Doctor didn’t offer a flu shot? It might depend on time of day
But an electronic "nudge" seemed to help, Penn researchers found.
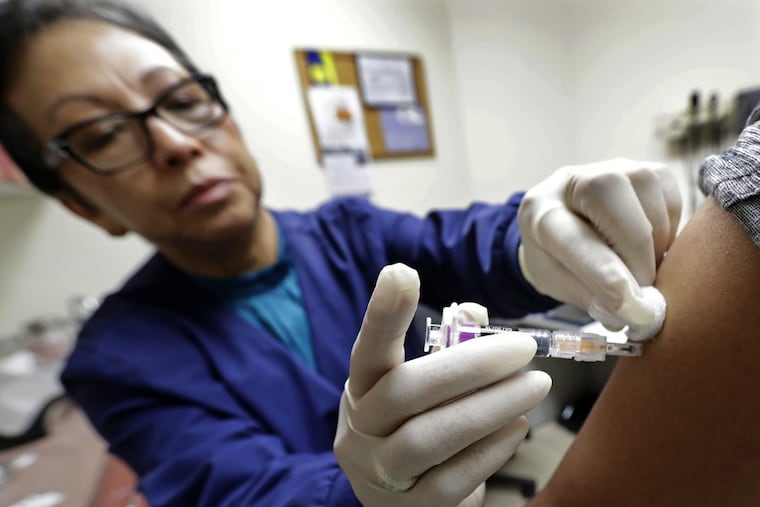
A couple of complex cases come through the door. Perhaps there is a battle with an insurance company. As the day wears on, even the most efficient physician can fall behind schedule.
One possible result, according to a new University of Pennsylvania study: Fewer patients get flu shots.
That finding came from a review of 96,000 patient records at 11 primary-care clinics in the Penn Medicine health system, published Friday in the journal JAMA Network Open. The rate of patients getting flu shots fell more or less steadily throughout the day — from 44 percent for those with appointments during the hour starting at 8 a.m., down to 32 percent by the late afternoon.
But in addition to identifying that shortcoming, the study authors offered a promising solution: an electronic nudge.
In the final year of the three-year study, nurses and medical assistants at three of the 11 doctors' offices received an automatic, computerized notice to create a vaccination order for each patient. The rate of patients getting flu shots at those clinics jumped by nearly 20 percent relative to the vaccination rates at the other clinics.
Flu Vaccine Rates by Time of Day
Penn researchers have reported success with nudges in a variety of other health-care settings, such as boosting prescriptions of cholesterol-lowering statins and improving the rate at which heart-attack patients are referred to a rehab program.
They even have a team — the Nudge Unit — devoted to studying the concept. Billed as the "first behavioral design team embedded within a health system," the unit is holding a symposium Monday and Tuesday to share the latest tools with executives from 21 health systems.
The concept of nudging is about more than just flashing notices on a screen, which can blend together in the stream of electronic alerts that wash over clinicians every day, unit director Mitesh S. Patel said. A better approach, he said, is to require an "active choice."
That method was implemented at three of the 11 clinics for the flu-shot study, led by Patel and Rebecca H. Kim, a resident physician in Penn Medicine's primary-care track. During the process of recording a patient's blood pressure and other vital signs, the nurse or medical assistant was required to click "accept" or "decline" in response to a computerized prompt to create a flu-vaccine order.
"You can't move forward without answering yes or no," said Patel, an assistant professor at Penn's Perelman School of Medicine.
The idea is that, upon seeing the order, the physician discusses the flu vaccine with the patient and, upon getting a thumbs-up, signs the electronic document so the shot can be administered.
In the three clinics where the nudge was used, nearly 60 percent of patients received a flu vaccine at some point during the 2016-2017 flu season — compared with less than half of patients at other clinics during the three flu seasons spanning September 2014 through March 2017.
(For both groups of clinics, these vaccine rates reflected whether patients got a shot at any point during the flu season. In the separate analysis of vaccine rates by time of day — with the rates ranging from 32 percent to 44 percent — the figures reflected only the patient's first doctor visit for the year in question.)
The study had some limitations, among them that clinics getting the nudge were not selected at random, but chose to participate — meaning that their higher vaccine rates could be due to increased motivation by the staff. Still, vaccine rates at the nudge clinics improved significantly even when compared with their own past performance — suggesting that the nudge did indeed make a difference.
The researchers plan to conduct a randomized study in the future. They estimated that if their early evidence is any guide, the nudge would enable Penn Medicine to vaccinate an additional 5,000 patients each year at its 36 primary-care practices.
At all clinics in the study, flu vaccine rates improved somewhat just after lunch before declining again — suggesting that physicians were able to get back on schedule temporarily.
While the lower vaccine rates later in the day are likely due to physicians falling behind, another factor could be that afternoon patients are in a hurry to get home, Patel said.
The flu vaccine is not the only type of health-care delivery that changes over time. As the day wears on, hospital staff are less likely to wash their hands, one study found. Physicians also are more likely to prescribe antibiotics when the drugs are not warranted — suggesting that when pressed for time, they may be caving to the demands of sick patients who just "want something."
