At home with hope
Joseph Beinlich's skin is pale. At 57, he walks about as fast as someone two decades older. He is OK with that, given the alternative.
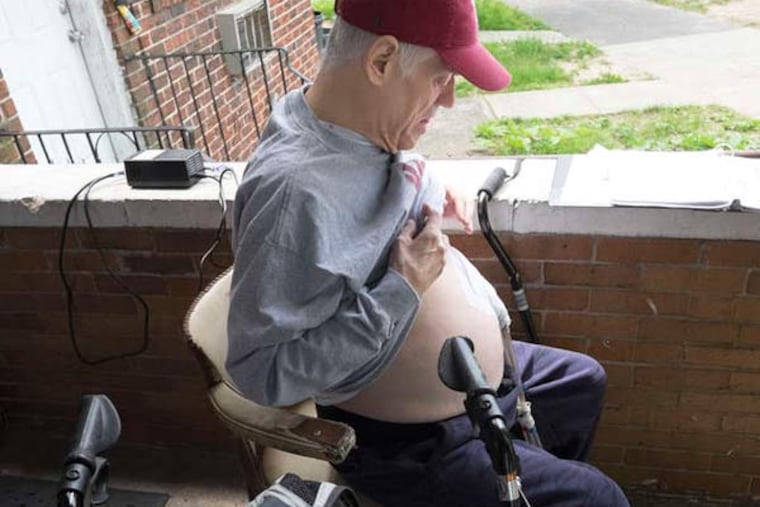
Joseph Beinlich's skin is pale.
At 57, he walks about as fast as someone two decades older.
He is OK with that, given the alternative.
"I'd rather be living than kicking up daisies," said Beinlich, of Philadelphia's Olney neighborhood.
Beinlich is being kept alive by an artificial heart. Temple University Hospital surgeons removed his own, badly diseased organ in August and replaced it with the 5.6-ounce plastic device.
More than 1,000 other patients have gotten the implants since the Food and Drug Administration approved them in 2004.
These days, some patients are able to leave the hospital, hooked to a portable, battery-powered "driver," instead of being tethered in the hospital to a clunky unit and cart that together can weigh well over 100 pounds. After a few months of recuperation, Beinlich in November became the first such recipient to go home from a Philadelphia hospital.
"Feels great," he said from his front porch, as his life-sustaining contraption beat with a soft but audible pip-pup-pip-pup.
Beinlich was followed by Mike Law, 65, who got an artificial heart at the Hospital of the University of Pennsylvania and went home this month to Westampton, N.J. Elsewhere in Pennsylvania, two more patients have gone home with artificial hearts from the Penn State Milton S. Hershey Medical Center.
The plastic hearts, made by SynCardia Systems Inc. of Tucson, Ariz., are approved for use as a "bridge to transplant" - a temporary fix until the patient can get a heart from a human donor.
The company is undertaking a study of whether the devices are suitable as "destination" therapy - permanent use.
Given the chronic shortage of donor organs, and the fact that many artificial-heart recipients do not live very long, the devices can end up being permanent anyway.
That's not necessarily due to the device, which is implanted in a two-hour operation. The patients who get them are generally very sick to begin with, said John Entwistle, who has implanted artificial hearts at Thomas Jefferson University Hospital.
"You have some patients where it's going to be very difficult to survive no matter what you do," said Entwistle, Jefferson's surgical director of heart transplantation and mechanical circulatory support.
In a 2012 study of 101 device recipients, 32 died within nine months of getting the implant, 29 of them within 40 days. The rest lived long enough to get a human-heart transplant. Complications associated with the device included stroke in eight patients, authors reported in the Journal of Thoracic and Cardiovascular Surgery.
According to the company, the longest-surviving patient made it nearly four years with an artificial heart before getting a transplant.
No matter how long they make it, the ability to go home is a boon for patients, said Rene J. Alvarez Jr., medical director of Temple's heart failure and transplant program.
"They can walk outside," he said. "They can go to a ball game. Psychologically, it's very important."
Beinlich goes fishing. Last month, he made the first day of trout season on the Pennypack Creek, a few miles from his house on busy West Roosevelt Boulevard.
Living with an artificial heart requires attention to detail. Someone has to be with the patient at all times in case something goes wrong. Beinlich's helpers include his brother, Rich, and a crew of friends.
"When this shuts off, he's dead," Rich Beinlich said, indicating the portable driver.
The driver operates the heart's valves by pumping air through plastic tubes that pass through Joe Beinlich's skin.
The Beinlichs have backup batteries at the ready, and they even got one of those briefcase-size power packs that can be used to jump-start a car.
The saga began in July, but in some ways, it had been years in the making.
Joe Beinlich had not been to the doctor in 20 years and suffered from uncontrolled type 2 diabetes and high blood pressure, said Eman Hamad, medical director of Temple's mechanical circulatory support program.
Beinlich often found himself getting short of breath at his job at the Sesame Place amusement park, where his tasks included working in the kitchen. It got so bad he quit smoking.
In late July, he checked in to Temple, where doctors determined he had suffered multiple heart attacks in the past. His ejection fraction - how much blood his heart was pumping with each beat - was a paltry 10 percent. Normal is about 60 percent.
In most heart-failure patients, the left ventricle is the one in trouble. They can be helped with an implanted pump called a ventricular-assist device.
In Beinlich, both ventricles were failing, so surgeons told him about the artificial heart. He was game.
After a few days hooked up to a heart-lung machine, he was stable enough to get the implant, which was covered by Medicaid.
According to Penn, Medicare reimburses providers anywhere from $142,000 to $230,000 for the device and the hospital stay.
The first long-term success with an artificial heart occurred in 1982. A patient implanted with the Jarvik 7 device lived for 112 days.
A later device, called AbioCor, enabled one patient to live 17 months, some of it at home. One of 15 patients to get that device had the operation at Hahnemann University Hospital in 2001 and said he regretted it because his health was so poor.
That product is no longer sold, leaving the U.S. market to the SynCardia heart.
Implanting an artificial heart is major surgery, involving opening the chest and removing the failed heart. Some surgeons have reservations about doing the procedure on the most frail patients, those who are hooked up to a ventilator and suffering from multiple organ failure.
Likely to die soon, such patients may be better off on a heart-lung machine, said Joseph Cleveland Jr., surgical director of cardiac transplantation and mechanical circulatory support at the University of Colorado Anschutz Medical Campus.
"The insult to them is less," Cleveland said.
In eligible patients, the gold standard remains a human-heart transplant. If a heart is available right away, it is an easier operation than if the patient first gets an artificial heart.
That is because the first operation causes the buildup of scar tissue, said Behzad Soleimani, surgical director of cardiac transplantation and mechanical circulatory support at Penn State Hershey.
But physicians hold out hope for a fully implantable device. Unlike the SynCardia, such a device would have an internal battery, so the patient would not be tethered to any external equipment. The battery would be recharged through the skin.
Beinlich would not mind that. His external driver, though far smaller than hospital-based drivers, still weighs 131/2 pounds.
"I won't miss this heavy thing on my back when I get my heart transplant," Beinlich said. "I'm going to do a happy dance."
That first day of trout season, Beinlich was unsuccessful.
"Cold air," he said. "No fish."
But he caught some fresh air along the Pennypack, and that was catch enough.
215-854-2430
@TomAvril1