Monkeypox is a public health emergency. Our messaging matters. | Expert Opinion
In the early days of an outbreak, it’s hard to know what to communicate to the public. But we need to do better.
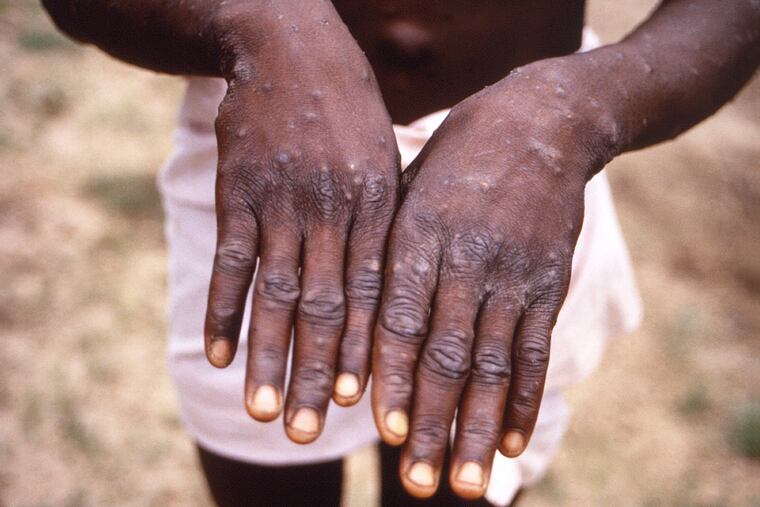
In June 2003, I was the chief government epidemiologist in New Jersey when the state received a report about a patient who looked like he had monkeypox.
It was an 11-year-old boy, who had just moved to New Jersey from Indiana. At the time, there was a small outbreak in the Midwest, traced to contact with pet prairie dogs that had been housed near infected animals imported from Ghana. The child had been bitten by an infected prairie dog, and now had a high fever and painful lesions on his body. His family seemed OK so far, but I knew that could quickly change.
Monkeypox outbreaks are rare outside of Africa; this was the first outbreak in the U.S. Following a protocol for investigating an infectious disease outbreak, and with guidance from the Centers for Disease Control and Prevention, we obtained tissue samples from the boy and sent them to the CDC for analysis. But it was going to take it days to confirm whether he had monkeypox. Now the question became: What should we do for his family?
The vaccine we mainly use today wasn’t approved for use in the U.S. until 2019; all we had was a live, modified virus version of the smallpox vaccine that can help prevent monkeypox, which is in the same family as the smallpox virus. We had some experience with the smallpox vaccine. Earlier in 2003, we had vaccinated several hundred health-care workers and first responders with this vaccine (including myself) in a campaign to prepare for a potential biological terrorist attack following 9/11.
Although none of the vaccines in this program had significant adverse effects, I hesitated over injecting seemingly healthy people with a live smallpox vaccine.
A more senior health official had reservations about vaccinating the boy’s family, voicing concerns about side effects. But I disagreed. Monkeypox is not often fatal, but it can be highly contagious, and I didn’t want an outbreak limited to the Midwest to spread here. So I acknowledged his concerns, but then offered the smallpox vaccine to the boy’s family members and several health-care workers with potential contact with the boy. The story ends well: No one had any side effects from the vaccine, and the boy ended up not having monkeypox, after all.
A new chapter
I tell this story now, nearly 20 years later, to show that in the early days of an outbreak, there can be some confusion. Depending on the cause of the outbreak (and its novelty), it can be hard to know how best to respond, who is at most risk, the source of the infection, what tests to do, who to treat and vaccinate (if there are available treatments and vaccines), and what messaging to share with the public. This was certainly true in the early days of COVID-19, and it’s true again in the current outbreak of monkeypox, which was just declared a global health emergency by the World Health Organization.
But this is not 2003. That outbreak spread to 47 people in the U.S., with likely many more unconfirmed suspected cases. In the current outbreak, more than 2,800 cases have been diagnosed in the U.S. as of Friday, from all but a handful of states. These cases are spreading from person to person for the most part, through close physical contact, not infected animals. Most of the patients have been men who have sex with men, but they are certainly not the only ones. On Friday, the U.S. reported the first cases among children.
“More than 2,800 cases have been diagnosed in the U.S. as of Friday.”
The good news is we now have a safer, two-dose vaccine available to prevent monkeypox. The bad news is we don’t have enough of it for all those people who may have had recent exposure, or are fearful of future exposure.
Pennsylvania has received only a few thousand doses so far. Philadelphia, too, is trying to meet the demand by starting with providing a single dose before additional doses arrive to complete the series.
For now, as with any new outbreak, the messaging matters. It’s up to public health officials to give people the information and tools they need to protect themselves from monkeypox until they can get vaccinated, and seek help if they need treatment. And from what I can see, we can do better.
» READ MORE: Pa. got more than 3,000 doses of monkeypox vaccine this week, but access is still limited
In New York City, public health officials are squabbling over whether to advise men who have sex with men to reduce their number of sexual partners. A brief scan of the websites of the health departments in our area shows a wide range of information on the current outbreak; New Jersey and Philadelphia offer the most comprehensive and updated information.
What to know
In case any of the messages you have heard are confusing, here are the main points: You are very unlikely to get monkeypox by casual exposure such as sitting next to an infected person on public transportation or at a mass gathering. The virus is not thought to be transmitted through airborne exposure, but by close, intimate contact with someone who is infected. Your best bet is avoiding skin-to-skin contact with someone who has the characteristic rash of monkeypox or who has been possibly exposed.
When it comes to advising people on their sexual behavior, here’s where I stand: We need to convey the message that certain behaviors are risky and that people can reduce their risk by modifying personal close encounters, even if it is only for the short term. This is not an anti-sex message.
Our public health departments need to communicate information to people that is grounded in science and current epidemiology. And they need to keep their websites updated with current information about the outbreak and the appropriate preventive measure locally. Just linking to the CDC website is insufficient to guide a local response. This is key to containing this outbreak, locally and in the U.S. The messaging should be consistent and nondiscriminating to minimize confusion and ensure timely access to testing, prevention, and treatment.
If officials keep having disagreements over who is at risk, and how best to prevent disease in the face of limited vaccine supply, they are only going to confuse and scare people. And that won’t stop the outbreak — if anything, it might make it worse.
Eddy Bresnitz is a physician and former deputy commissioner of the New Jersey Department of Health, where he was also the medical adviser to the COVID-19 Response Team.