In Philly, doctors bring specialty care to communities that need it most
Rose Carvalho had not been to her doctor for a while. Then she got a letter asking whether she would be interested in a free eye exam - at her primary-care doctor's office.
Rose Carvalho had not been to her doctor for a while. Then she got a letter asking whether she would be interested in a free eye exam - at her primary-care doctor's office.
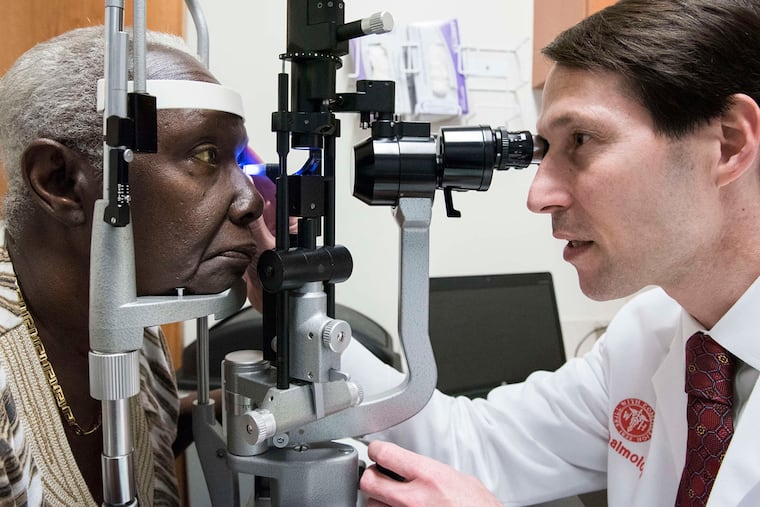
It was good timing because she had noticed changes in her night vision and had trouble reading the guide on the TV screen. The former social services worker saw a Wills Eye Hospital doctor who made the trip from the Center City institution to Spectrum Health Center in West Philadelphia for the exam, part of federally funded research aimed at lowering barriers to care.
The result: Carvalho learned she has a small cataract and some warning signs that she might have diabetes, and scheduled follow-up appointments to investigate both.
Carvalho says she knows plenty of people who are reluctant to go to doctors in general and specialists in particular.
"As long as we can see, we're fine," she said. "A lot of time, people don't go because they don't have insurance, and they have no idea if they have diabetes or glaucoma."
Medical practices are making it easier for patients to multitask, offering eye exams at primary-care offices or dental services at pediatric visits, and taking blood pressure at barbershops. Some of the changes are attempts to make things easier for busy families. Other offerings are intended to reach people who can't afford to see a doctor or dentist or eye doctor regularly.
Stethoscope and a book
As a pediatrician at St. Christopher's Hospital for Children and director of Community Pediatrics and Child Advocacy, Daniel R. Taylor serves some of the city's poorest families. He greets his young patients with the usual stethoscope, plus some less-expected items, including an age-appropriate book to encourage reading and fluoride treatments to encourage good dental health. Taylor and his colleagues also make sure families are receiving appropriate benefits such as food stamps. There are a lawyer and four social workers on staff for more complicated needs. Taylor hopes to bring in an ob/gyn and a psychiatrist soon.
"In medical school, we're taught that it's genetic code that determines health and behavior, but the zip code you live in has a huge impact," Taylor said.
With numerous resources in the same location - an eye doctor is 50 steps away, he said - families can get everything done in a same-day visit.
"We do know that if we don't invest in their health now, we'll pay tenfold down the road," he said. "Kids get hurt in unsafe neighborhoods and unsafe blocks."
One-stop approach
That one-stop approach took medical centers some time to appreciate. Fifteen years ago, as a physician at Wills Eye, Jeffrey Henderer tried to offer free glaucoma testing to low-income Philadelphians at senior centers. Doctors would show up in a van, do a quick test, and contact people who showed signs of the disease, which results in irreversible blindness.
It didn't work. A lot of people got screened, but very few came to the doctor's office to get the care they needed.
"Part of it was some of them forgot about the screening, but it was also that they didn't know us as physicians," said Henderer, who is chair of the department of ophthalmology at the Lewis Katz School of Medicine at Temple University. "We thought it was cost, but the medical care was free. We thought we were failing to communicate as physicians. Race didn't matter. No one followed up."
It wasn't enough to show up and leave, he said. The eye doctors needed to get the primary-care doctor involved so patients would buy in.
"Ninety percent of the people had primary-care physicians, but none of them went to the ophthalmologist," he said.
Now Henderer, along with research coordinator Martin Schardt and several medical students, travels to Philadelphia Health Center 5 at 1900 N. 20th St., by Temple's campus, to give eye exams. They have a 50 percent show rate, far better than the 20 percent they saw before, and people come back for treatment.
The group makes three visits a month, two of which are funded by the Wills grant. The five-year, three-part program focuses on testing for glaucoma, the top cause of blindness in the African American and Latino communities, said L. Jay Katz, chief of the Wills Eye Hospital glaucoma service.
The first phase involved mobile units visiting senior centers and churches. Now the group is working with 17 primary-care offices, and the next step includes social workers to encourage patients to follow up with a local eye doctor. In the current phase, the primary-care offices offer a free telemedicine screening that takes about 20 minutes - without dilation - to screen for glaucoma. Primary-care doctors refer the patient to the screening, focusing on people at risk and those over 50. The scans are read at Wills, and patients with abnormalities are invited back for a complete exam at the doctor's office, Katz said.
'Invisible' diseases
Leila Hardware, a primary-care physician at Spectrum Health Services, said that for the nine months Wills has been at the center, she has sent about 20 patients a month for the screenings.
"This is the best idea because people don't want to come and see me and then have to go to other places to get other things done," she said. "They can see me and go to the next room. I can tell them to just go downstairs for an X-ray."
Hardware calls glaucoma a "huge problem" for the center's patients.
"They don't see the need to take care of something that's not painful," she said. "A lot of older people lose a little vision and they think it's because of age, not because of something that might cause blindness."
"Invisible" diseases such as glaucoma and hypertension often are caught in the early stages with regular checkups, physicians say, and that's why it's so important to reach patients before the results are irreversible or even fatal.
Krystal Hill, a first-year University of Pennsylvania medical student, visits the Philly Cuts barbershop in West Philadelphia as part of the Student National Medical Association's Cut Hypertension program. She typically goes twice a month, and sometimes the blood pressure numbers she finds are so high that she has sent customers (and once, a barber) to the emergency room.
"It's not a home visit, but the barbershop is a home base," said Hill, 27, who is from Houston.
Hardware says the trend of health centers offering multiple services will continue, particularly for underserved communities whose members might not otherwise seek care until it's too late.
"They'll go to the doctor when they're sick, but a lot of illnesses you don't realize until it's far gone, until you have cancer, or they're taking your foot off in the ER because of diabetes, and it could have been prevented," she said.