing infections related to central lines. These widely used plastic tubes are inserted into a large vein, typically in the neck or chest, to deliver fluids and medicine.
The predicted infection numbers were determined by a Centers for Disease Control and Prevention formula that takes into account hospital size and types of intensive-care units, among other factors.
Five area hospitals did worse than predicted at preventing infections associated with urinary catheters, though several said their numbers had improved since then. And just two local hospitals, Hahnemann University Hospital and Temple University Hospital, were better than predicted at preventing both kinds of infections.
The efforts are driven partly by pressure from insurers to cut costs. Medicare no longer pays for treatment of these infections, along with other conditions deemed to be caused by the hospital. An added penalty was proposed this month: Medicare would cut payments to hospitals whose rates of these infections are too high.
Amid the scrutiny, the numbers have dropped. The CDC estimates that central-line infections fell 41 percent from 2008 to 2011, though an exact comparison is tricky because more hospitals are now reporting.
Hospitals in the eight-county Philadelphia region reported 254 central-line infections in Medicare intensive-care patients from mid-2011 to mid-2012, and 263 urinary-catheter associated infections in the first half of 2012.
Data for prior years were unavailable, because Medicare recently switched from analyzing billing records to clinical data, which is considered more accurate.
Yet, because the infections are reported by the hospitals themselves, some experts suspect that not all cases are submitted. Many states do not audit the data, though Pennsylvania and New Jersey have done so. In California, a review of 100 hospitals found more than one-third of central-line infections were not reported, in some cases due to confusion.
Still, there is real improvement, said Peter J. Pronovost, a Johns Hopkins University researcher who put the issue in the national spotlight by helping Michigan hospitals to slash infection rates.
Pronovost cites what happened in Michigan, where the ICU mortality rate fell 10 percent, compared with 11 states that had yet to adopt broad anti-infection measures.
"Moving mortality in a whole state is unheard of," he said.
So how are local hospitals doing it? Among the tools are: