Penn study finds deadly C. diff infections are on the rise
Penn study finds big upsurge in bacterial infections particularly dangerous to the elderly. A newer treatment holds promise.
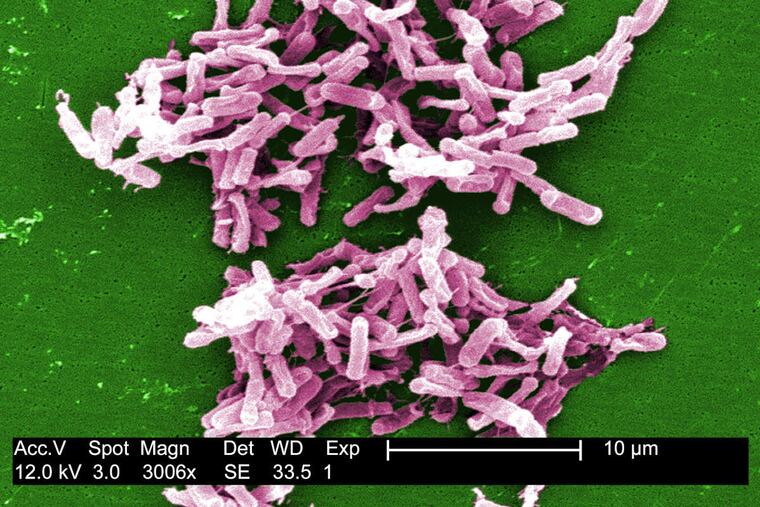
A new Penn study has uncovered a marked increase in a recurring and potentially deadly form of a common intestinal infection that can result in diarrhea, severe gut inflammation and fatal blood infection, especially among the elderly.
Intestinal infection with the bacterium Clostridium difficile — widely known as C. diff — is the most frequent healthcare-linked infection in the country.
By analyzing a nationwide health insurance database, researchers from Penn's Perelman School of Medicine discovered that the annual incidence of multiple recurring C. difficile infections increased by nearly 200 percent from 2001 to 2012, according to the study published online Monday in the Annals of Internal Medicine . During the same 11-year period, the rate of ordinary C. diff infections grew by only about 40 percent.
Cases of the bacterial infections are considered to have multiple recurrences when patients have been treated with at least three closely spaced courses of antibiotics. Ordinary C. diff infections clear up after one or two courses of medication.
It seems to flourish in people whose normal, healthy gut bacteria have been killed or reduced, sometimes as a consequence of medication, said study senior author James D. Lewis, a Penn gastroenterology professor. That may include antibiotics, proton-pump inhibitors or corticosteroids.
The most promising new treatment for recurring C. diff infections is fecal microbiota transplantation — infusing beneficial intestinal bacteria into patients to compete with C. diff, according to the study. Although the treatment has become more commonly used, and some research supports its use, additional study is merited, said Lewis.
"While we know that fecal microbiota transplantation is generally safe and effective in the short term, we need to establish the long term safety of this procedure," he said.
At one time, C. diff infections were seen almost solely in patients in hospitals and nursing homes. Increasingly, however, people who have not been hospitalized are getting the infections, Lewis said. The bacteria have the ability to encapsulate within spores, making them resistant to usual sterilizing procedures.
Although the rapid rise in recurring infections may be linked to the more frequent use of antibiotics and corticosteroids, it could also be due to the recent emergence of new strains of the bacteria, Lewis said.
For the Penn study, the researchers used a commercial database with records on more than 40 million U.S. patients with private health insurance.
The patients who contracted the recurring infections as opposed to the more easily remedied variety tended to be people who were exposed to antibiotics, corticosteroids or proton-pump inhibitor treatments, and they were more likely to be female. Those with the recurrent infections had a median age of 56, versus 49 for the less-severe infections.
The American Gastroenterological Association recently set up a registry for physicians to report their findings with fecal microbiota transplantation procedures. Lewis, a member of the steering committee, said it is a way for doctors performing the procedure to "contribute data to help answer these critical questions" about the longer term health effects of transplantation, a procedure that has long been used in veterinary medicine.