This isn’t just flu season. For millions, it’s also sinusitis season.
Good sinus hygiene might help you prevent a sinus infection.
Fourteen-year-old Dawit “D.J.” Debebe, a freshman at Perkiomen Valley High School, had long struggled with allergies, but something new, and much worse, attacked his sinuses in September.
He started having headaches so painful he had to sit out football practice. He worried he might have a concussion. “It was just constant pain,” he said.
The pain was so “horrific” that his mother, Victoria Debebe, took him to an emergency department. An MRI revealed that all of the sinuses on his left side — air-filled cavities in the skull that produce mucus and, ideally, wash away impurities — were not only completely clogged, but that bone surrounding the larger sinuses was bending from the force of the trapped mucus.
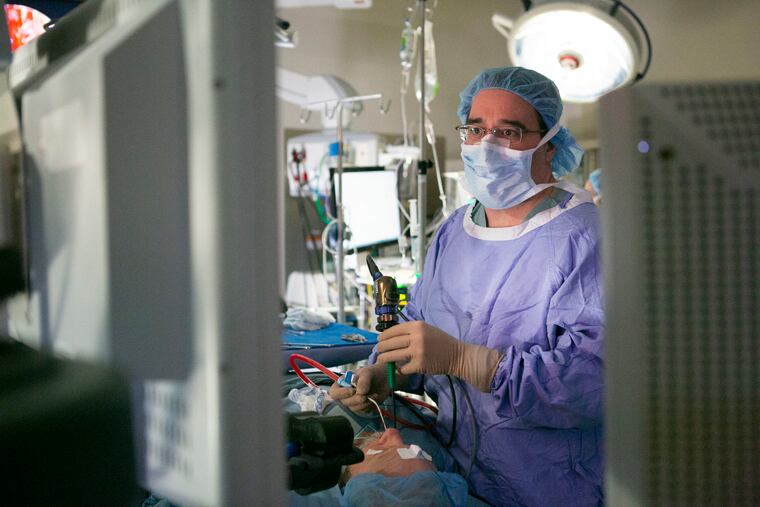
Antibiotics and steroids were no help. James Palmer, director of rhinology (sinus surgery) at Penn Medicine, concluded an allergic immune response to fungus was the problem. The only reliable treatment was endoscopic sinus surgery, a procedure done from inside the nose without outside incisions.
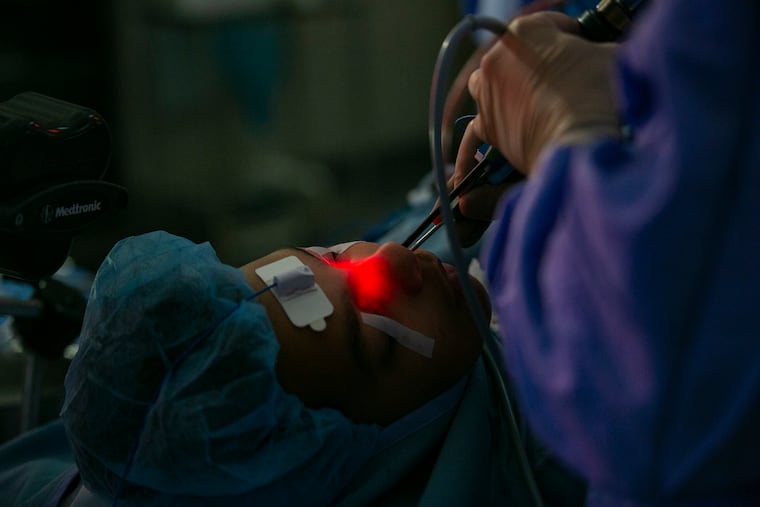
So D.J. found himself last month in an operating room in Penn’s Perelman Center for Advanced Medicine, blissfully anesthetized as Palmer pulled thick green blobs of infected mucus from his nasal passages and snipped and drilled away at a honeycomb of thin, nonessential bones in his sinuses to improve drainage. All the while a light inserted in D.J.’s nose to illuminate Palmer’s work made the teen’s nose glow like Rudolph the Red-Nosed Reindeer. Once Palmer opened up the clogged sinus, the entire center of D.J.’s face glowed an intense red.

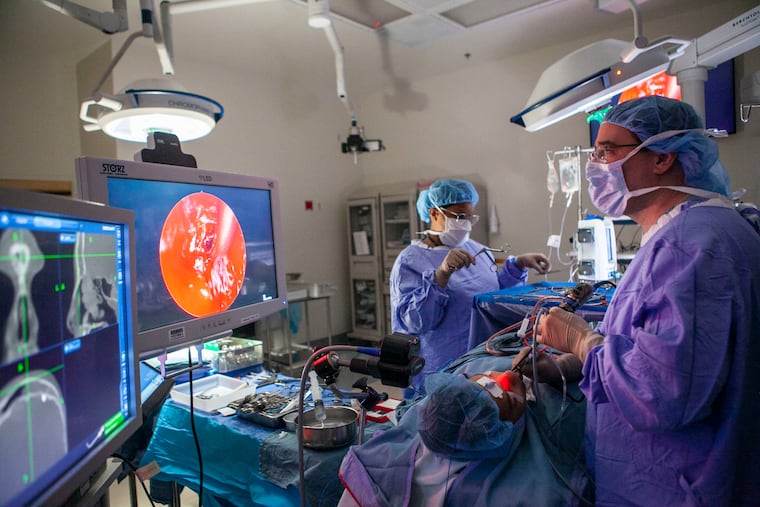
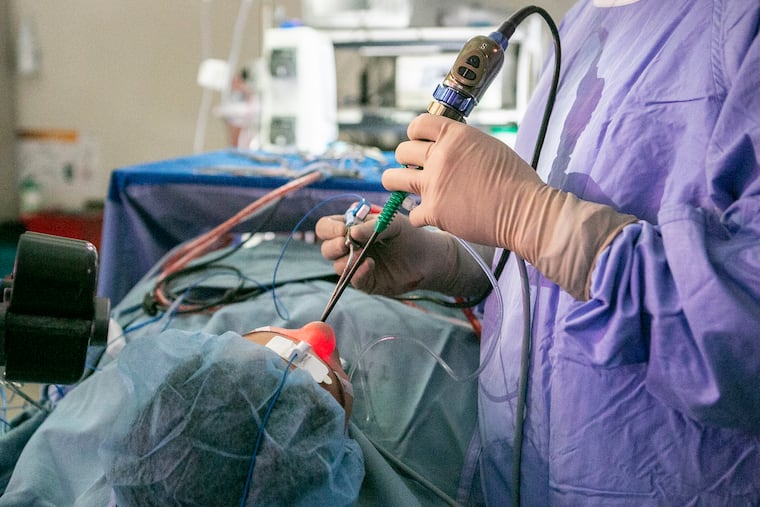
D.J. is an extreme example of what can go wrong with sinuses. But each fall and winter these little caves in our heads torment millions with pain, pressure, and thick, yucky mucus that lengthens the misery after seasonal viral ailments have run their course.
This is not just cold and flu season. It’s sinusitis season.
You can get a sinus infection at any time of the year, but doctors say they see more patients with sinus complaints in fall and winter because cold, dry air and respiratory bugs set the stage for sinus malfunction.
Unlike the flu, sinus infections rarely kill, but they are still a big deal. Count yourself lucky if you’ve never had a clogged sinus make it feel as if your head might explode. According to the U.S. Centers for Disease Control and Prevention, 29 million adults — 11% of the population — were diagnosed with sinusitis in 2018. Palmer says 5% to 20% of the population has chronic sinusitis — sinus inflammation that lasts more than a couple of months. The American College of Allergy, Asthma and Immunology estimates that people spend $1 billion a year on over-the-counter medications and $150 million on prescription drugs for sinus infections. Twenty percent of outpatient prescriptions for antibiotics are for sinus infections, said Noam Cohen, a Penn Medicine otorhinolaryngologist, or ear, nose, and throat (ENT) doctor.
» READ MORE: Flu now widespread in Pennsylvania, causing 5 deaths
Troubling as they can be, sinuses are also weird and interesting. “There’s an entire world inside your nose. ... It’s a window to your entire body,” Palmer said. “Sinuses are a reflection of the overall health of the patient a lot of times.” Sinus malfunction, he said, has been associated with sleep, heart, and lung problems.
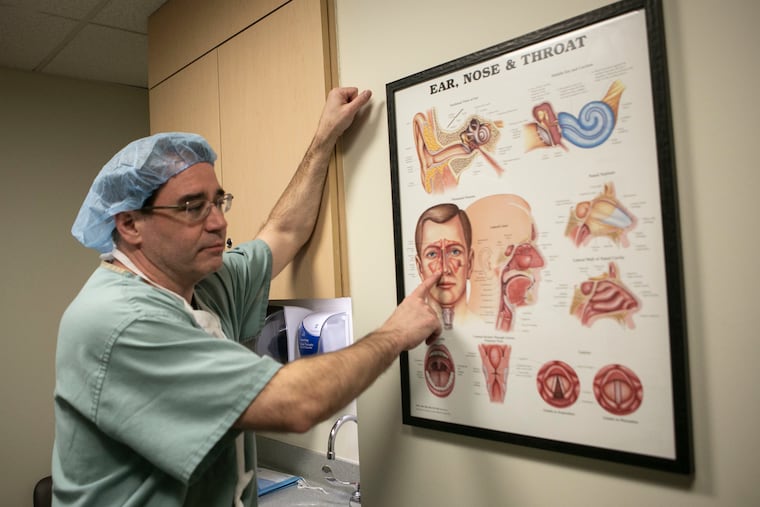
What are sinuses?
The sinuses are connected, hollow cavities in the skull that run behind the center of the face, from the forehead to beneath the cheekbones. Connecting the larger sinuses is a labyrinth of smaller sinuses. People can have six to 20 of those in configurations that are as different as fingerprints, Cohen said.
Palmer said they warm, moisturize, and filter air before we draw it into our lungs. They also lighten our heads a little bit and act like a cushion in a trauma. If you’re hit hard in the face, the sinuses will crumple in a way that protects your eyes and brain, Cohen said. Each day, the sinuses produce a quart or more of mucus, which traps bacteria, and, ideally, ushers them out holes that drain into the throat. Those holes are really small, from one to two millimeters in diameter.
What is sinusitis?
We’re most likely to worry about sinus infections, but you don’t necessarily need bacterial infection to have nasty sinus symptoms. Doctors more often use the broader term sinusitis or rhinosinusitis, which refers to inflammation and swelling in the nose and sinus cavities that lead to poor sinus drainage. Sinusitis can be caused by viruses, fungi, allergies, and irritants, said Kenneth Einhorn, chief of the division of otolaryngology at Abington-Jefferson Health.
The inflammation can pave the way for bacteria. When mucus gets trapped in a sinus, it provides what Donald Solomon, an ENT at Cooper University Hospital, calls a “warm, happy environment” for bacteria that might normally be swept away.
Sinusitis can be acute, recurrent, or chronic. It’s considered acute if it lasts no more than a month or two. Some people have frequent, short-term sinus problems that they’re able to clear. These are recurrent. Still others end up with sinus problems that linger for many weeks or months. This is chronic sinusitis.
Know the signs
Typically, true sinus infections happen after you’ve had something else, like a cold or the flu, so you’re looking for symptoms that get worse after a couple of weeks. Sinus infection symptoms, Einhorn said, include thick mucus, pressure pain over an inflamed sinus, pressure in upper molars, ear fullness, postnasal drip, sore throat, and coughing that’s worse at night. Headaches, fatigue, and fever can also be present.
Chronic infection can be dangerous if it spreads outside the sinuses. If you notice a change in your sense of smell, you should get that checked out, Palmer said. That can sometimes be caused by a tumor.
Why are some people prone to sinusitis?
It’s probably some combination of genes, personal anatomy, and environment. You can have sinus problems when your sinuses are too wet – or too dry.
Solomon said some people with allergies have fewer sinus problems after they move to the desert. Cohen said people who live in the Deep South suffer more often from inflammation related to allergies and fungi. There are fewer cases of fungal infections as you go north and more caused by bacteria.
Air quality is also an issue. Pollution leads to more sinusitis, Palmer said. Smokers are at much higher risk, Einhorn said.
The septum, the wall that divides the two sides of the nose, can become bent or deviated enough to obstruct mucus flow. Polyps, which are small, fleshy growths, can also block openings.
Kie Frohnhofer, a 62-year-old contractor from Western Pennsylvania who was in Palmer’s OR the same day as D.J., has another medical condition associated with chronic sinus infections and polyp growth: aspirin-exacerbated respiratory disease (AERD). He had already had sinus surgery four times and gets frequent infections. “It feels like somebody set two bowling balls on my cheeks, and it’s just pushing into my head,” he said. Three of his senses — smell, taste, and hearing — have been affected.
Cohen has been studying a surprising connection between sinusitis and taste receptors in sinuses that affect our ability to fight off germs. So far, he’s established that one receptor involved in detecting bitter flavors also plays a role in combating Pseudomonas aeruginosa, a bacterium that causes about 15% of chronic rhinosinusitis. “We basically can explain a small part of the disease,” he said.
Cohen is running a clinical trial next year that will test whether spraying the bitter-tasting medication quinine in the nose makes people who’ve had sinus surgery better able to fight off sinus infections.
Age and sinusitis
Sinusitis becomes more common in middle age. According to the CDC, 15% of 45- to 74-year-olds got sinus infections in 2018, compared with 8.5% of younger adults. The percentage dipped slightly in those over 74.
A study earlier this year from Vanderbilt University Medical Center found that people over age 60 with chronic sinusitis had a different form of inflammation than younger patients and may be less responsive to steroids, which are often used to treat sinus problems.
Prevention for the susceptible
Sinus specialists are big fans of good sinus hygiene. Rinsing frequently with salt water — sprays don’t do the job — clears out the sinuses and helps keep tissue moist, doctors said. A neti pot can work, but doctors said the NeilMed squeeze bottle available in drugstores is well-designed.
Sinus sufferers need to take particular care to keep symptoms under control during their allergy season or when they catch a respiratory virus.
With a cold, Palmer, immediate past president of the American Rhinologic Society, said, “hit the saline hard.” Steam, including long showers, is also helpful. Use a humidifier in the winter.
Einhorn recommends starting an over-the-counter steroid spray like Flonase or Nasacort. Use a decongestant spray like Afrin for no more than three or four days.
When to see the doctor
If you’ve taken all the preventive measures above for 10 to 14 days and you still have symptoms, it’s probably time to see a doctor.
At that point, many doctors might prescribe a short course of antibiotics. Whether oral steroids should be used for “garden variety” sinusitis is controversial, Einhorn said.
Ibuprofen or acetaminophen can reduce sinus pain.
If the sinusitis becomes chronic, sinus specialists are likely to prescribe three to six weeks of antibiotics as well as oral steroids, perhaps added to nasal saline rinses for direct delivery.
Cohen said dupilumab, an injectable drug, was approved earlier this year for people with both polyps and chronic rhinosinusitis, and other biologics are in the works. “While there is a lot of excitement for it, it is expensive, about $30,000 per year,” he said.
When all else fails
Surgical remedies could involve fixing a deviated septum or removing polyps. Doctors may use balloon sinuplasty or minimally invasive surgery to improve drainage.
Doctors once thought that sinuses drained by gravity and they poked holes in the bottom of cavities to improve flow, Cohen said. They now know sinuses are more complicated. Tiny hairs called cilia actually work like an escalator to move mucus. Now, doctors focus more on widening sinus pathways to make irrigation more effective and deliver medications directly, which helps the cilia work better.
Many people’s sinuses are like houses built in the 1960s with lots of little rooms, Palmer said. In modern sinus surgery, doctors remove some of the partitions and inflamed tissue. “I make them into an open floor plan,” Palmer said.
People who have had sinus surgery need topical steroids, which have fewer side effects than oral steroids, for life.
Two weeks after their surgery, Debebe and Frohnhofer said they were breathing better than they had before their procedures.
Doctors said success rates are good, but, as Einhorn pointed out, “There’s nothing that is on the verge of a cure.”
Solomon said people still have to deal with their underlying allergies and the effect that has on sinuses. “Most people will tell you that they feel better,” he said, “that things have improved, but I also think it’s rare for people to tell you they’re 100% perfect.”
