I worked at a hospital during the AIDS crisis. Medical workers have it worse now. | Opinion
I felt helpless and overwhelmed during the AIDS crisis — yet still far more supported than the health-care workers fighting the coronavirus today.
In 1987, I was an intern in a Bronx hospital when death caved in on me. Young patients collapsed in acute respiratory distress. The diagnosis: AIDS. The treatment: aerosol pentamidine. The outcome: quick death.
How did I feel as a physician working through a health crisis? Helpless, impotent, and overwhelmed. Courses in microbiology had failed to prepare me for this onslaught. And, yes, I also heard whispers of a “gay disease” at the nurses’ stations — fueled by government officials and others nationwide who were scapegoating this community.
Yet, there were things I never felt during that unforgettable year. I never felt unsupported by the hospital administration, nor lacking in equipment such as gloves, needle caps, or masks. I never for one instant doubted that I belonged right there with those patients, whether at their bedside on admission, whether holding their hand when they were being intubated, or whether hugging them when I told them they were going to die. I had taken the Hippocratic oath, and undergirding me was the medical community and a national government that supported my development as a physician.
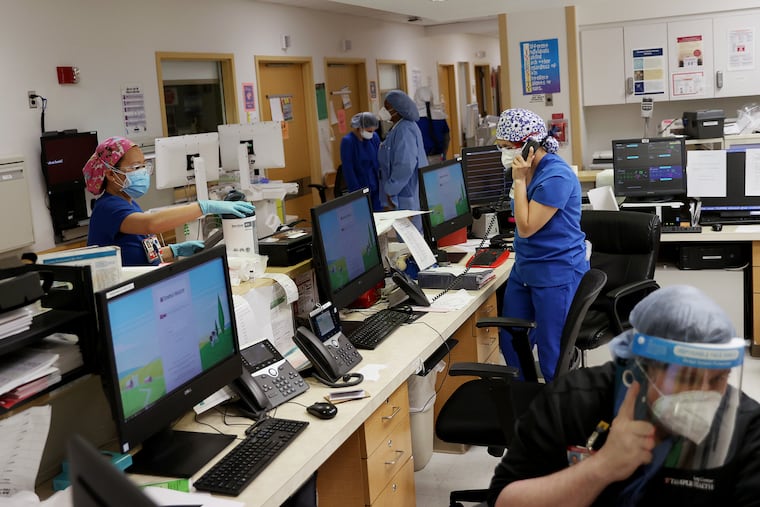
Fast-forward to 2020. While Americans offer symbolic support for at-risk workers, posting #HealthCareHero on social media and applauding them at nights, the reality is that frontline caretakers — including doctors, nurses, and other health professionals — are in an impossible position. While being asked to care for patients with respiratory symptoms, just as we were during the AIDS crisis, they lack structural support. Sometimes they lack basic equipment, access to crucial testing tools, and even the training necessary to deal with COVID-19.
Recently, I began to hear interviews with distraught ER nurses and to read op-eds written by frightened clinicians. My internist friend was told to keep quiet when he verbalized his fears at a meeting with hospital administrators. Another was fired when he granted an interview to a local newspaper to discuss safety. Another was told to go home when she purchased her own protective equipment after finding the one N95 mask given to her by her department inadequate.
» READ MORE: Healthcare workers don’t need Blue Angels. They need green money. | Solomon Jones
So what do I feel now? Furious. If I were in a frontline post, rather than a psychiatrist, I would respond reflexively to the sick person in front of me. But in my spare moments, before my head hit the pillow, I would feel conflicted about my obligations. What if I contracted the illness because I couldn’t protect myself? What about my obligation to my family, friends, students, and patients for whom I am responsible? The frontline health-care worker doesn’t have the luxury of ethical rumination. But the rest of us — non-frontline workers, leaders of clinical personnel, and the public — must claim it, including on their behalf.
Even when I accidentally stuck myself with a dirty needle from an infected patient in 1987 — and had to wait six months for a negative HIV test — I never felt as abandoned as our clinicians are now.
The woeful protection we are seeing for our health-care workers exposes several problematic dynamics in U.S. hospital systems. For one, hospital administrators have been co-opted by the business class. They have been given responsibility for the hospital’s bottom line, and are paid according to their performance in this domain. They are also responsible for planning, ordering, and stockpiling equipment for hypotheticals such as pandemics, but lack clinical background.
Moreover, clinicians rarely have the power to decide how hospital resources are spent, despite having the most intimate knowledge of patients and what is needed to take care of them. Within hospitals, administrators and clinicians rarely work in collaboration. Wouldn’t the system work better — and more ethically — if administrators sometimes worked rounds in the ICU and came face-to-face with unconscious patients, while clinicians were trained to balance their one-on-one obligation to the patient with their public health commitment to the communities they serve?
The public has not fully absorbed what will happen should our health-care workers become ill at high rates during this pandemic, which is likely given their exposure. If clinicians are home sick, who will take care of our citizens? I worry that effusive public support for health-care workers inadvertently relieves officials of their responsibility for the damage caused by lack of preparation for the pandemic. Praise for the workers, on its own, will not ultimately protect any of us.
Our political climate of division, in which President Donald Trump sees fit to undercut the experience and expertise of medical professionals, prevents our citizens from understanding their vulnerability. When health-care workers have reported that they lack essential protective equipment, the president has called their testimony “fake news.” Because physicians haven’t been trained to organize, they struggle to present their desperation cohesively.
Where is our collective anger? It is entwined with our helplessness and silence. Anger is a vital engine for mobilization. It can be scary, and easily gets turned inward or directed at the wrong target. Now is the time to aim it squarely where it belongs: at the health-care administrators and public officials failing our frontline workers. The health-care worker should never end up in this spot. Even when I accidentally stuck myself with a dirty needle from an infected patient in 1987 — and had to wait six months for a negative HIV test — I never felt as abandoned as our clinicians are now, and I never wanted to be anywhere else.
Andrew I. Smolar is a psychiatrist and psychoanalyst, a clinical associate professor of psychiatry at Temple University School of Medicine, and a training and supervising analyst at the Psychoanalytic Center of Philadelphia. ahzsmolar@verizon.net