At PHMC’s medical respite, homeless Philadelphians get desperately needed care
When they leave the hospital, some homeless Philadelphians are still too sick to stay in a shelter. Medical respite beds fill the gap.
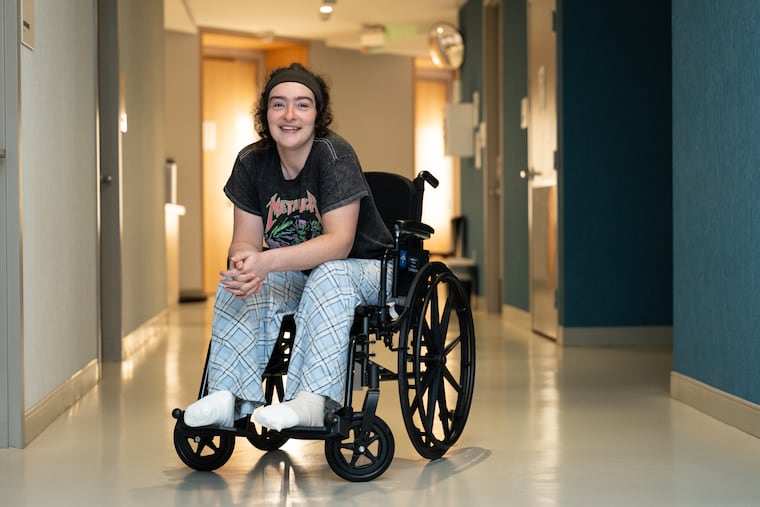
After months of living on the streets, Alexis DiBella felt she had finally turned a corner at the end of last year.
The 31-year-old had just gotten a bed in a women’s shelter. Excited to “to dig into life again” after a frigid winter, she brushed off some lingering pain in her feet.
Over a few days, they grew red and swollen. One night, still in her first week at the shelter, DiBella took off her socks and shoes and discovered that both feet had turned black.
She had developed frostbite while living outside.
Doctors eventually amputated one of her feet. After a month in the hospital, DiBella was ready to be discharged — but the shelter where she’d hoped to start a new life could not accommodate her disability.
“I didn’t know where I was going,” DiBella said.
That’s when a social worker recommended she move to a medical respite in West Philadelphia run by the Public Health Management Corporation, a healthcare organization that runs several federally qualified health centers and health programs for homeless Philadelphians.
Medical respites are shelters specially equipped to house people with medical needs that are not severe enough for hospital care, but exceed the care available at traditional shelters.
The Medical Respite on Cedar, where DiBella has lived since January, has 20 beds and opened in 2023. An additional 20 beds are available at the Medical Respite at Serenity Court, a facility in North Philadelphia that opened in 2014. They are the only shelters of their kind in the city.
Nationwide, there are 237 medical respites in 45 states; Pennsylvania has five total medical respite programs, and New Jersey and Delaware operate one apiece, according to the National Health Care for the Homeless Council.
The respites help patients with a wide range of medical conditions, from diabetes complications to ongoing cancer treatment. A few years ago, there was an influx of patients with wounds from xylazine, the animal tranquilizer then ubiquitous in Philadelphia’s illicit drug supply. Lately, after a particularly severe winter, the respites have dealt with another type of wounds: complications from frostbite, like DiBella’s.
“So many young folks are coming in here with either finger or toe amputations,” said Sabrina Thigpen, the Cedar respite’s program administrator.
PHMC began floating the idea of a medical respite after hearing from its nurses working with shelters across the city about residents with medical needs that required more attention than a traditional shelter could provide, Thigpen said.
Both facilities are consistently full and operate waiting lists. “We know that 40 beds for an entire city doesn’t meet the need,” said Jake Becker, PHMC’s managing director.
Medical respites exist in other cities around the country and share common funding challenges. “Who takes responsibility for the healing of people that are too well to be in a hospital and too sick to be on their own?” Becker said.
The respites are hoping to find funding to expand into more complex care, like delivering intravenous antibiotics, he said.
Insurance coverage for patients can be complicated, and many respites operate by cobbling together funding from partnerships with hospitals and other healthcare organizations. Together, PHMC’s respites have a $5 million operating budget and receive $50,000 from the city; the rest comes from healthcare institutions who pay set rates to send patients to the respites.
“We would love to be able to step up our capacity for services to bridge even more of the gap,” Becker said.
Mayor Cherelle L. Parker has proposed adding 1,000 new shelter beds in her fiscal year 2027 budget. Though details about her plan to fund the Office of Homeless Services have not yet been released, advocates hope it will include some money for medical respite beds, said Joshua Shipper, the senior director of advocacy and public policy at Project HOME, the prominent housing and homeless services nonprofit.
» READ MORE: In frigid temperatures, service providers work to get Philadelphians out of the cold
Project HOME has been working with PHMC to advocate for more funding for medical respite beds, either through partnerships with health systems or funding from the city, Shipper said.
“Any approach should seriously consider a variety of types of beds — long term, short term, and medical respite,” he said. “We want options for people to receive care, especially if that care does not quite rise to the level of hospitalization, so that hospitals are able to free up beds and treat those with really serious conditions.”
Typically, patients stay at Philadelphia’s respites for about 60 days, but some stay longer. The goal, staff say, is to find them consistent housing by the time they leave. Sometimes, patients find friends at the respite and opt to live together once discharged: Recently, several women who’d become close at the respite rented a house together, Thigpen said.
The Cedar respite has a cafeteria, group meeting areas for patients, and hospital beds — two to a room, with a few single rooms for patients who are immunocompromised.
Staff care for basic medical needs and arrange transportation for higher level care, like cancer treatment. They also connect patients with other services, like housing assistance or substance use treatment.
Even if patients return to the street after their time at the respite, staff hope to connect them with a support system and more stability.
“This is a stepping stone,” said Carl Graves, 52, who has been receiving treatment at the respite for a wound on his leg. Six years ago, he was shot three times and developed an addiction to the pain medication he was prescribed, which eventually landed him on the streets.
His time at the respite has helped him stabilize medically, but also reconnect with family and address symptoms of post-traumatic stress disorder from his shooting. “I’m just happy for the second chance,” he said.
He and DiBella became friends while staying at the respite. Like Graves, DiBella is not yet sure where she’ll live after leaving Cedar. But DiBella said she’s connected with social workers who will help her secure housing when she’s ready to be discharged.
DiBella is sometimes overwhelmed by how much her life has changed in the last several years, from a stint in jail, which resulted in losing her housing, to the months on the street and the amputation. But she’s grateful that she was able to recover at the respite.
“If I didn’t go through what I went through, I would have never found this place,” she said.