Insurers look at virtual visits to doctor
If you could have the equivalent of a doctor's appointment - via the Web - without actually going to the doctor, would you do it? Are you willing to pay for it?
If you could have the equivalent of a doctor's appointment - via the Web - without actually going to the doctor, would you do it? Are you willing to pay for it?
Some doctors, medical information companies, and, most important, health insurers are betting that patients will fork over a co-pay or more for the convenience of describing their symptoms from work or home.
Online banking meets the house call.
Aetna Inc., one of Philadelphia's dominant insurers, and Cigna Corp., which is based here, have announced that they will pay for doctors' visits on the Web. Aetna expanded a pilot program in California, Florida and Washington to the rest of the country on Jan 1. Cigna will start paying in January.
"This is something that is taking off and has the potential to grow exponentially over the next few years," Cigna spokesman Joe Mondy said.
The insurers think their customers - employers - will like the service because it can improve efficiency and might prevent more expensive problems. Insurers pay less for a Web visit than for a meeting with the doctor, and employees don't have to miss work for an appointment.
The payments are another sign of how information technology is changing the doctor-patient relationship while creating new quandaries. Today's most tech-savvy doctors encourage patients to view lab results, make appointments, refill prescriptions, and discuss symptoms online. Some of them wonder how patients will react to charges for a service that had been free. Doctors who use e-mail less worry about losing the personal touch with patients and giving insurers more data. And patients are particularly concerned about privacy.
"I just don't trust computers with personal information," Jeffery Morris of Plymouth Meeting said last week as he ate dinner at the Plymouth Meeting Mall with Roosevelt Hall, a friend from Philadelphia.
Morris said he wanted a personal visit because a doctor might spot things Morris wouldn't notice. Neither man liked the idea of paying for virtual visits. "He gets paid when I walk in that door," Hall said of his doctor. "That's when the meter starts running."
But Marcia Sampson, a Colorado woman in Philadelphia last week for a convention, said Web messaging would be fine for some repeat problems. "An e-mail would save me a lot of hassle," she said. "I'd be willing to pay for that."
Even in states where they have been around a while, e-consults are unusual. In a survey of Californians last year for the California HealthCare Foundation, only 4 percent said they had e-mailed their doctors.
"It's still pretty much in its infancy, although I think it's going to rise," said Jonah Frohlich, the foundation's senior program officer.
At least initially, it will be tough to find a doctor offering the service in this area. RelayHealth, a California company that offers its 16,000 physician subscribers a secure Web site for administrative duties - such as refills and appointments - and Web visits, has only 93 physician members in Pennsylvania and 300 in New Jersey.
Robert Berenson, a senior fellow at the Urban Institute in Washington, which does economic and social policy research, said many e-mails didn't fit into the categories that insurers planned to cover. More "robust" communication will blossom, he said, when doctors are paid an extra fee for coordinating patients' care.
Edward Fotsch, chief executive officer of Medem, a company that provides 70,000 doctors with online services, said insurance coverage for Web consults made for a good press release, but didn't cost insurers much. "The actual utilization of e-consults is just incredibly low," he said. They account for fewer than 5 percent of the transactions on Medem Web sites. The primary reason doctors buy his service, he said, "is to make their practice more efficient."
Horizon Blue Cross Blue Shield of New Jersey tried paying for Web visits about four years ago and gave up. "I don't think the market was ready for that level of technology," said Richard Popiel, Horizon's vice president and chief medical officer. He thinks things have changed, he said, and the company is talking about trying again.
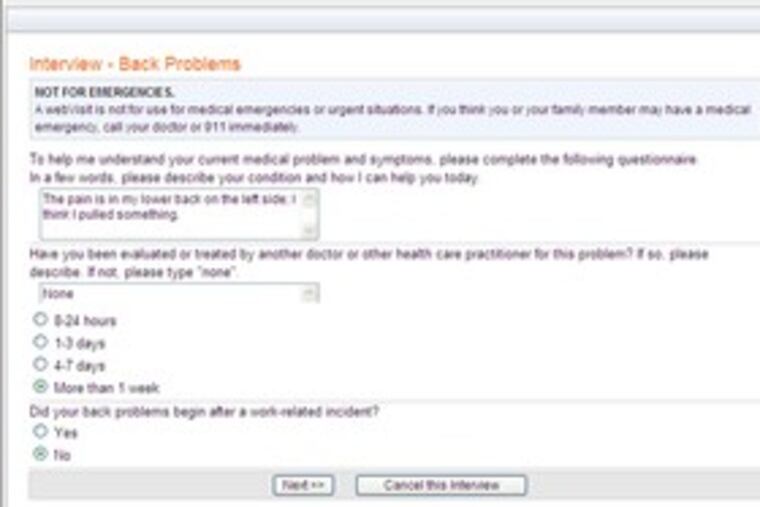
Aetna and Cigna contract with RelayHealth. The insurers pay only for Web visits, which are more than the simple messages you might send a friend. Patients fill out questionnaires about their symptoms, reducing the chance of leaving out crucial information. The company has a list of 150 ailments, including acne, erectile dysfunction and sinus pain, considered appropriate for e-visits.
Cigna patients will have their usual co-pay, often a percentage of the total bill. Doctors get $25 for a Web visit and about $65 for an office visit. Aetna pays doctors $25 to $35 for a Web visit and $35 to $100 or so for an office visit. Its subscribers have the same co-pay for either. Those in high-deductible plans might pay the whole fee.
This region's largest private health insurer, Independence Blue Cross, does not pay for Web visits, but is participating in a project that will offer some doctors incentives to use more information technology. The nation's most influential payer - Medicare - also does not pay for this kind of care.
Daniel Wolk, the self-described geek of the Medical Group at Marple Commons, has been using RelayHealth's Web consultation for close to four years.
He does only about two Web visits a week. They take him about five minutes each, and he has been doing the work for free. "I'm afraid if I started charging for the services, some patients would start making phone calls instead," he said.
He finds the services that insurance won't cover the most useful. He enjoyed ordering a prescription while he was out of the country. When he sent a patient results from a liver test last week, he included links to information the patient needed.
"I think it's better-quality information for the patient," he said.
Wolk's partner, Janet Specter, isn't a Web-visit fan. She said she worried about security and thought she would miss too much by not being able to hear and see patients. She said patients misdiagnose their ailments about 80 percent of the time. "So many times, you find not at all what they thought was happening."
Lisa Rankin is a doctor in Port St. Lucie, Fla., one of the first states where doctors got paid for Web visits. For a patient without insurance, she said, a Web visit is cheaper than going to the office. It saves others the hassle of missing work. Meanwhile, she collects a little money from people who might otherwise try to use the phone. "There definitely is a nice niche for it," she said.
Can charges for phone calls be far behind?
Health experts say some doctors already charge for calls, especially after hours. But, they say, it's harder to document phone calls than Web contacts, a difference that likely will keep insurers from paying. Doctations, a new company in Long Island, N.Y., offers a compromise: Web consults that use the video and audio capability of most laptop computers.
Many beleaguered doctors like the idea of charging for phone time, as lawyers do, though they don't really think that will happen.
Frederic Becker, a primary-care doctor in King of Prussia, said the three doctors in his practice made 75 to 100 phone calls a day. He thinks they should be paid. "Of course we should be. It's time," he said. "I must spend an hour and a half on the phone a day. My compensation is zero for it."