Who lives, who dies: Pa., N.J. facing tough priorities as COVID-19 cases mount
“Any time you’re trying to decide who gets a ventilator, who gets life-saving equipment, because of limited resources, they’re gut-wrenching, difficult decisions,” said a Philadelphia health-care leader.
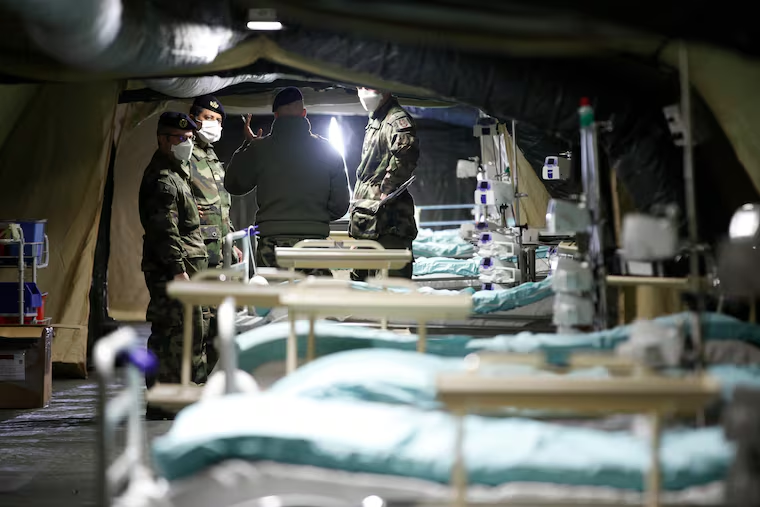
As New Jersey’s COVID-19 cases surged to almost 7,000 Thursday, behind only New York’s, health officials in the Garden State and in Pennsylvania prepared guidelines doctors may be forced to use in deciding which critically ill patients will get access to life-saving technology and which will not.
The prime issue is access to ventilators, essential to keeping what could be thousands of severely ill patients breathing long enough to recover from the virus. Both states have acknowledged that they will be thousands of ventilators shy of what will be needed if the coronavirus continues on its current trajectory.
"That is, I would have to say, one of the more difficult issues that we will be discussing,” Judith Persichilli, New Jersey’s health commissioner, said Thursday.
New Jersey’s cases grew by almost 2,500 overnight; Pennsylvania’s total was 1,794 Thursday.
“We have to obviously hope for the best but plan for the worst,” New Jersey Gov. Phil Murphy said in a news conference Thursday. "This is literally to keep the curve as flat as possible and below the capacity of the health-care system, including all of the equipment.”
New Jersey’s triage policy is being crafted, officials said. Pennsylvania has an interim policy being circulated to the health-care community, but it is not being made public, said Nate Wardle, a spokesperson for the state Department of Health.
Pennsylvania Health Secretary Rachel Levine declined to call the guidelines a triage policy, calling it instead a “crisis standard of care." She also noted that physicians and health systems will still exercise their judgment.
A Pennsylvania physician who has seen the state’s draft guidelines said they do not set out hard rules on ventilator access based on age or preexisting conditions.
“It’s a combination of how critically ill a patient is and determining how long and whether they would benefit from ventilator treatment and prognosis over the short, medium, or long term,” said Arvind Venkat, an emergency physician at Allegheny General Hospital in Pittsburgh and president of the Pennsylvania chapter of the American College of Emergency Physicians.
» READ MORE: This physician knows what a ventilator shortage means during COVID-19 — and how we all can help | Expert Opinion
His organization contributed to writing the guidelines, he said, and emphasized that no Pennsylvania hospitals have begun to face shortages that would require such guidelines.
“These are incredibly awful decisions, and I just don’t know that we want every doctor or nurse having to choose on their own, so we need to start creating some set of policies about how we will ration care,” said Ashish K. Jha, a doctor and director of the Harvard Global Health Institute. “I think we should put that word out there: We are going to ration care, so some people will live and some people will die.”
A state triage policy does provide some legal cover for doctors who may face malpractice lawsuits over patient deaths, said Robert Field, a professor of health management and policy at Drexel University. Their most significant value, though, is to allow a framework for decision-making.
» READ MORE: Coronavirus could mean even hospital-rich Philly won’t have enough intensive-care beds, experts warn
“To ask them to withhold care or withdraw care, even when it’s necessary, is asking them to do something they’re not trained to do and probably goes against their inclination,” he said. “They didn’t go into medicine to deny care.”
Bioethical decision-making
Doctors and nurses have been talking for weeks about news reports of Italy’s hospitals being overwhelmed with COVID-19 patients, said Jack Lynch, chief executive and president of Main Line Health, which runs four acute-care hospitals in the Philadelphia suburbs.
“Any time you’re trying to decide who gets a ventilator, who gets life-saving equipment, because of limited resources, they’re gut-wrenching, difficult decisions,” Lynch said.
» READ MORE: As COVID-19 crisis worsens, Pa. and N.J. have even fewer life-saving ventilators than anticipated
Health-care workers routinely discuss triage protocols while planning disaster response, he said.
“When you’re on the scene of a mass casualty, for example, they triage based on the likely outcome,” Lynch said. “And so people who are near death often are not given the same level of care as people who are likely going to be benefiting from that life-saving care.”
Persichilli said she hasn’t yet seen New Jersey’s plan for “bioethical decision-making," which was drafted by a subcommittee of doctors in the Medical Society of New Jersey. She said she’ll meet soon with the state’s COVID-19 advisory group to discuss “bioethical considerations of the availability of particularly life-saving modalities, like ventilators."
“But I do want to make sure that everyone understands that we are doing everything possible to make sure that we do not get into that situation, but if we do, we will be prepared,” she said.
A troubling trajectory
Most people who develop COVID-19 will recover without hospitalization. But current estimates are that during the peak of the epidemic — which has not yet been reached — more than 12,000 Pennsylvanians and 8,000 Garden Staters could require ICU treatment at any given time. Of those, about half will likely require treatment with a ventilator, and some will need to spend weeks on the devices.
» READ MORE: Worldwide coronavirus infections near 500,000 as health systems buckle
North Jersey is nearing a crisis point, and Persichilli ordered three major hospitals across the state to establish field hospitals in the coming weeks. New Jersey has about 1,900 ventilators statewide and has asked federal authorities for 2,500 more, Murphy said Thursday.
The Pennsylvania Department of Health is reporting it has 3,600 ventilators available — still far short of the need but more than it knew of a few days ago. Wardle said the state is working to get more from various sources including the federal Strategic National Stockpile.
» READ MORE: Pa. coronavirus shutdown wreaks havoc on economy as new unemployment claims top 645,000
Health experts say stringent social distancing and stay-at-home policies will be crucial to avoiding ventilator shortages.
Pennsylvania’s COVID-19 cases have been doubling every two or three days, Allegheny General’s Venkat said. Still, he found something to be hopeful about.
“The only silver lining is, it’s pushing into the public consciousness the need to accelerate ventilator manufacturing and supply chains,” Venkat said.
Staff writers Lisa Gartner and Pranshu Verma contributed to this article.

