What are the symptoms of breakthrough COVID-19? And did I have it?
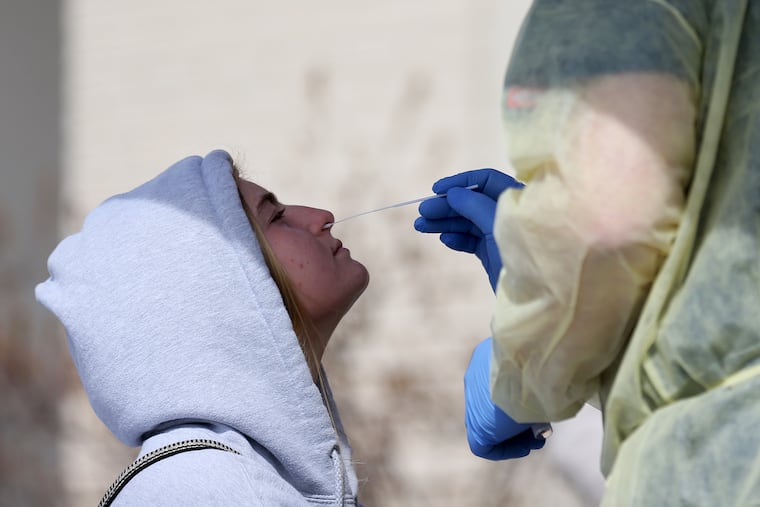
It's easy to mistake breakthrough COVID-19 symptoms for allergies and sinus problems. Testing remain confusing.
I returned home to suburban Philadelphia from a trip to the Chicago area on a recent Sunday. That Monday, I began learning firsthand how confusing COVID-19 remains 19 months into the pandemic.
I had driven across Western Pennsylvania, Ohio and Indiana — all places with higher COVID-19 case rates than we have here — on Labor Day weekend to help a childhood friend downsize. We were both fully vaccinated, albeit six months ago. At rest stops, I wore a KN95 mask, but the vast majority of fellow travelers were maskless. Some employees also eschewed masks, including a pale, weary-looking fast-food worker who did not cover a sneeze and responded to my glare with a sullen, “Sorry.” Masks were also a rarity at the two hotels where I stayed.
I spent the week cleaning, loading boxes and carrying heavy stuff up and down stairs. There was much dust. We ate outside at three restaurants. My friend contributed belongings to a neighborhood garage sale. I regret not wearing a mask for that, but it was also outside. I drove the 780 miles home flanked by fields of blooming weeds.
So, that Monday, when I felt achy, congested and tired, I was not concerned. I’m prone to sinus problems after late-summer visits to my Midwestern homeland. Muscle aches were to be expected. But I also had a sore throat and a slight cough, unusual symptoms for me and possible signs of COVID-19.
» READ MORE: What to expect if you get a breakthrough infection
I still had the symptoms on Tuesday, along with some chest tightness and slight ear pain. No fever. My pulse oximeter reading was normal. I had a dentist appointment on Thursday, though, and I imagined the screening questions. Have you traveled into a COVID zone? Do you have symptoms? I would be sent home. I figured a quick test would solve that problem.
Ha! Appointments at my local testing centers were full, making results by Thursday morning impossible. What about a 15-minute, over-the-counter antigen test? Those were not available nearby, either, but I found one by Ellume at a CVS eight miles away. It was well-designed and easy-to-use. Soon I had shocking results: I was positive.
Whoa, I thought. This surely means that thousands of people are walking around spreading virus while thinking they have allergies. I canceled the dentist appointment, resigned myself to 10 days of CDC-recommended isolation and obsessed, fruitlessly, about how the virus got to me.
» READ MORE: Don’t confuse allergy symptoms with COVID-19.
Then I wondered whether I should get monoclonal antibodies, a treatment that amplifies immune response to the virus. I’m old enough to qualify (65-plus), although my very minor symptoms argued against it. Before deciding, I wanted confirmation, and I knew that PCR tests are considered the best.
A telehealth doctor — my regular doctor and the local urgent care center refused to see me because of my at-home results — ordered a PCR test at a nearby hospital. I got Tuesday’s last appointment. An employee gave my throat — not my nose — a perfunctory swipe and hurried away. A day later, I got those results: Negative.
First thought: Yay, I don’t have COVID.
Second thought: But it was a throat swab.
I knew that the vaccine might allow the virus to enter and infect my nose, but it is meant to prevent more serious infection in the lower respiratory tract. What if the virus were only in my nose? To be extra safe, I scheduled a third, nasal PCR test — the earliest appointment I could get was Friday — at a drugstore, also not near my house. I awoke Saturday feeling much better. By Sunday, when the new results — also negative — arrived, most of my symptoms were gone.
The experience left me frustrated with the state of testing, a consistently weak point in the U.S. defense against COVID-19. President Joe Biden has pledged to make tests more available and affordable. I was also left with questions not easily answered by Google searches, including whether I actually had COVID-19 or not. So I asked some experts what they know about breakthrough cases and testing in the hope that it would help others struggling with the same questions.
What are the symptoms of breakthrough COVID-19 cases?
This can run the gamut from no symptoms at all to illness that sounds like what we’ve been hearing about for months in the unvaccinated. You will find stories on the web of people warning you that having “mild” breakthrough symptoms means not-bad-enough-for-the-hospital to doctors, but still feels really crappy.
The more common experience, doctors told me, is that many vaccinated patients have symptoms like mine, truly so mild that they could easily be written off as allergies, sinus problems or colds.
Breakthrough symptoms have not yet been well-studied, doctors said. A rare effort came from the Zoe COVID study, which relies on information users submit on an app. In June, it found that the top five symptoms for breakthrough COVID were headache, runny nose, sneezing, sore throat and loss of smell. In unvaccinated cases, the top five included headache, sore throat, runny nose, fever and persistent cough.
“It’s been a tricky virus,” said Elyse Morel, lead physician for Virtua Urgent Care. “It’s good at mimicking other things.” Many cases that looked like sinus infections to her turned out to be COVID-19.
Judith O’Donnell, an infectious diseases doctor and director of infection control at Penn Presbyterian Medical Center, said doctors are seeing runny nose, stuffiness and congestion more often in vaccinated patients. Many have just one or two symptoms at a time, rather than the broad constellation of symptoms that unvaccinated patients often experience.
Doctors said sore throat, headache, brief fever and cough are also common breakthrough symptoms. Short-term loss of taste and smell can also happen.
O’Donnell said vaccinated people seem less likely than the unvaccinated to develop fever, gastrointestinal symptoms, low oxygen levels or pneumonia. She is not seeing the second, very serious phase of infection that often puts unvaccinated people in the hospital or intensive care unit.
When should you get tested?
If you have sniffles and you haven’t been around other people, you probably have allergies. But anyone who’s been out and about needs to keep in mind that the delta variant is markedly more contagious than previous strains of COVID-19.
Virtua’s Morel is finding infection in vaccinated people who thought they were following all the protective guidelines. “I’ve met some folks where we were surprised when their COVID test came back positive,” she said. “Even if it seems like something you’ve had in the past, please don’t hesitate to get tested.”
O’Donnell suggests testing when you have a new symptom that is unusual for you. William Schaffner, an infectious-diseases specialist at Vanderbilt University Medical Center, says the threshold for testing should be especially low for frail, older people who are at high risk for serious COVID-19.
He said “testing has kind of drifted off the radar screen” as the country emphasized vaccination. It is especially important now that businesses are requiring employees to get vaccinated or face extra tests. It remains to be seen, he said, whether the United States has adequate testing capacity.
Martin Topiel, a Virtua Health infectious-diseases specialist, conceded that getting a test quickly is already a problem. “Access to testing is a challenge for everybody,” he said. “Getting results fast is very important so that we prevent spread to others.”
This is the rub. Even if you’re not very sick, you can spread the virus to people who might get much sicker than you. On the positive side, vaccinated people tend to spread the virus to fewer people than the unvaccinated do, and they’re contagious for a shorter period of time, although no one knows what that is.
What kind of test should you get?
This is the tricky one. Experts gave conflicting information, just as my tests did.
The kind of antigen test I took is usually quite reliable, especially for people who have symptoms. That’s because these tests look for proteins made by the virus soon after it invades the body and is most contagious. These antigens surge in the first few days of infection, then plummet within a week.
Antigen tests are particularly good at determining when people are infectious, said E. John Wherry, director of the Institute of Immunology at Penn Medicine. Virtua Urgent Care retests people who get negative antigen results but accepts that positives are accurate. I chose not to get monoclonal antibodies, but could have done so based on my antigen test results alone.
» READ MORE: COVID-19 testing at home is both possible and reliable. Here's what you need to know.
But PCR tests are considered the gold standard. Because they can pick up a minuscule amount of viral genetic material, they are far more sensitive than antigen tests. Results take longer, though, and people can test positive when they are no longer infectious. While some doctors, including O’Donnell, think throat and nose swab versions are interchangeable, others said the more uncomfortable nasal test is better. They’d like more information on what is best for vaccinated people.
Ravina Kullar, a spokesperson for the Infectious Diseases Society of America and an infectious-diseases consultant to Los Angeles nursing homes, suggested that getting a throat swab may not have been ideal in my case. Wherry agreed that it would have been better for both my antigen and PCR test to use samples from my nose, because the vaccine could have prevented viral replication lower in my body.
The throat swab, Wherry said, is valuable for telling whether the virus has gotten into the lower respiratory tract, where it can do its most serious damage.
He thinks we all should have antigen tests on hand for situations such as mine. He admits that’s not easy. His wife has allergies, and he had trouble finding tests, too. “At-home, rapid tests should be much more available,” he said. He also thinks they should be free, which they are not. “Everybody should have a stack of these in their house, in my opinion.”
He thinks the antigen tests correlate best with whether a person is currently infectious, and that’s a crucial factor in isolation. If at-home tests were widely available, Wherry said, “this would take out of circulation most people who are infectious.”
So, did I have COVID-19 or not?
“We would probably consider you to be negative,” Topiel said.
Wherry’s view was that I probably was negative by Friday, but likely was positive when I took the initial antigen test. “I think that you probably had an infection,” he said. “It stayed in the nasal cavity. … I think what you’re describing is what we’re going to see a lot more of moving forward.”
Should I (and other vaccinated people) have insisted on a nasal PCR swab? Wherry said he probably would now. “It’s a great question, and I don’t have a great answer for you,” he said.
Should vaccinated people get monoclonal antibodies?
This treatment, which is given as an infusion, must come during the first 10 days of symptoms. Vaccinated people can get it if they are old enough or are considered at high risk.
» READ MORE: Monoclonal antibodies can help high-risk people with COVID-19
Wherry thinks most vaccinated people won’t need the extra boost. He would use it in people known to have particular deficits in their immune response, such as multiple sclerosis patients who take a medication that affects production of antibodies.
Most doctors I talked to, though, thought this treatment was a good idea for people with breakthrough cases.
Kullar said you can’t tell whether your case is going to stay mild, and the treatment is an “extra layer of protection,” especially for people who are immune-suppressed or have other medical problems.
O’Donnell said she wouldn’t base the decision simply on age, but she would give monoclonal antibodies to people who are moderately or severely immunocompromised. Topiel said Virtua offers it to everyone who is eligible.
Schaffner favors it for people 65 and over or in high-risk groups, whether they’re vaccinated or not. “My strong recommendation,” he said, “is run, do not walk. Get that monoclonal antibody treatment.”
Now what?
You’ve heard this before, but the doctors want you to hear it again. The vaccines do not give you an impermeable armor against this virus. O’Donnell likens it to using an umbrella in a downpour. It will deflect most of the rain, but you could still get wet. Distancing and mask wearing add to your protection. Even outside, masks are a good idea when you can’t distance from others.
If you think things are confusing now, just wait. Respiratory syncytial virus, or RSV, is already making an early, intense assault on the country, and it can look like COVID-19. Flu is waiting in the wings. Morel has already seen a couple cases. Flu symptoms strongly overlap with those for COVID-19.
“If you think there’s muddying of the waters now, wait till we get into the flu,” Schaffner said. “This winter, I think clinicians are going to do a lot more testing.”
Addendum: Five days after I thought my symptoms were gone, I awoke with a fever and headache. These can be symptoms of COVID-19, but also other viral infections. I had barely left the house since my first test. I was tested at an urgent care center for COVID-19, flu and RSV. All came back negative. I had the fever for four days.
On Oct. 1, Ellume, the maker of my over-the-counter COVID-19 test, voluntarily recalled several lots of its tests because of elevated rates of false positives. My test was from one of the recalled lots.
» READ MORE: Our best Philly tips: Read our most useful stories
Staff writer Marie McCullough contributed to this article.
