Putting a freeze on heart attacks
A new cooling treatment is being tested to see if it can limit the damage to victims.
NEW ORLEANS - It took five mighty shocks to get Cynthia Crawford's heart to start beating again after she collapsed at Ochsner Clinic a few weeks ago. A dramatic rescue, to be sure, yet still routine.
What came next, though, was not.
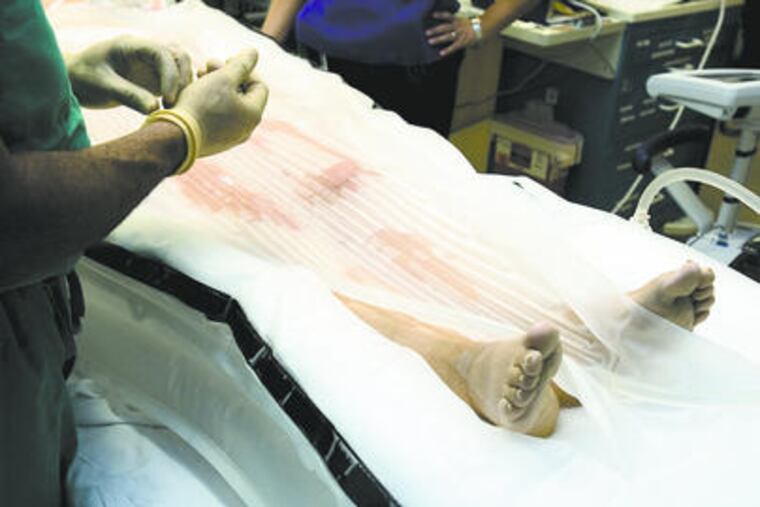
As she lay unconscious, clinging to life, doctors put her in an inflatable cocoon-like pool that sprayed her naked body with hundreds of icy jets of water, plunging her into hypothermia.
"Like jumping in the North Sea," said her lead cardiologist, Paul McMullan.
Days later, Crawford was recovering without the brain damage she might have had.
For years, doctors have tried cooling people to limit damage from head and spinal cord injuries, strokes and even prematurity and birth trauma in newborns. It's also used for cardiac arrest, when someone's heart has stopped. In January, New York will join several other cities requiring ambulances to take many cardiac arrest patients to hospitals that offer cooling.
Now doctors will be testing a new and dramatically speedier way of doing this for a much more common problem - heart attacks, which strike a million Americans a year.
"It's extremely appealing" because the cooling system is non-invasive and can be used in an ordinary hospital room, said George Sopko of the National Heart, Lung and Blood Institute, which is paying for this first-of-a-kind study.
Animal research suggests it will help, "but we need the hard evidence" from human tests to know, he said.
Heart attacks occur when an artery gets blocked, depriving the heart muscle of oxygen and blood, and causing part of it to die. But the damage does not happen all at once - cells die off slowly, sending chemical messages that make nearby cells do the same. Cooling the body to around 90 degrees from its usual 98.6 slows this down.
"Tissue that would have died, were it not cooled, can stay alive," McMullan said.
Surgeons use cooling now during open-heart surgery, and promising results from a few studies several years ago led the American Heart Association to recommend it for cardiac arrest patients, whose hearts have stopped.
"The problem with all these trials is the cooling was too slow," taking up to six hours with some devices, said the leader of a key study, Michael Holzer of Medical University of Vienna in Austria.
Doctors at Ochsner (pronounced OSH-ner) have high hopes for the ThermoSuit, made by Life Recovery Systems in Waldwick, N.J. A pump rapidly inflates the pool-like suit until it puffs up tightly around the patient as doctors Velcro on a plastic topsheet. Tubes spray naked patients with frigid water as other tubes drain it away. McMullan has used the suit on 12 cardiac arrest patients, like Crawford, and cooled them to around 90 degrees in as little as nine minutes, typically in about half an hour. "That's the kind of speed we're going to need" for this to be practical," said Lance Becker, a University of Pennsylvania doctor and a Heart Association spokesman.