Pa. nursing homes with COVID-19 cases should test all residents and staff, health officials say
More than two-thirds of the coronavirus-related deaths statewide have been residents of long-term care facilities.
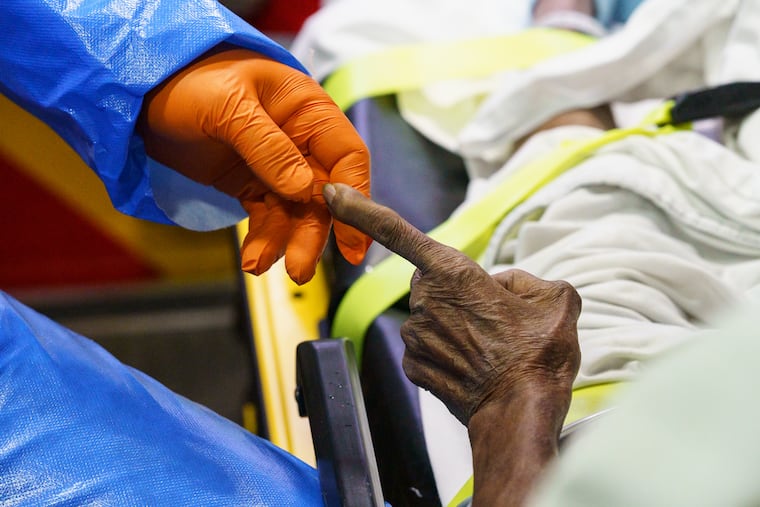
Pennsylvania health officials on Tuesday released new guidance to nursing homes, suggesting those with confirmed cases of the coronavirus test all residents and staff.
Secretary of Health Rachel Levine referred to the strategy as “universal testing,” and Gov. Tom Wolf called the plan “fairly radical," but an advisory state officials said was sent to long-term-care facilities across the commonwealth simply noted that testing of all residents “should be considered” in facilities with confirmed cases of COVID-19.
The advisory says that if a facility doesn’t have the capacity to do so, patients displaying symptoms should be tested, which long-term-care facilities have been doing for months. The advisory also recommended facilities without a confirmed case of COVID-19 test 20% of residents and staff.
However, the Pennsylvania Department of Health is “committed to testing all patients and staff in Pennsylvania’s long-term-care facilities,” Department of Health spokesperson Nate Wardle said in a statement.
He said via email that “the option is there for universal testing for facilities that need to do it,” but added that it isn’t recommended for facilities without confirmed cases.
The chief executive of a company that owns four nursing homes in Southeastern Pennsylvania said the alert didn’t go much beyond what nursing homes have been trying to do, given the limited availability of testing. “It’s a heads-up” for nursing homes to get ready for "the mandate that you must test everyone,” said Lisa Sofia, CEO of Premier Healthcare Management LLC.
Levine said Tuesday that the state’s testing capacity had increased in the last 2½ weeks as supplies of testing swabs have become more plentiful. She said tests would be processed by both commercial laboratories and a state-funded lab in Exton, and that the Pennsylvania National Guard will provide “mobile testing” to facilities that can’t test on their own.
"This effort will give us a clearer picture of the extent of outbreaks in nursing homes and a head start at stopping them,” Levine said. She did not answer questions about the cost of the mass testing program.
Pennsylvania has 695 nursing homes, with 75,000 residents, and at least 1,200 personal care homes.
Wolf said during a Tuesday call with reporters that the testing of employees and residents would be performed “once a week,” but the advisory sent to facilities didn’t require weekly repeat testing. It says initial testing should be prioritized and “repeat testing should be aligned with consideration for testing capacity.”
It also recommends that facilities retest residents who display symptoms consistent with COVID-19 but initially tested negative.
Of the more than 3,800 Pennsylvanians who have died of the coronavirus, more than two-thirds were residents of nursing or personal-care homes, according to Pennsylvania Department of Health data. More than 12,000 residents and 1,700 employees of upward of 500 long-term-care facilities have tested positive to date.
Pennsylvania Attorney General Josh Shapiro on Tuesday announced his office has opened criminal investigations into “several” nursing home facilities in the state, and called on Pennsylvanians to report suspected cases of neglect in such communities.
A handful of other states have required mass testing in nursing homes, including Maryland, which did so in late April. On Tuesday, New Jersey Gov. Phil Murphy said health officials will require all staff and residents at the state’s long-term-care facilities to be tested by May 26, with a follow-up test a week later. The state’s health commissioner said last week that under a pilot program in South Jersey, nearly 4,000 residents and staff were tested. Nearly 10% of staff and 24% of residents tested positive. Most were asymptomatic, she said.
Gov. Andrew Cuomo of New York said Sunday the state would require nursing homes test all staffers twice weekly.
Levine also announced other new requirements, including that hospitalized nursing home patients be tested for COVID-19 before being discharged back to their nursing home. In addition, long-term-care facilities will now be required to report cases and deaths to state officials using the same system hospitals do, with the goal of publicizing case and death counts by nursing home later this month.
The administration’s announcement came after weeks of bleak news from long-term-care facilities in the southeastern part of the state.
» READ MORE: Over 9 days, Bucks County saw 100 coronavirus deaths — most in nursing homes
County officials have repeatedly stressed that a large percentage of the COVID-19 deaths in their jurisdictions are seniors in these facilities. In the four counties surrounding Philadelphia, deaths associated with long-term-care facilities make up more than 80% of each county’s total deaths from the virus, according to data from the Department of Health.
Officials in both Bucks and Delaware Counties have asked the state to exclude long-term-care facilities from the county’s overall case counts that are used as one benchmark for when a county can begin to reopen some businesses. State officials have not committed to do so, but have said there will be some subjectivity in deciding when counties and regions can reopen.
Bucks County’s Neshaminy Manor, the only facility owned by the county, has been hit particularly hard, with 35 residents dying from the coronavirus as of Monday, county officials said. David Damsker, the head of the county’s health department, pledged last week to begin testing every resident at the facility as the infection rates soared.
In some of the region’s homes with high death figures, the lack of staffing has compounded an unprecedented situation. Some — like the Southeast Veterans’ Center in Chester County and the Broomall Rehabilitation & Nursing Center in Delaware County — have had the state dispatch National Guard members to their facilities to aid their struggling employees. Levine said Tuesday the National Guard has assisted 10 facilities.
The state-run Southeast Veterans’ Center has seen nearly 30 deaths from the coronavirus since early April as residents’ families routinely complain of a lack of information from inside. Some have told The Inquirer that critical questions about their loved ones’ care go unanswered for days.
Broomall has recorded similar numbers: 37 residents have died there from the virus amid similar complaints from outside about a lack of transparency.
Staff writers Harold Brubaker and Pranshu Verma contributed to this article.

