Once a COVID-19 vaccine is here, there will be a new challenge: Convincing people it’s safe
Communications experts said there has never been a vaccine introduction like this one will be. What does science say about how to inform the public?
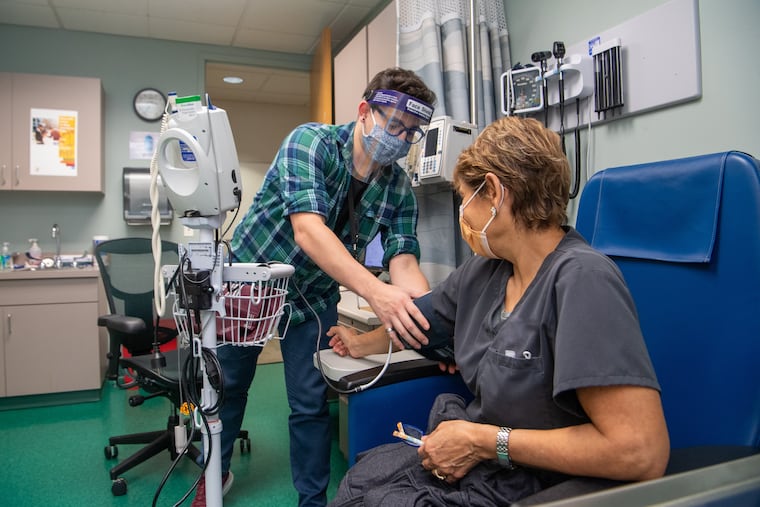
There’s a good chance that a coronavirus vaccine could be available by late 2020 or early 2021.
Developing an effective vaccine that fast would be a remarkable scientific achievement. It would also provide the first real hope of taming a new, deadly virus that has upended all aspects of American life — if people are willing to take it. Many may not be.
Polls show decreasing support for getting vaccinated as battles between science and politics have weakened trust in government agencies that evaluate and recommend vaccines. Enthusiasm for a vaccine is particularly low among Black Americans, a group that has been especially hard hit by COVID-19. Republicans are less likely to seek a vaccine than Democrats. Polling from STAT and The Harris Poll found that the percentage of Americans who said they would get a vaccine as soon as possible dropped from 69% in mid-August to 58% in early October. Several other polls have found that only about half of Americans now want a COVID-19 shot.
Because of politicization around vaccines, leaders of unions representing about two million health care workers announced Tuesday that they will not receive or administer a new coronavirus vaccine “without additional assurance from independent experts that the approval process has not been tainted.”
While support could easily grow once a vaccine is approved, the polling is worrisome because broad vaccination is the best way to block the virus. The alternative — herd immunity after most people have been infected — would lead to far more suffering and death, experts say.
» READ MORE: Herd immunity could protect us from COVID-19 — in theory
The issue is so important that a committee of the National Academies of Sciences, Engineering, and Medicine that was asked to set priorities for allocating early, scarce vaccine doses included chapters in its report earlier this month on the possibility that demand would be too low. The group emphasized the importance of “evidence-based” communication about vaccines so they actually are used.
» READ MORE: Medical workers should get coronavirus vaccine first, scientific group says
This raises an important question: What does the science of communication say about how to discuss a new vaccine for a new disease with a wary public?
A ‘whole new ball game’
People who study medical communication said any vaccine approved soon will face unprecedented challenges. While many Americans question the motives of pharmaceutical companies, people have in the past largely accepted guidance from the Food and Drug Administration and the Centers for Disease Control and Prevention, said Kathleen Hall Jamieson, director of the University of Pennsylvania’s Annenberg Public Policy Center. Both agencies have lost considerable luster this year because of allegations of politically motivated influence from the Trump administration.
“Science has become another voice in the room and not the voice,” said Rupali Limaye, director of behavioral and implementation research at Johns Hopkins University.
Confusion and distrust will make it harder to convince the public to try a new product, especially when some already had concerns about vaccines. Plus, some of the vaccines now in trials are very different from those in the past.
“This is a whole new ball game,” said Alison Buttenheim, a public health researcher at Penn Nursing who studies behavioral aspects of infectious disease prevention, including vaccine acceptance. “Anyone who says we know what messaging will work here is not correct.”
It did not help that the president, eager for a win on coronavirus, predicted a vaccine could be available before Election Day, raising the specter of an emergency authorization timed for political impact. It was an unlikely claim when he made it, and the FDA later changed its rules to make that timetable unworkable.
Multiple communications experts said that the very name of the government’s vaccine development effort, Operation Warp Speed, was a mistake. People want a vaccine as soon as possible, but they want to be sure it works, and they want it to be safe. There’s an association between breakneck speed and mistakes that will now have to be addressed.
The top priority will be restoring faith in the science of vaccine development. Assuming the first vaccine is indeed safe and effective, this will require exceptional transparency about the testing process. How many people got the shots? How long were they monitored for side effects? How well did the vaccine protect them?
Finding trusted messengers
Communications experts said it matters greatly who promotes the vaccine. People believe a “trusted messenger.” During the vice presidential debate this month, Sen. Kamala Harris illustrated how this works. “If the public health professionals, if Dr. [Anthony] Fauci, if the doctors tell us that we should take it, I’ll be the first in line to take it — absolutely,” she said in response to a question. “But if Donald Trump tells us that we should take it, I’m not taking it.” Of course, in politically fractured America, some people might take the opposite approach.
The important lesson is that people want to know that someone they respect recommends the vaccine. This could be a national political figure, but people are most likely to respond to local leaders, especially family doctors and local nurses, communications experts said. They may also listen to ministers, family members, and celebrities. For those who, like Harris, trust science and Dr. Fauci, it could be a scientist. Philip Massey, a health communications expert at Drexel University’s Dornsife School of Public Health, said public health officials should be talking with groups like Black Lives Matter activists about vaccines.
The message itself needs to vary with each group’s concerns. How does the vaccine work for people over 65? Was it tested in large enough numbers of Black people to address the fears of a group that has historic reasons to be wary of medical research?
“It’s not going to be one message that works for everybody,” Buttenheim said.
Some people will want numbers, and Baruch Fischhoff, a psychologist who studies risk assessment at Carnegie Mellon University, believes most of us can understand them if they’re presented properly. He believes public health officials should be laying the groundwork for that communication now. He would begin by explaining how many people were in the trial and how long they were followed. Some percentage of participants had serious side effects. A company may say that a vaccine is 60% effective, but what does that mean? It could be that 30% of participants were totally protected and 30% had milder symptoms, while the vaccine had no effect on the rest. People should see those numbers, said Fischhoff, who, like Buttenheim, was on the Academies of Sciences vaccine committee.
Once that foundation is laid, Fischhoff said, people will be more receptive to campaigns asking them to get the vaccine.
Dominique Brossard, chair of the department of life sciences communication at the University of Wisconsin-Madison, thinks it’s best to keep messages simple and include links to more detailed data for people who want to go deep. If numbers must be used, make them concrete. Most people, for example, can’t visualize what 225,000 deaths — the current national death toll — means. They might understand it better if they knew that’s the population of Brossard’s town: Madison. It’s also more than two Allentowns.
Most research on vaccine communication has centered on children and parents reluctant to vaccinate, Brossard said. There’s much less evidence about adult vaccines. She thinks attitudes toward flu shots — some people get them every year and some never do — will likely spill over onto a coronavirus vaccine. People underestimate the risks of COVID-19 most likely because they don’t personally know anyone who has been seriously ill. Public health officials, she said, need to tell stories that emphasize both the short- and long-term impact of COVID-19.
» READ MORE: Don’t know any COVID-19 patients who’ve died or been in the hospital? That may explain a lot.
She added that messages need to be short, emotionally appealing, and consistent.
Massey said any vaccine campaign will need to address the 3 C’s: confidence in the vaccine, complacency about the disease and convenience of getting the vaccine. He hopes that giving the vaccine first to frontline workers, who have been pandemic heroes, may sway others.
Jamieson thinks it likely will be helpful to compare the risks of the vaccine with the much greater risks of COVID-19.
Buttenheim said some people may respond to pleas to help their communities even if they are not personally worried about the disease. Overall, the message should be simple: “This is safe. This is effective. This is the norm. This is what everybody is doing, and this is what people I admire are doing.” Messaging about where and when to get vaccines needs to be equally straightforward.
Limaye says it’s not helpful to argue against misperceptions. Instead, pivot to the severity of the disease and the person’s susceptibility to it. If they’re not worried about themselves, maybe they would get a shot to protect an older relative.
» HELP US REPORT: Are you a health care worker, medical provider, government worker, patient, frontline worker or other expert? We want to hear from you.
Some people may be deep into conspiracy theories or social media information bubbles. Jamieson said the only hope is to expose them to frequent positive messages about vaccines, because familiarity increases the perception of accuracy.
But Buttenheim said, "There are some people we’re not going to be able to persuade. It is what it is.”
