Medical workers should get coronavirus vaccine first, scientific group says. Healthy, middle-aged people are at the back of the line.
Making sure that the racial groups hit hardest by the virus have early access to the vaccine was a priority.
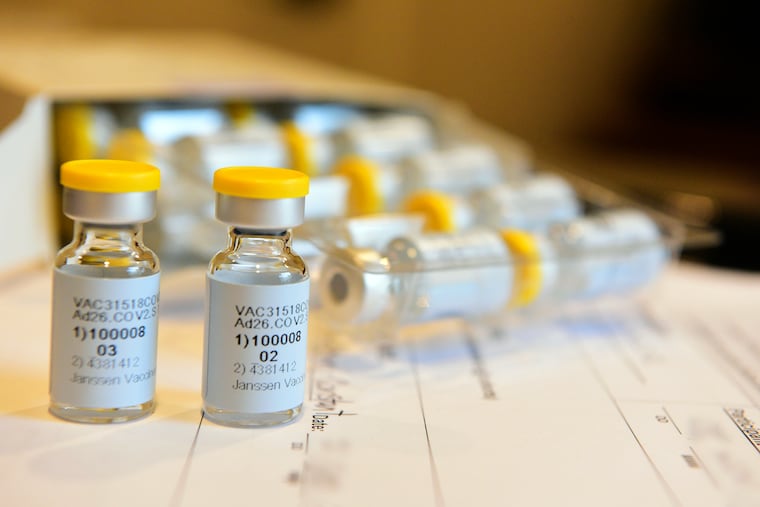
When there finally is an approved vaccine for COVID-19, the first doses should go to front-line health workers in hospitals, nursing homes, or home care as well as first responders like police officers and firefighters, according to new recommendations from the National Academies of Sciences, Engineering, and Medicine.
That first-in-line group, which represents 5% of the U.S. population, is critically important for keeping the health system running, but also faces high risk of getting and transmitting the new virus.
Once more doses are available, people with underlying health problems that put them at “significantly higher risk” for severe disease and death could line up for shots as part of Phase 1b. That would likely include people with two or more major health problems, such as cancer, chronic kidney disease, chronic obstructive pulmonary disease, obesity, heart disease or diabetes. Phase 1b, which includes about 10% of Americans, would also include people 65 and older who live in congregate settings, such as nursing homes, homeless shelters and jails.
A panel assembled by the national academies took on the project at the request of the National Institutes of Health (NIH) and the U.S. Centers for Disease Control and Prevention (CDC). It is difficult to know how influential its recommendations will be. Traditionally, the CDC’s Advisory Committee on Immunization Practices (ACIP) recommends who should get vaccines. It has been discussing allocation for months, but has not yet made official recommendations.
The academies panel said its recommendations may need to be modified depending on the characteristics of vaccines that prove safe and effective enough for widespread use. Some may be more effective in certain patient groups. Trials of vaccines currently in the final phase of testing have not included children.
The 237-page document stresses that it is important that Americans trust that the vaccine is safe. The group called on the government to reach out to minorities and other groups that are often skeptical about vaccines and may be even more concerned now because of political pressure to approve a vaccine quickly. It also said that public health officials involved in distributing the vaccine need to make it accessible to people who live in poorer neighborhoods and to racial and ethnic groups, such as Blacks, Hispanics and American Indians, that have been disproportionately affected by the virus.
Wide vaccine coverage is considered a crucial step in bringing the pandemic to an end. There are now 149 vaccines in development with four in the last stage of clinical trials. During a webinar to introduce the report Friday morning, Victor Dzau, president of the Academy of Medicine, said vaccine may be available by the end of 2020 or the beginning of next year, but there won’t be enough doses at first to meet demand.
Members of the panel emphasized the importance of having an independent, nongovernmental group weigh in on vaccine distribution. “This turns out to be so important for the trust factor,” said William Foegge, committee cochair, emeritus professor of international health at Emory University and former CDC director.
The group decided not to directly target race, Foegge said, but focus instead on racism, or factors that contribute to high disease burden among certain minorities. “This virus has no concept of color, but it has a very good concept of vulnerabilities,” he said. That led the group to consider health conditions that disproportionately affect minorities as well as social factors, like crowded homes, multi-generation households, and risky jobs that contribute to viral spread.
Helene Gayle, cochair and president of the Chicago Community Trust, said the group also believes the United States should share some of its vaccine with the rest of the world, support the World Health Organization, and participate in global vaccine planning.
The plan calls for vaccinating people in four phases. After Phase 1a and 1b:
Phase 2 — 30% to 35% of the population — includes teachers, child care workers and school staff as well as critical workers who can’t avoid coronavirus exposure. Think food and transit workers. It also includes people with health problems that put them at moderately high risk for severe COVID-19, defined as having one important underlying health problem. This group also includes younger people who live in congregate settings and the remaining people who are 65 and up.
Phase 3 — 40% to 45% of the population — includes children (if they were part of clinical trials) and young adults between 18 and 30, because their wide social networks make them likely to spread the disease. People who work in moderately risky businesses, like hotels, banks, gyms, hair salons and factories, are in this phase.
Phase 4 is everybody else. That seems to be healthy, middle-aged people in low-risk jobs. Plus everyone who could have been vaccinated earlier but decided not to.
The Academies panel said that ACIP should make specific age recommendations. If more than one vaccine is available at the same time, it will guide how they should be used.
The proposal allows for state and local flexibility.
