CDC advisory committee discusses who should get first vaccine doses
Equity is a high priority. Minorities have been especially hard hit by the virus, but could also find it hard to access vaccines.
A key committee that will advise the U.S. Centers for Disease Control and Prevention (CDC) on who should get the first doses of COVID-19 vaccine agreed Monday on initial priorities and an ethical framework. But the hours-long meeting of the Advisory Committee on Immunization Practices (ACIP) demonstrated just how complicated it will be to get the vaccine into the arms of millions of people.
First off, the different vaccines in development have different attributes, such as how they work and can be distributed, and it isn’t yet known which products will be approved first by the Food and Drug Administration.
Committee members emphasized that they want groups disproportionately affected by the virus — especially minorities and lower-income people — to have good access to vaccines. Ensuring that happens will require additional funding for local governments overseeing distribution, they said.
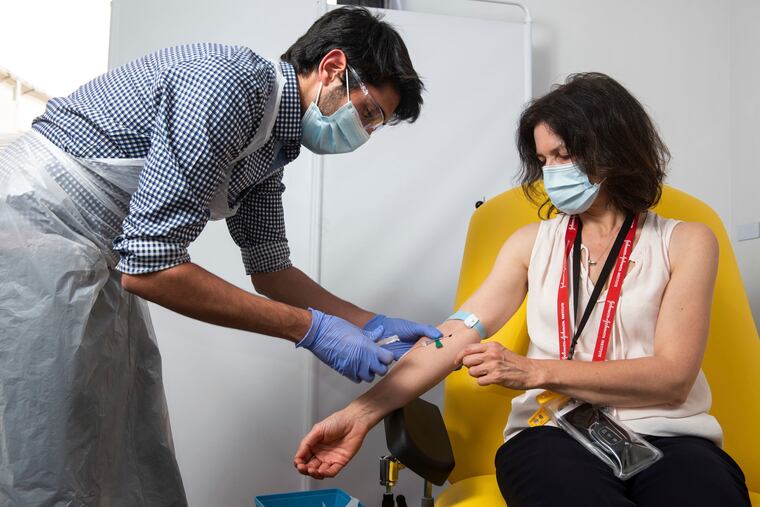
The committee generally agreed that health-care workers should get the first doses of vaccine because of the risks to them and their patients and because they play a crucial role in fighting the coronavirus. Vulnerable long-term care residents also are in this first group, though members debated their situation at some length. Essential workers, including food, education, and energy workers, as well a police and firefighters, should be in the second priority group because these workers often don’t have luxury of working from home and tend to be racially and demographically diverse.
The group’s work is growing more urgent.
» Here are Philly’s current COVID-19 guidelines: inquirer.com/phillyguidelines
Pfizer filed with the FDA for emergency authorization for its vaccine on Friday. Moderna, which also released late-stage results showing its vaccine was about 95% effective, has not yet done so. AstraZeneca on Monday said its vaccine was 62% to 90% effective in testing, depending on the dose. While the Pfizer and Moderna vaccines require very cold storage temperatures, complicating distribution, the AstraZeneca product does not. All require two doses, which will also make it more challenging to fully vaccinate millions of Americans.
» READ MORE: Why coronavirus vaccines seem to work better than expected
ACIP has said it will meet soon after the FDA approves a vaccine to make final recommendations. The CDC has usually accepted ACIP guidance.
Many traditions have been broken this year, though. A panel assembled by the National Academies of Sciences, Engineering, and Medicine also considered vaccine prioritization at the request of the National Institutes of Health (NIH) and the CDC. Plus, there is a new administration taking office in January, possibly after the first batch of doses have been shipped.
Last month, the Academies panel recommended that people be vaccinated in phases, with initial doses going to frontline health workers in hospitals, nursing homes, or home care as well as first responders like police officers and firefighters. Once more doses are available, people whose underlying health problems put them at high risk for severe disease and death could get shots along with those aged 65 and older who live in congregate settings, such as nursing homes, homeless shelters, and jails. In that framework, young adults, who are likely to spread the virus to more vulnerable groups, would get priority over healthy middle-aged people with relatively safe working conditions.
ACIP is initially prioritizing four groups most at risk for COVID-19: 21 million health-care workers, 87 million essential workers, more than 100 million adults with underlying health problems and 53 million people aged 65 and up, it said in a report released Monday in the CDC’s Morbidity and Mortality Weekly Report.
ACIP members Monday agreed with a framework that weighed priorities based on maximizing benefits, minimizing harms and promoting justice and equity.
Health-care workers came out on top, although there was some concern about whether employees who can work from home should be included at first. The three other groups had similar ratings when the committee considered the impact of vaccines on hospitalizations and deaths, on whether a group was likely to embrace vaccination, and on equity. Reluctance to get a vaccine is likely to be a significant problem, particularly among some minority groups.
» READ MORE: Once a COVID-19 vaccine is here, there will be a new challenge: Convincing people it’s safe
There were concerns about adding nursing home and assisted living residents to the highest priority group because they have not been included in vaccine clinical trials, and vaccines tend to be less effective in the elderly. Robert Atmar, a professor of medicine at the Baylor College of Medicine, was also worried about safety and whether reactions to the vaccine would lead to extra evaluations. Another committee member worried that residents would die for other reasons but the deaths would be blamed on vaccines.
However, others said the vaccines are likely to have some efficacy in this group, which has had an especially high death rate and lives in conditions that make it hard to hide from the virus. Plus, from a practical standpoint, it makes sense to vaccinate interested staff and residents at the same time.
The committee’s current priority list calls for putting people with chronic health conditions like obesity and diabetes as well as people aged 65 and up in one very large group after essential workers.
