‘Not disposable people’: Patients on ventilators caught in the middle as nursing homes bleed money
Several Pennsylvania nursing homes say bankruptcy is a real risk because the state isn't paying them enough to cover the cost of providing critical care for patients on ventilators.
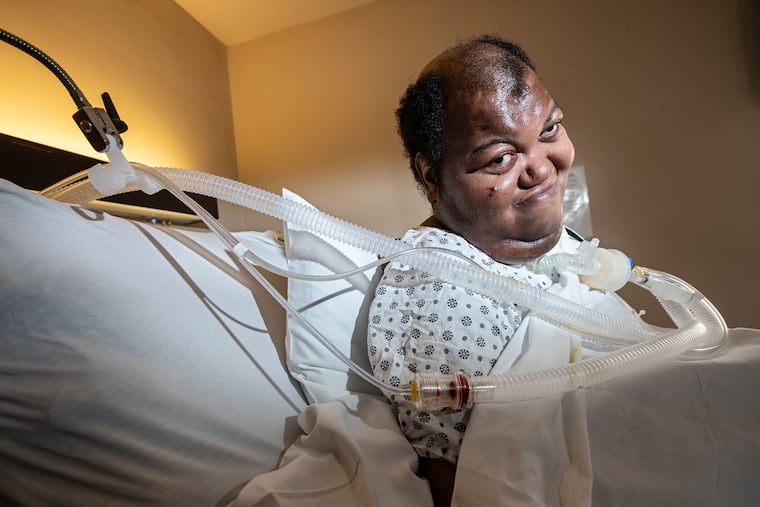
Fox Subacute Care in Warrington has been home for Zafir Boroughs since 2008.
The 36-year-old, who suffers from a rare muscle degenerative disease and needs a ventilator to breathe, urged a visitor to look at his wall plastered with posters of comic-book heroes, all given to him by Fox staff.
It’s more than a community, said Boroughs, a big man who sprinkles conversation with gently sarcastic asides. “It’s a family.”
Last month, Boroughs learned that Fox had filed for bankruptcy and might go out of business without a state rescue. Since then, he has been experiencing anxiety.
“It’s incredibly scary, the thought of losing your home. In my case, it’s more scary because I can’t just go find an apartment,” said Boroughs, who moved out of his parents’ house more than a decade ago because he wanted his independence.
Boroughs and hundreds of other Pennsylvania residents have been caught in a squeeze between the state and nursing home operators who say it costs as much as $200 more per day than what the state is reimbursing them for the care of patients like Boroughs.
If the state can’t come up with more money, providers warn that Pennsylvania could see a cascade of nursing home closures.
While it’s not unusual for nursing homes to bemoan low Medicaid rate, significant fallout has already started among nursing homes with beds for ventilator-dependent patients.
The Pennsylvania Department of Health counts 10 facilities in Southeastern Pennsylvania with 424 beds available for patients dependent on ventilators. Since August, three of those Philadelphia-area facilities have taken 79 beds — nearly one in five — out of service.
An additional 233 local ventilator beds at Fox and another facility that also takes only ventilator patients are in jeopardy, the owners said.
Statewide, there are 26 nursing homes that allot 921 beds for ventilator-dependent patients.
State officials say they are monitoring the situation affecting the nursing homes with ventilator patients and those with tracheotomies.
“Right now there are enough beds to meet the needs of people with need for vent-trache services, but that doesn’t mean that will be the same condition three to six months from now,” said Kevin Hancock, a deputy secretary at the Pennsylvania Department of Human Services overseeing long-term services for the elderly and disabled Medicaid beneficiaries.
Funding struggles are not unusual in the world of Medicaid, where reimbursement rates are notoriously low, forcing providers to rely on higher rates from other insurers to subsidize Medicaid.
State officials have suggested that providers with only ventilator patients might benefit from taking some lower-cost patients who are not on ventilators. But, despite having that suggested patient mix, some Philadelphia-area nursing homes were forced to cut back or stop taking ventilator patients.
Statesman Health & Rehabilitation Center, in Levittown, closed a 30-bed ventilator unit last month, and Deer Meadows Rehabilitation Center, in Northeast Philadelphia, closed its 23-bed unit in October. And, AristaCare at Meadow Springs, in Plymouth Meeting, reduced capacity to 50 from 76, starting in August.
“We put in a self-imposed quota on the number of vent patients that we’re going to have at any particular time, because we’re ready for doom and gloom,” said Sidney Greenberger, AristaCare’s chief executive.
Operators have long complained about insufficient rates, but what brought things to a head, they say, is a major change in the way Pennsylvania Medicaid pays for long-term care.
Instead of paying nursing homes directly, Pennsylvania hired three managed-care companies to administer Medicaid payments for nursing homes and other long-term services, including community-based supports, for the elderly and disabled.
Under the old system, rates were set based on costs. However, nursing homes typically would get paid 15 to 20 percent less than the rates, depending on the state’s annual budget allocation for health care.
To prevent care disruptions as the new system started, the managed-care companies were required to contract with all nursing homes that took Medicaid and pay them per-day rates that were no less than those they received in 2018 under the old system.
Those rates were a floor under initial three-year contracts, state officials said.
Ultimately under the new system, the managed-care companies are expected to negotiate rates with nursing homes and other service providers. The ventilator specialists believed they would be able to get higher rates that way.
That did not happen, nursing home operators say. They say the three managed-care companies, Independence Health Group’s AmeriHealth Caritas, Centene Corp.'s Pennsylvania Health & Wellness, and UPMC Community HealthChoices, have refused to negotiate rates closer to the cost of caring for ventilator patients.
That was too much for Fox Subacute to take, after already losing $27 million on $142 million in revenue at its four nursing homes over the last five years, according to public records. The facility, where 70 percent of the patients are on Medicaid, was banking on being able to negotiate higher rates under managed care for nursing homes, formally called Community HealthChoices.
“We thought we would get it resolved when managed care came in. It didn’t happen,” said Joseph F. Murray, general counsel at Fox Subacute, which is based in Plymouth Meeting. Murray said Fox receives about $500 a day from Medicaid for ventilator patients. The care costs about $630 per day, he said.
AmeriHealth and Centene did not comment. UPMC said it is working on new payment arrangements “that could help nursing facilities that provide high quality care to some of our most medically vulnerable members.”
Like Fox, Tulip Special Care, in the East Falls section of Philadelphia, takes only ventilator patients. The 60-bed nursing home on the seventh floor of the former Medical College of Pennsylvania Hospital is unusual, however, in that it opened in 2018, just six months before the Medicaid payment system started in Southeastern Pennsylvania.
That meant that the rate floor for Tulip did not capture the acuity of the patients it serves, said J. Edward Burleigh III, Tulip’s CEO. “We’re behind, and we’ll never be able to catch up unless they renegotiate with us."
How long can Tulip hang on?
“It can’t last too much longer,” said Michael F. Young, an investor in Tulip, which spent $4.5 million on construction. “There has to be a real understanding of what it costs to run this level of facility.”
If Tulip can’t survive, that would displace patients like Robert Hillsee, 66, from Northeast Philadelphia. At home he uses a ventilator at night and was at Tulip this month for rehabilitation of his right leg, which lost its strength after he spent a long time in bed after his left leg was amputated.
“I can’t stand,” Hillsee said. “I’m just weak all over.”
The only nursing home in Delaware County that takes ventilator patients, Aventura at Prospect, is bucking the trend by keeping its 30-bed unit open.
Facility administrator Aharon Franco said the home, with new owners for about a year, wants to be a community partner. “Right now, that’s the need. There are no other vent beds. Everybody is just shutting their doors,” he said.
An effort to help the facilities is underway in Harrisburg.
State Sen. Camera Bartolotta, a Republican representing Southwestern Pennsylvania, recently cosponsored a bill that would provide $7 million more annually, or up to an additional $130 a day per ventilator patient statewide. Still, this late in the year, the measure would need a miracle to become a reality.
“We were so hoping it would be something that would be a wonderful Christmas gift to a lot of these families who are extremely nervous and wary of what’s going to be happening to their loved ones in these homes that are really financially strapped,” said Bartolotta, who is cosponsoring the bill with Republican colleague Dan Laughlin, who represents Erie County.
“These are not disposable people,” said Bartolotta.
