Prescriptions — and overdoses — are skyrocketing for anti-anxiety drugs that make opioids even more lethal
Experts say an explosion of benzodiazepine prescriptions in the middle of an opioid crisis is particularly concerning, because both drugs become much deadlier when mixed with each other.
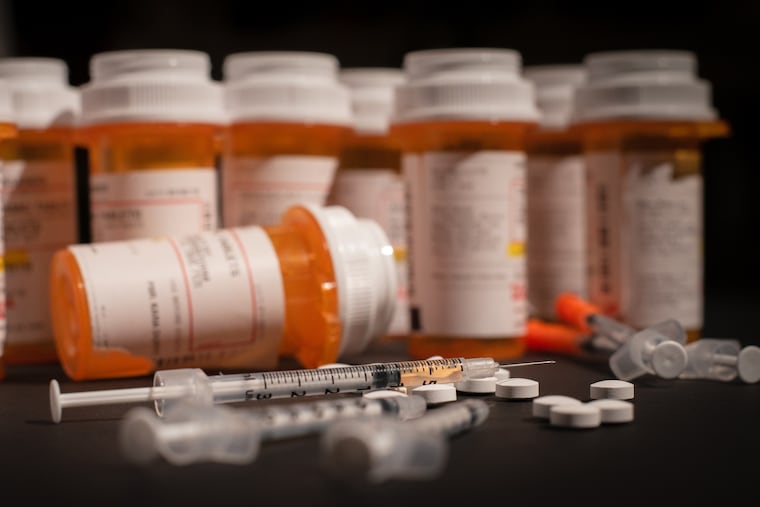
Even as health officials around the country struggle to get a handle on an opioid overdose crisis that caused a record-breaking number of deaths last year, doctors and researchers are sounding the alarm on another class of drugs that they say are prescribed far too often -- and which themselves are behind an increasing number of overdoses.
Prescriptions for benzodiazepines -- which include the common anti-anxiety drugs Xanax, Ativan, and Klonopin -- have skyrocketed over the last 15 years, following the same kind of trend lines that opioid prescribing did before doctors and insurance companies began to seriously curb pain-pill prescriptions.
Doctors have long warned about the potential addictive properties of “benzos" -- but an explosion of benzodiazepine prescriptions in the middle of an opioid crisis is particularly concerning.
That’s because both drugs become much deadlier when mixed with each other. In 2014, according to data from the Centers for Disease Control and Prevention, about 30 percent of opioid overdoses also involved benzodiazepines. And since 2012, the vast majority of overdose deaths associated with benzodiazepines in Philadelphia have also involved opioids. The combination was behind more than a third of the city’s fatal overdoses last year.
“They’re two drugs that are sedating and slow down your central nervous system,” said Abigail Kay, a psychiatrist, associate dean at the Sidney Kimmel Medical College, and former medical director of Jefferson Hospital’s Narcotic Addiction Rehabilitation Program. “If you combine them, they become stronger and more dangerous.”
Rick Pescatore, director of clinical research in Crozer Keystone Health System’s department of emergency medicine, often sees overdose patients who revive only after multiple doses of Narcan, the overdose-reversing drug. “There’s this supposition that it’s extremely powerful opioids, when more often, it’s co-ingestion with benzos,” he said.
A June study in the Journal of the American Medical Association found that Medicare Part D beneficiaries prescribed benzodiazepines and opioids at the same time were five times more likely to overdose in the three months after they began to use the drugs together, compared with people who used only opioids.
And, Kay said, even in a time when doctors have been heavily pressured to stop prescribing opioid pain pills, she’s often shocked at how willing her colleagues are to prescribe benzodiazepines.
“It amazes me how many doctors hand it out like candy,” she said.
Between 1996 and 2013, the number of adults who filled a benzodiazepine prescription increased by 67 percent, according to a 2016 study published in the American Journal of Public Health. And a 2017 study in the British Medical Journal that looked at more than 300,000 Americans with private insurance found that the number of people who were prescribed opioids and benzodiazepines at the same time increased by 80 percent between 2001 and 2013.
A Bucks County woman named Jean, who’s been using heroin on and off for the last several years and who did not want to give her last name because of concerns about her privacy, said she saw a psychiatrist for anxiety five years ago who prescribed her Klonopin on her second visit. She didn’t tell her doctor she was using opioids at the time, she said, but it was immediately clear how powerful the two drugs were when used in combination.
“I was way more tired and out of it. I would trip down the stairs. I would fall asleep at work,” she said. “I would go through my prescription in less than a week, and then I would start buying on the street.” Eventually, her parents told her doctor she was using heroin, and her prescription was cut off.
Even for patients in opioid recovery, benzodiazepines can serve as another temptation. Many of Kay’s patients on methadone or other opioid-based medication-assisted treatment also test positive for benzodiazepines, sometimes prescribed by another doctor, or purchased on the street. Prescription-drug monitoring programs can help curb the former, Kay said, but the problem persists.
Yaya Lifford, 24, of Baltimore, said he started using opioid pain pills at 16, and quickly realized that a Xanax pill would enhance the high. “And then I wouldn’t do a Percocet until I ate a Xanax,” he said. That was his routine until one day eight months ago. His addiction had led him to the streets of Kensington, where he purchased a bag of what he now believes was heroin laced with fentanyl, the powerful synthetic opioid behind most of Philadelphia’s overdose deaths.
“I died -- my heart stopped. I was three, four Xanaxes in, and then I’m waking up strapped to a chair. They were like, ‘We had to bring you back to life,’” Lifford said. “That was when I knew it wasn’t a joke.”
A few months later, Lifford went to in-patient rehab and began a methadone maintenance program. The drug curbed his craving for opioids, but he found himself unable to stop thinking about Xanax, and the high he might feel if he took it with methadone. “There were four people in rehab with me trying to get off methadone and benzos," he said. “It was another addiction in itself.”
Experts are careful to note the benefits of both opioid pain pills and benzodiazepines for some patients. “Benzos are effective medications when you use them in combination with small procedures, or if you need to treat someone who is acutely agitated, and you can use them in the short term for anxiety,” said Jaakko Lappalainen, chief of addiction psychiatry at Crozer. Kay prefers to treat anxiety with anti-depressants -- which don’t have the immediate calming effect of benzodiazepines, but are safer to use for longer periods of time.
Benzodiazepine withdrawal, Lappalainen said, can be particularly dangerous -- similar to withdrawal from heavy alcohol use. Mild withdrawal symptoms include restlessness and anxiety, muscle shaking and jerks; severe withdrawal can induce seizures, which can be fatal.
Lappalainen said people trying to reduce their benzodiazepine use are usually tapered off the medication over a longer period of time or recommended to an in-patient detox because quitting cold-turkey can be so dangerous.
Still, Pescatore said, it’s no surprise that benzos have become so popular, and so prevalent. These are anxious times, and patients who turn to benzodiazepines or opioids are often trying to escape larger underlying problems -- chronic pain, trauma, economic distress and persistent health problems. But, he said, doctors can’t repeat the mistakes of the opioid crisis.
“This is a symptom of a deeper disease,” he said. “And this is something we need to get out ahead of.”