Don’t know any COVID-19 patients who’ve died or been in the hospital? That may explain a lot.
People are bad at evaluating risk when numbers are involved. A personal connection may tip the scales.
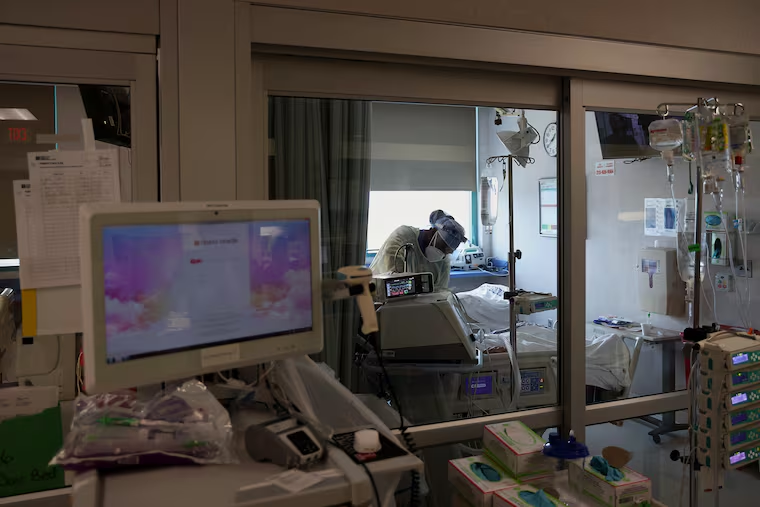
Seven months into the pandemic, it’s no secret that plenty of people still downplay the risks of COVID-19, scoffing at mask-wearing and social distancing.
Politics clearly feeds that mind-set, as suggested by a new Pew Research Center survey in which Republicans were more likely to say the crisis was overblown. Others may resist restrictions — capacity limits in restaurants, say — because their livelihoods are at stake. And psychologists have warned that COVID-19 fatigue can lead people to be careless about precautions.
But a more fundamental reason for the uneven support of COVID-19 prevention measures may lie in simple math: Despite more than 200,000 deaths and 400,000 hospitalizations in the United States, an Inquirer analysis suggests that in much of the country, the typical person knows no one in either of those categories. (Surveys, including another one by Pew, have reached similar conclusions.)
That explanation may seem jarring — do we really need to know someone who is gravely ill in order to practice safe behavior? — but psychologists say it makes sense. Human beings are notoriously poor at evaluating risk, particularly when the threat in question is more abstract, or when numbers are involved.
A personal connection to a problem makes it seem more real, said Carnegie Mellon University researcher Julie Downs, director of the Center for Risk Perception and Communication.
“If you know a bunch of people who have gotten sick, or if you have a family member who died or got sick with COVID — especially if it’s somebody you know well enough that you were with them and helping them — you’re naturally going to think that it is more likely to happen in general," she said.
» READ MORE: With young adults fueling COVID-19, a surge in vulnerable older people may be just weeks away, says CDC
Other research suggests that a failure to embrace COVID-19 restrictions may be fueled by a lack of empathy, in the same way that someone in rural Pennsylvania may not view urban gun violence as an urgent problem, or that those without military family members may give less thought to the ongoing toll of combat.
In one study, psychologists found that people who expressed higher levels of concern for people with COVID-19 were more likely to report that they had limited social interaction to reduce the spread of disease. What’s more, the researchers found they could influence a person’s level of concern.
In the same study, a different group of participants was directed to read a passage about how social distancing would relieve pressure on hospitals and prevent severe illness, especially among the elderly. Another group read the same passage and also watched a video about a 91-year-old man who was worried the virus would infect his chronically sick wife, while a third control group did neither.
Afterward, those who watched the video and read the passage were more likely to express support for COVID-19 restrictions than those who only read the passage, the authors reported in Psychological Science. And those who only read the passage were no more likely to support restrictions than those who had received no information at all.
The findings suggest that in seeking to encourage safe behavior, public health officials may need to supplement facts with an appeal to empathy, said lead author Stefan Pfattheicher, an associate professor of psychology and behavioral sciences at Aarhus University, in Denmark.
» READ MORE: How ‘caution fatigue’ may slow social distancing efforts
“The knowledge is there, but some people don’t adhere to this knowledge,” he said. “Maybe information is not enough.”
As for the math of not knowing someone with severe COVID-19, let’s take it step by step. To determine the chance that two events will occur, you multiply the probability of one by the other. Such as when you flip a coin once, the chance of getting heads is 50%. Flip it twice, and the chance of getting heads both times is 50% times 50% — 25%. Three flips, and the chance they all are heads is 25% cubed (12.5%), and so on.
Here’s how it works with COVID-19. So far in the United States, one in roughly 800 people has been hospitalized, meaning the chance that a given person has not been hospitalized is 799 out of 800 (99.9%) So the chance that any two people have not been hospitalized is 799/800 times 799/800 — 99.7%. For three people, it is 799/800 cubed (99.6%), and so on.
(This method isn’t strictly accurate, because picking a person at random from the entire U.S. population is not like flipping a coin, and the odds of COVID-19 hospitalization for each additional person added to the calculation will be ever-so-slightly different. Also, the true probability that a given person knows someone with severe COVID-19 will vary widely depending on geography and age, said Ashton Verdery, a demographer at Pennsylvania State University. But after hearing a description of the Inquirer calculation, he said it was reasonable as a rough approach.)
Then take the fact that the average American knows about 600 people, as researchers at Columbia and Princeton Universities have calculated. Take 799/800 raised to the 600th power (multiplied by itself 600 times), and the result is close to 50% — i.e., there is about a 50-50 chance that the “average” person does not know someone who was hospitalized with COVID-19.
Same goes for deaths. One in about 1,600 Americans has died of COVID-19, leaving 1,599 of 1,600 that have not. Take 1,599/1,600 raised to the 600th power, and you find the typical person has greater than a two-thirds chance of not knowing someone who died of the disease.
These estimates are roughly consistent with a Pew survey in August, in which four in 10 Americans said they knew someone who had been hospitalized or died as a result of having COVID-19. In a reminder that the disease has hit harder in communities of color, 57% of Black Americans said they knew someone who had been hospitalized or died.
The racial gap is especially acute in Philadelphia, according to a new Pew survey last week. One-third of Black and Hispanic residents said they knew someone who had died of COVID-19, compared with just one out of eight white Philadelphians.
Human beings have a good sense of relative risk, said Downs, the Carnegie Mellon researcher. We know it is safer to stand back from a cliff than stand on the edge. But when it comes to evaluating numbers, our perceptions are easily distorted.
And after seven months of a pandemic, those numbers will only get bigger.
