Targeting a tumor
When Christopher Teti was diagnosed with aggressive brain cancer in 2011, Kevin D. Judy performed traditional surgery at Thomas Jefferson University Hospital. He removed a portion of Teti's skull and cut out the tumor.
When Christopher Teti was diagnosed with aggressive brain cancer in 2011, Kevin D. Judy performed traditional surgery at Thomas Jefferson University Hospital. He removed a portion of Teti's skull and cut out the tumor.
When a second tumor showed up this year, Judy tried a far less intrusive approach. He and colleagues drilled a dime-size hole in the patient's skull, inserted a slender, laser-emitting wand, and destroyed the malignant growth with heat.
Aside from the drilling part, Judy did the procedure from a separate room, pushing down on a foot pedal to turn on the laser inside Teti's skull. The patient lay inside an MRI machine, which delivered real-time images to Judy's computer screen, indicating when the tumor cells had reached the desired temperature.
Within minutes, it was over.
As with every other part of the body, surgeons have increasingly chosen to operate on the brain with minimally invasive surgery - reasoning that it leads to quicker recovery and, they hope, better outcomes.
Researchers have not proven that brain-cancer patients who get the laser treatment live longer than those who get regular surgery. But Judy and other surgeons say early results are promising, touting it as an option for those whose tumors are in sensitive or difficult-to-reach areas of the brain.
The kind of cancer Teti had, glioblastoma, is a grim disease, killing most of its victims within a year or two. No matter what method surgeons use to remove the initial tumor, it almost always comes back.
Yet Teti, 55, had an upbeat outlook.
The Fairmount resident had already beaten the odds with the traditional surgery in 2011, making it three years with no recurrence of the dizziness, numbness, and other symptoms that first signaled a problem.
When an MRI scan in August showed that a marble-size tumor had come back in his left frontal lobe, he was unwilling to undergo the risk of having his skull cut open again. But upon hearing from Judy about the laser treatment, Teti was game.
So on Oct. 1, he had a date with a drill.
The 'lunar lander'
You know the carpenter's adage, "Measure twice, cut once"?
For a brain surgeon, they should change it to "Measure dozens of times."
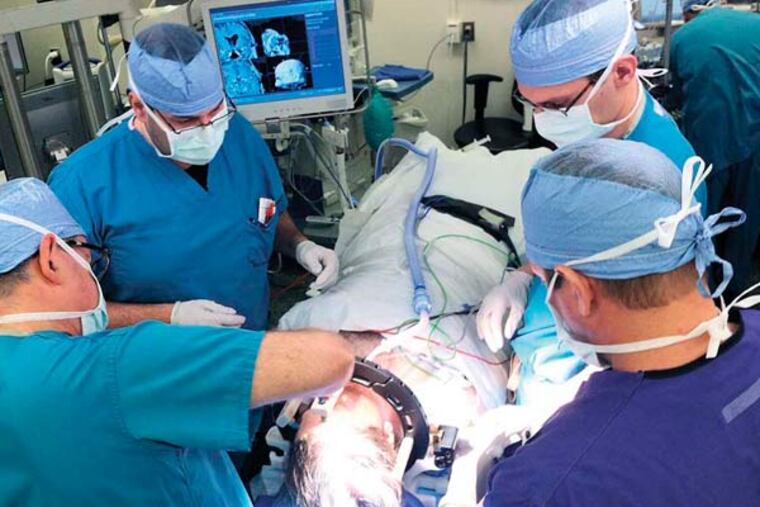
The Jefferson surgical team fixed Teti's head into position with screws. Then team members spent nearly an hour checking and rechecking the position of his skull and the tumor inside it before drilling.
They could not see the tumor, but they knew where it was from an MRI image taken the day before. They determined where to drill by gently touching his head in various spots with infrared probes. This process yielded a real-time map of the skull that they could then match up with the earlier MRI image, which showed both the skull and what was inside.
At 9:10 a.m., surgical resident John C. Styliaras fired up the drill. He gently guided the whirring device through the flesh and bone, creating a small, round hole with very little blood.
Then the patient went for yet another MRI, this time so the surgical team could watch as Judy did the procedure. The team had fastened a small white tripod to Teti's skull, which surgical technician Nathaniel Bryan called "the lunar lander." The tripod had a hole in the center to guide the placement of the laser probe.
As Teti lay in the MRI doughnut, Judy and colleagues sat on the other side of the wall. A robotic device lowered the laser probe through the hole into Teti's brain as the team watched on a screen.
Then Judy delivered heat to the tumor by pressing a foot pedal, occasionally using a computer mouse to adjust the laser's position. Asked if he had ever imagined sitting at a computer to perform surgery, he responded with mock outrage.
"It takes great skill to step on this pedal!" Judy said.
Joking aside, it was indeed a painstaking, if brief, process. As he adjusted the position of the laser, Judy had to keep a close eye on the computer screen.
The system's software was continuously updating and redrawing contour lines to indicate when various parts of the tumor had heated enough so its cells would die. The goal was to hit 43 degrees Celsius (109 degrees Fahrenheit) for 10 minutes (or a shorter duration if the temperature exceeded that level).
The system Judy used is called NeuroBlate, made by Monteris Medical Corp. of Plymouth, Minn. A competing product that also uses lasers to heat up tumors, called Visualase, is sold by Medtronic Inc., of Minneapolis.
Both also have been used to treat patients with epilepsy. One of Judy's colleagues at Jefferson, Ashwini Sharan, uses the Visualase system for that purpose, saying he prefers its narrower probe.
Surgeons have been using lasers for decades to ablate tumors in various parts of the body. What is new is software that enables pinpoint measurement of temperature in each cluster of cells.
As with any procedure, insurers pay hospitals varying amounts depending on the coverage and geographic area. Medicare reimburses about $30,000 for the type of tumor ablation that Teti underwent, Jefferson officials said.
Teti's treatment lasted barely 15 minutes. Many patients go home the next day; Teti stayed in the hospital an extra day because at first, he had trouble pronouncing a few words.
Now he sounds great. A retired administrator of federal government contracts, Teti spoke easily and articulately by phone a few days after surgery, full of praise for his surgeon.
"He's saved my life twice," Teti said of Judy.
But even if it was good for Teti, is the surgery a good idea for everyone?
Evidence
A study led by Alireza M. Mohammadi, a surgeon at the Cleveland Clinic, analyzed the results of the laser treatment in 34 brain-cancer patients. In cases where the surgeon was able to treat all or most of the tumor with heat, the cancer came back in about 10 months, whereas those with poor "coverage" had tumors come back in five months, on average.
Those results are not very useful for patients, said Diane Robertson, director of health technology assessment at ECRI Institute, a nonprofit organization in Plymouth Meeting that evaluates evidence for medical devices and procedures.
The study did not compare the laser treatment with other approaches, so there was no way to tell if it was any better or worse, she said. What's more, the study would have been more helpful had it measured the patient's quality of life, she said.
"You don't want to see patients being told that there's something that is going to help them when there isn't any evidence to indicate that it is," Robertson said.
Lynne Taylor, director of neuro-oncology at Virginia Mason Medical Center in Seattle, had similar concerns.
"They're not talking about the patients' symptoms," said Taylor, a fellow of the American Academy of Neurology. "They're talking about what the MRI scan looks like."
Mohammadi, the Cleveland Clinic surgeon, acknowledged that the study should be viewed with caution, but said "as an initial report, it was promising."
He said a randomized trial was in the works, in which patients who get the laser treatment would be compared with those who get a biopsy followed by chemotherapy and radiation.
Mohammadi's study of 34 patients, published in the journal Cancer Medicine, also did not follow the patients long enough to determine their median survival rate.
For Teti and most other patients, that's a big one. And by that measure, three and a half years after his initial diagnosis, with two kinds of surgery under his belt, he is doing great.
215-854-2430