Patients on high doses of opioid painkillers risk overdose when tapering, study finds
“There are risks of starting opioid therapy, and risks of continuing therapy. But there are also risks to attempting to stop therapy,” said the study's lead author.
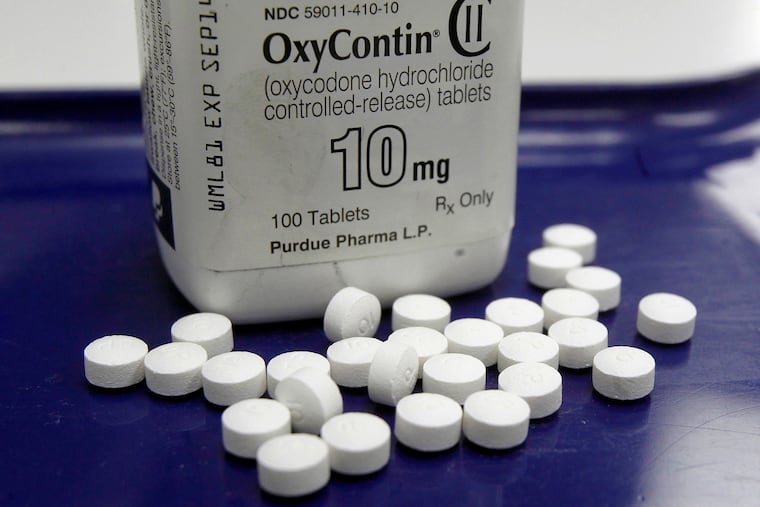
Long-term pain patients on high amounts of opioid painkillers who taper their dose are at a higher risk of suffering a mental health crisis or an overdose, a new study has found.
Researchers at the University of California, Davis, looked at a database of more than 113,000 patients prescribed higher doses of opioid painkillers between 2008 and 2019 -- an average of about 50 morphine milligram equivalents per day -- for at least a year. From there, they identified patients who had tapered their dose, which researchers defined as reducing it by at least 15% over a 60-day period.
Researchers found that the group of patients who tapered experienced a 68% increase in overdoses and twice the number of mental health crises compared with patients who stayed on their normal dose of medication, according to a university news release. Those risks were even more pronounced among patients whose original doses were higher and who reduced their doses more quickly. The report did not explain how patients overdosed.
The overprescription of opioid painkillers is widely blamed for the skyrocketing overdose crisis in the United States. The trend started in the 1990s, when drug manufacturers advertised opioid painkillers as nonaddictive and encouraged doctors to treat pain as a “fifth vital sign.” That led to a flood of opioid painkillers in the conventional and illicit markets, and a spiraling addiction and overdose crisis whose ramifications are still felt today. In 2020, some 93,000 Americans died of overdoses, more than in any other single year.
Around the country, state officials, insurance companies, and pharmacies have cracked down on overprescribing by instituting prescription caps and intense monitoring of opioid painkillers. But the UC Davis study suggests that heavy-handed efforts to get long-term pain patients off of opioids can also put them at risk.
“There are risks of starting opioid therapy, and risks of continuing therapy. But there are also risks to attempting to stop therapy,” said Alicia Agnoli, a physician and assistant professor in the department of family and community medicine at UC Davis, and the study’s lead author. “What [the study] really speaks to is there is not a one-size-fits-all approach to opioid prescribing. Things like dose ceilings and forced tapers are generally not beneficial to large populations of patients.”
She said she was surprised by how closely tapering and overdoses and mental health crises were related. And while patients who started at higher doses of painkillers and tapered rapidly had a higher risk of an overdose or mental health crisis, patients on lower doses who tapered at a slower rate still had some risk of an adverse outcome.
It’s crucial for physicians to give patients more support while they’re tapering off opioids, she said -- and for policymakers to reconsider policies around opioid prescribing that might not be adequately preventing overdose.
Stigma and shame around opioid use and addiction can contribute to a heavy-handed approach to prescribing and tapering that’s dangerous for patients in general, said Agnoli, who treats both pain patients and people with substance use disorder in her primary-care clinic.
“There are almost no chronic conditions I can think of where you look at medical maintenance and say, ‘When are you going to get off it?’ We don’t ask diabetic patients when they’re going to get off their insulin. We reevaluate the need for those medicines at regular intervals and employ every tool we have to treat the underlying causes,” she said. “These are strategies that apply to depression, high blood pressure, diabetes, asthma, and we seem to really struggle with applying that to both complex chronic pain and substance use disorder.”
