The patient’s fever was so high that paramedic Tim Mumford could feel the heat radiating off the man’s skin through two layers of latex gloves. He fought for air in short, rapid gulps, drawing so little that his face was tinged with blue.
Pressing a stethoscope to the 56-year-old man’s chest, Mumford knew his patient needed more than an oxygen mask to survive the six-mile trip to Bryn Mawr Hospital. He also knew that opening the man’s airways would spray the coronavirus all over the back of the ambulance. Essentially a sealed metal box.
“Get out of the truck,” Mumford told his partner, Joe Ellis, also a paramedic with Narberth Ambulance.
Mumford went to work on tavern owner Jim Griesser. He got him to the hospital alive, hopefully with enough time for doctors to place him on a ventilator. Mumford had a bad feeling about Griesser’s chances. He tried not to dwell on it. Sometimes fixating on your rear-view mirror makes it harder to focus on the next 911 call ahead, Mumford explained.
Mumford then called his wife, a nurse at Christiana Hospital in Delaware. “Take the kids to your parents’ house,” he told her.
Five days later, the paramedic woke up with a screaming headache and a sore throat, fearful of coronavirus but relieved to know he hadn’t exposed his 3-year-old son and 11-month-old daughter. Or his partner.
Mumford, 34, was one of nine members of Narberth Ambulance who had to self-quarantine after a coronavirus exposure or positive test.
“This makes me nauseous. I’m scared for them. I can see the stress in their face.”
Now, for the first time in his nearly 30 years as volunteer chief of Narberth Ambulance, Christopher Flanagan said he fears for his team’s safety. The 50 paid staffers and roughly 80 volunteers of Narberth Ambulance sleep, cook, and eat together. They bicker and tease and console one another. Like any tight-knit family.
“This makes me nauseous. I’m scared for them. I can see the stress in their face," said Flanagan, whose military buzz cut matches his no-nonsense demeanor. He also is police superintendent in Radnor Township.
“When they see a call come in and they know that they are going to put themselves at high risk again, maybe five, six times in a day, that makes me ill. I want to protect them. I want to do something about it, and it’s just not that easy.”
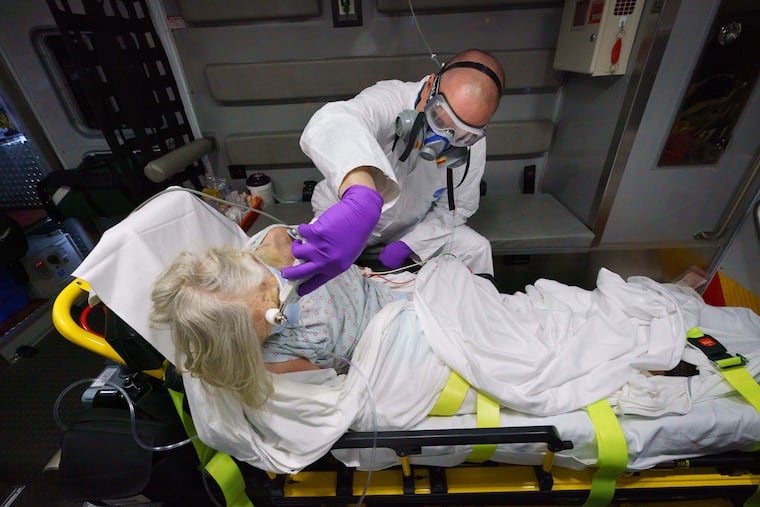

















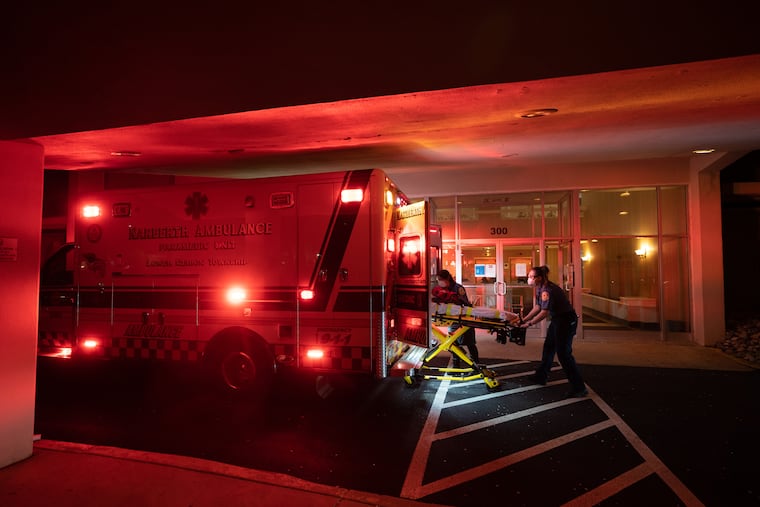

New rules
Narberth Ambulance responds to 911 calls across five towns that straddle Montgomery and Delaware Counties: Lower Merion, Narberth, Haverford, Conshohocken, and West Conshohocken.
On March 21, just days after Gov. Tom Wolf put Montgomery County on lockdown, Flanagan got on a video conference call with 78 company members. He laid out new protocols designed to limit staff exposure to the virus and reserve precious personal protection gear, like N95 masks, gowns, Tyvek suits, gloves. And banned hanging out at the station house when not on duty — a real departure for this team.
“Any questions?” Flanagan asked.
Paramedic Amanda Csanady, her voice wobbly, asked the question on everyone’s mind: “Are we going to die?”










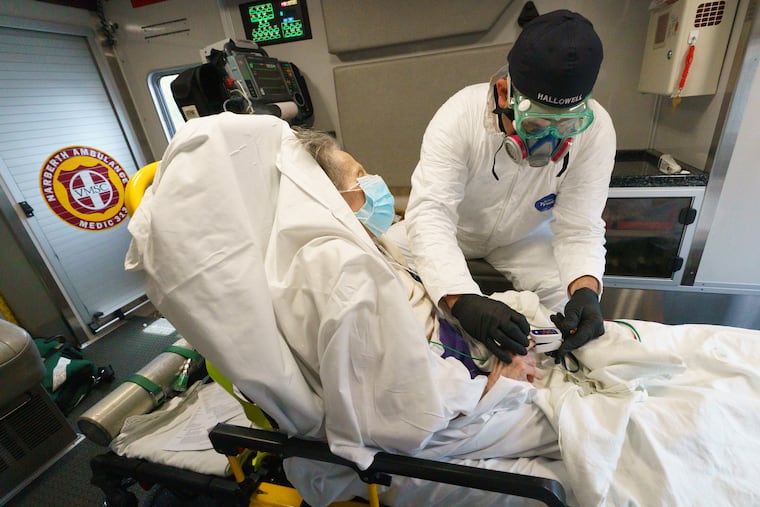
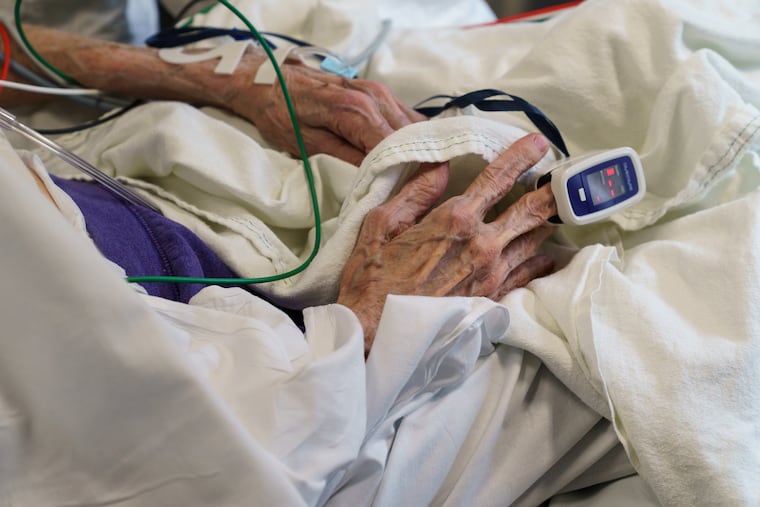








Csanady, 37, was alone in her Conshohocken apartment, her mind spinning: Is our system going to break down? What if the cops all get sick? Who is going to stop the looters?
Living alone has its pros and cons. “I don’t have to worry about coming home and infecting my family, but it’s also like, you are now in the apocalypse alone. You are just there with you and your thoughts — and the cat who hates me,” Csanady said.
She’s used to being in control of her health. “You can’t catch a heart attack," she said, while eating Greek yogurt mixed with chia and flax seeds for breakfast during a recent shift.
“Are we going to die?”
During the video conference, Flanagan saw she was near tears. He texted: “I will call you after call, Chris.” He made a mental note to have stress management reach out to her.
“We can’t take a chance with their mental health and their spirit," he said. "If you break that, then you don’t have anything left.”
An expensive fight
Before COVID-19, many of the company’s roughly 10,000 annual calls were car accidents caused by commuters heading in and out of Philadelphia. Or sports-related injuries from universities and schools in the area.
Calls are way down now, and so is the nonprofit’s primary source of revenue — billing insurance companies for hospital transports.
But fighting this virus is expensive. Each day, the company goes through gallons of a disinfectant called “quat,” short for quaternary ammonium cation. They hose down everything in the station at 6 a.m., 2 p.m., and 10 p.m.
At 2 p.m. on a recent Saturday, volunteer Sean Littlewood, an ICU nurse at Jefferson University Hospital, appeared in the doorway of the station’s common living area with a CO2 tank on a hand-truck dolly. The gas-filled cylinder powers a paint sprayer filled with quat. Fellow company members hopped off dorm-like wood couches with boxy blue cushions and scattered like insects. Littlewood fumigated every inch, from the worn pink carpeting to dining room tabletop. A haze filled the room.
“I don’t like breathing it,” said EMT Eric McKeever, as he Googled “quat” on his smartphone. “Did you read that quat causes severe skin burns and eye damage?”
“Makes sense,” Battalion Chief Drew Hallowell responded. “I’ve washed my hands with it and my hands are still attached.”
“For now,” quipped volunteer Danielle Levine, a resident physician at Jefferson University Hospital.
A cruel trick
The first call on a Saturday morning came from a Bala Cynwyd nursing home. A 94-year-old woman with COVID in respiratory distress. At 6:46 a.m., Lt. Patrick Glynn stood near the ambulance as Hallowell headed inside with a stretcher on wheels. To limit exposure and save on masks and Tyvek suits, only one paramedic goes inside. Nursing home staff bring patients to the lobby when possible, under the chief’s new rules.
This was at least their fourth trip here in two days. “We’ll see somebody in Room 201. Then we’ll go back a few hours later for the person in Room 202 and et cetera,” said Glynn, who wore a half-face respirator and a yellow disposable gown over his uniform.
“The person will be alive, but it’s a question of, ‘What kind of alive, you know?' ”
“The person will be alive, but it’s a question of, `What kind of alive, you know?'”
Of the coronavirus-positive 911 calls, roughly 90 percent have come from one of the area’s 14 nursing homes or rehabilitation centers, according to Narberth Ambulance statistics from March 15 to April 18.
By 7 a.m., Glynn and Hallowell arrived at Lankenau Medical Center. It was 44 degrees, the wind lashing a cold drizzle across the open canopy. Hallowell stood beside the woman outside the locked emergency room doors. With an orange-gloved finger, he rang the intercom. Staying outside is another new rule to protect paramedics.
“Hello?” Hallowell yelled into the call box. He pulled the blankets snug around the woman’s neck, though she insisted to him that she was just fine. But Hallowell knew she was in a state of “happy hypoxia,” a cruel trick of the coronavirus, in which her oxygen-saturation level was dangerously low. She was on the precipice of coding.
Hallowell, sweating inside his white Tyvek suit, hit the intercom again. A hospital security guard materialized on the other side of the glass doors.
“Can you tell them I’m out here with a COVID patient?” Hallowell said, his voice muffled through the N95 mask, but his frustration clear.
Within moments, a hospital staffer rushed out with a gurney.
“You’ll warm up now, Evelyn," Hallowell told his patient. “It was nice to meet you.”
Before leaving, Hallowell spread open his arms, as if about to be frisked, so Glynn could spray him from head-to-toe with disinfectant, careful to get the soles of his black boots. Hallowell stripped off his suit and tossed it in a hospital trash can. He thought about his own parents, who are almost 80.
“She was coughing when I walked in," Hallowell said. "They didn’t have a mask on her yet.”
Back at the station, he cranked up a playlist of Broadway show tunes to shake off the call. "We’ll close the town in a whirl. And we won’t come home until we’ve kissed a girl!,” the Hello Dolly lyrics go.
Hallowell, 50, started as a volunteer with Narberth Ambulance in 1987 and was in paramedic school in 1991, the year U.S. Sen. John Heinz’s Piper plane collided in midair with a helicopter, killing Heinz and six others, including two children struck by falling debris at Merion Elementary School.
He’s both hard-nosed and sentimental. Humming to West Side Story, he called out, “Anybody have laundry they want in?”
He walked by the common area, then doubled back when he saw Glynn and EMT Eric McKeever on opposite ends of a small couch, both wearing masks as prescribed. He frowned.
“Social distancing!” Hallowell said.
“I was here first,” McKeever replied, grinning.
Hallowell, a paramedic who is also an official team photographer for the Philadelphia Eagles, said he’s had “a temper tantrum or two” about people in his company not wearing masks. Even inside the Ardmore station, McKeever joked, you can hear him "bitching all the way in Haverford.”
McKeever served in the military during the Gulf War in 1990. He talked openly about killing soldiers with the Republican Guard in Iraq — and about needing therapy twice weekly because of it.
“I hate it,” McKeever said. “Nobody wants to look at themselves. I go just so that I’m not a horrible person to other people.”
‘In the name of the Father’
There was a collective groan inside the station when the name of a nursing home crackled over radio dispatch. They listened for the now-familiar code letters: “AFRI,” or “Acute Febrile Respiratory Illness,” the catchall phrase for a suspected COVID-19 case.
“In the name of the Father, and of the Son, and of the Holy Spirit. Amen,” a paramedic yelled out as the alarm sounded.
Red lights pulsing, Narberth Ambulance trucks passed one another to and from nursing homes. The service road leading to Lankenau felt like a conveyor belt as company members delivered patients with slim odds.
Paramedics said the nursing home population was vulnerable before the pandemic, but watching them die in quick succession has been hard. Each one — some World War II veterans and Holocaust survivors — carries a piece of history, lost.
Paramedic Chas Carlson, 26, said sometimes all he can do is hold his patient’s hand and try to be reassuring.
“This is where I would take my Mom if she was sick.”
“Listen, I know this is really scary but this is a great hospital. This is where I would take my Mom if she was sick,” Carlson said he tells frail, teary-eyed seniors.
But out the windows, what he sees tells another story.
“We pass those white refrigerated [morgue] trailers as we come in. I’m thinking to myself, `Am I taking them inside for the last time? Is this the end?’”
EMT volunteer Sarah Awad, 25, is perhaps Carlson’s polar opposite.
“Nothing bothers me,” she said. “In terms of the gore and the nature of EMS, I really don’t struggle much at all. I almost feel bad about it in terms of not being affected by things. I view other people’s pain and that’s really sad but none of the pain is my own."
Less than a week ago, Awad’s grandmother died of the coronavirus at an Ohio nursing home. On Sunday at about 1:20 a.m., Awad placed a resident from Rosemont Care & Rehabilitation Center in Bryn Mawr into an ambulance. The patient, a man in his 60s, was cocooned in wrinkled sheets; his head slack to one side, eyes barely open. Awad’s ponytail, curved into a “C" at the back of her neck, appeared childlike in contrast to the ghostly scene.
At Rosemont, residents are crammed three in a room, each passing the virus to the other.
“It’s no one’s fault,” Awad said. “It’s not just this one person. It’s not just this one setting. It’s every congregant setting in the world. Coronavirus just thrives in these settings.”
Paramedic Andrew Schifferli said he fears being asymptomatic and passing the virus to someone else. Even when not working, he obsessively takes his temperature, he said.
“If you cut corners," he said, “and someone gets sick and dies — that’s not entirely not on you. That’s partially your fault."
Still, the new 45-minute decontamination regimen after each 911 call is exhausting at times. During a recent Friday night shift, Schifferli tried unsuccessfully to save a nursing home resident. By the end, the 28-year-old paramedic said he felt like he had showered in the virus. Before the coronavirus, when a patient died, the paramedics rode home together in the front, talking through what went wrong. That night, he sat in back of the ambulance alone.
“It’s very isolating,” he said. “You’re sitting there, knowing that for whatever reason, you failed to revive someone, and you feel the virus lingering on you.”
The joy of ordinary runs
Nowadays, the paramedics almost welcome a non-COVID call. They especially appreciate talking to patients who are well enough to engage.
Last Tuesday afternoon, Tim Mumford and Chas Carlson were called to the Wynnewood apartment of 77-year-old James Bradley. He has a spinal cord injury and needed his catheter changed. A paratrooper in Vietnam, Bradley asked to be taken to the VA Medical Center in West Philadelphia. Ordinarily, Mumford and Carlson don’t have time to take patients to the city. But with most everyone staying home, traffic was light, so they agreed.
Mumford drove. Carlson and Bradley, a retired EMT and firefighter from Long Island, spent the 16-minute ride talking about books they’re reading. For Carlson, it’s The Lemon Tree, about a friendship between a young Palestinian man and an Israeli girl.
“I felt like I never really had a grasp on the conflict or really understood it,” Carlson said.
“I don’t feel like I’ve ever had either,” Bradley agreed. “I’m interested in it.”
Bradley reflected on the future, post-pandemic.
“We’re never going back to the way things were before,” Bradley said. “I’m not sure what our life is going to look like, what our society is going to look like, but it’s not going to be like before.”
For paramedics and EMTs, face masks will likely become mandatory on every call — the same way latex gloves did during the AIDS epidemic in the ’80s.
A surprise on TV
Narberth Ambulance members share so many tender moments with strangers each day. Sometimes their lives get forever intertwined.
Mumford, who got sick five days after treating Jim Griesser, tested negative for the coronavirus, but thinks he’s probably among the many who had a false-negative test. He remembered how scared he felt — not for him, but for Griesser — when he picked him up on March 27. He feared he had died.
But when Mumford was watching a patient’s homecoming parade on the news April 19, he recognized Griesser’s face. It felt like a gift.
Griesser, co-owner of Manoa Tavern in Havertown, spent 19 days in the hospital and 14 days on a ventilator. This Sunday, he and Mumford talked on the phone for the first time. Griesser’s voice was still hoarse.
“You sent me through a bit of a scare,” Mumford said.
“Sorry about that,” Griesser said.
“No, no. No need to apologize. I’m just happy to hear that you’re OK,” Mumford said.
Griesser said he was thankful to Mumford, fellow paramedic Joe Ellis, and all the nurses and doctors who cared for him.
One day, Mumford said, he hoped to shake Griesser’s hand.
“I’m a hugger,” Griesser said, “so I don’t know if it’s a year from now, or two years from now, but whenever we’re allowed to touch one another again, you’re gonna get more than a handshake, buddy.”

