Opioids after surgery far more common in U.S., Canada than in Sweden
Compared to their counterparts in Sweden, patients in the U.S. and Canada were seven times as likely to fill opioid prescriptions after four low-risk surgeries.
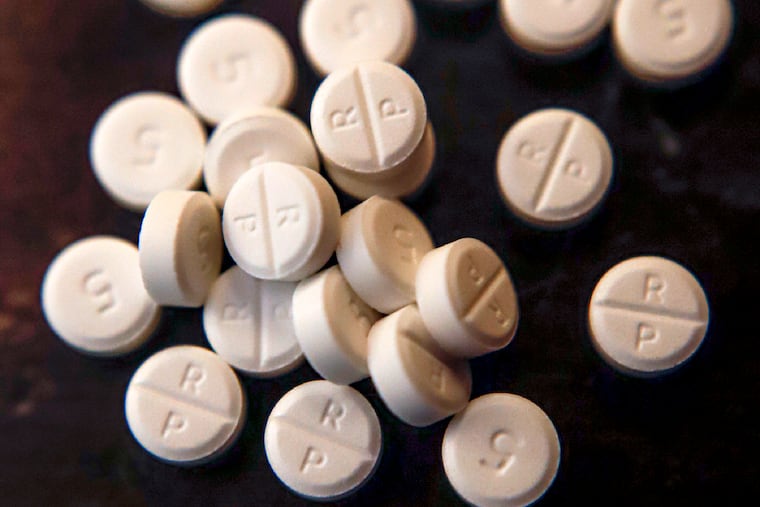
The opioid epidemic has been blamed in part on physicians who prescribed too many of the addictive drugs to patients recovering from surgery.
A new study suggests that in North America in recent years, the numbers were especially skewed after certain low-risk procedures for which safer pain medicines can be sufficient.
Compared with their counterparts in Sweden, patients in the United States and Canada were seven times as likely to fill opioid prescriptions after undergoing one of four procedures: laparoscopic gallbladder removal, laparoscopic appendectomy, knee arthroscopy to remove the meniscus, and lumpectomy.
The study authors, among them four from the University of Pennsylvania, did not determine why the prescription totals varied so widely. Nor did they advocate that doctors prescribe no opioids for the surgeries studied, as some patients may feel substantial pain.
Yet the findings serve as a reminder that for many common procedures, opioids need not be the default choice, said Mark D. Neuman, an associate professor of anesthesiology and critical care at Penn’s Perelman School of Medicine.
“It’s not to say that these aren’t potentially painful experiences,” Neuman said. “It’s just to say that the way we treat them in the United States is not the only way to operate.”
The researchers sought to compare opioid prescriptions in the U.S. and Canada — both of which have been ravaged by the epidemic — with those in a relatively unscathed western European country. The authors settled on Sweden because data were readily available for the four kinds of surgery in question, Neuman said.
The researchers compared the numbers of prescriptions filled within a week of surgery for more than 200,000 patients ages 16 to 64 in the three countries. None had been prescribed opioids previously.
More than two-thirds of U.S. and Canadian patients filled their opioid prescriptions after each of the four surgeries, with rates hitting 80% in both countries for arthroscopic surgery to remove the meniscus. In Sweden, the rates ranged from just 2% after a lumpectomy to 16% after laparoscopic surgery to remove the gallbladder or appendix, the authors reported in JAMA Network Open.
» READ MORE: Opioids, ankle sprains, meniscus tears, and more news from orthopedics research
The data included the years 2013 and 2014 in all three countries, and also 2015 for the U.S. and Canada.
The rates at which patients fill prescriptions may have declined somewhat since then, as public health experts have increasingly sounded alarm.
In guidelines issued in December 2018, for example, the Philadelphia Department of Public Health recommended that no opioids be prescribed after “minor” procedures. Laparoscopic gallbladder removal, arthroscopic knee surgery, and lumpectomy all were said to meet that definition. Appendectomies were not mentioned.
At Penn Medicine, where Neuman is chair of the opioid task force, the health system has not adopted such a policy. But it has taken a variety of steps to limit prescriptions, such as lowering the numbers of pills in the default settings of its electronic prescription systems.
Research has shown that many prescribed pills go unused, raising the risk of “diversion” — when pills fall into the hands of recreational users.
Though the study authors did not determine why prescriptions were filled less often in Sweden, Neuman said, marketing restrictions could play a role.
That country does not allow the marketing of prescription drugs to patients, unlike the U.S., where drug companies have been accused of minimizing the addictive nature of prescription opioids.
In Canada, prescription drugs can be advertised to patients on a limited basis, referencing only their “name, price, and quantity.” References to a drug’s “therapeutic use and/or benefits” are not allowed.
Neuman said the variation between Sweden’s opioid prescription rates and those in the two North American countries is so extreme that multiple factors are likely at play.
The authors did not have access to patient satisfaction scores, and as a result, they said it was possible that pain was undertreated in Sweden. But evidence suggests that opioid prescribing practices in Sweden are more “judicious,” the authors wrote.
“I think the starting point in the U.S., it seems to be the assumption that somebody will need opioids,” Neuman said. “I don’t think we can snap our fingers and say, ‘Let’s decide to be Sweden today.’ It really reflects probably a very different cultural approach to pain treatment.”
