The COVID-19 pandemic may make getting health insurance harder. Here’s why.
If the Supreme Court invalidates the ACA, more than 20 million people — including at least 1.5 million Pa. and N.J. residents — would lose health insurance gained through healthcare.gov.
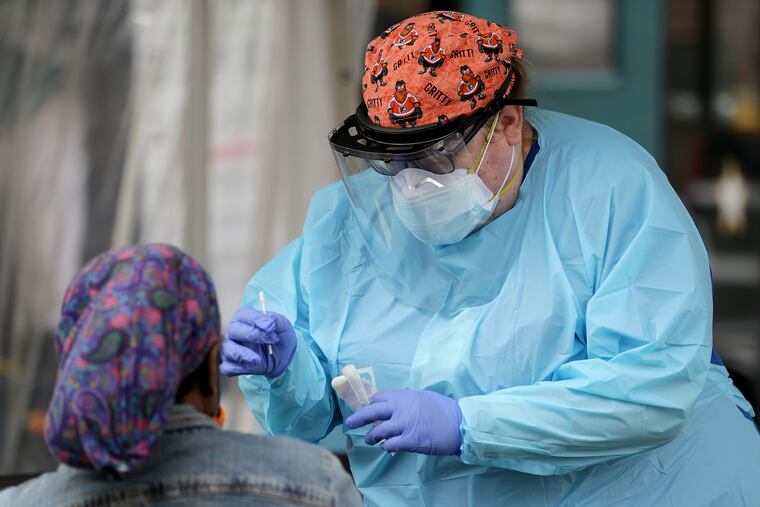
The high cost of treating COVID-19, its long-term health complications for those who recover, and the economic ramifications of the pandemic are driving home the value of the protections created under the Affordable Care Act — and how much trouble many Americans will find themselves in if the law is overturned.
A week after the presidential election, the U.S. Supreme Court is expected to hear arguments in a lawsuit brought by Texas and a group of Republican attorneys general that seeks to get rid of the Obama-era health-care law. An opinion is expected to be handed down next year.
If the court decides that the ACA should be tossed, more than 20 million people — including at least 1.5 million Pennsylvania and New Jersey residents — would lose health insurance they gained through the federal healthcare.gov, a state-based ACA marketplace, or Medicaid expansion.
Many more people, even some who get it through an employer, would be affected by the reversal of one of the law’s most popular insurance rules: protections for people with preexisting conditions. More than one in four people have a medical condition that, before the ACA, would have made them uninsurable.
“Insurance coverage is a little bit like a game of musical chairs,” said Karen Pollitz, a senior fellow at the Kaiser Family Foundation who studies health reform and private insurance. “With the ACA reforms, there was a much higher likelihood that if you lost your job, there would be another chair for you.”
Millions with preexisting conditions
Before the Affordable Care Act, insurers selling individual health plans were allowed to deny coverage entirely, exclude coverage for certain medical problems (or body parts), or charge higher rates for “riders” to a policy that would cover a person’s preexisting condition.
For instance, in one study of pre-ACA individual health plans, Pollitz found that insurers were willing to sell health insurance to a fictional woman who took prescription medication for seasonal allergies, but excluded coverage for allergies — and her entire upper respiratory system. Paying out-of-pocket for allergy medications may not seem too harsh, but in this case, if she developed lung cancer or punctured a lung during a car accident, she’d be on her own to pay those expenses, too.
The Kaiser Family Foundation, a nonprofit health policy organization in Washington, estimates that about 27% of adults under age 65 — about 54 million people — have a preexisting condition that would have made them uninsurable in the individual market. Congestive heart failure, diabetes, severe obesity, and pregnancy are some of the medical conditions that would have been reason enough for an insurer to refuse to sell someone an insurance policy.
As many as 133 million people have a condition, such as allergies, high blood pressure, or a history of smoking, that could make it harder for them to get insurance, according to the Kaiser Family Foundation.
Depression, anxiety, and substance abuse — all on the rise during the pandemic — were routinely excluded from insurance before the ACA mandated that insurance plans cover mental and behavioral health services.
People who developed a medical condition after buying their individual plans weren’t necessarily in the clear. Before agreeing to pay a bill for, say, a brain tumor, insurers routinely looked back at a person’s medical history for any indication that a problem was brewing.
This practice of evaluating people’s underlying medical conditions and determining how expensive they would be to insure — and whether they should be covered — is called medical underwriting. It enabled insurers to keep premium prices low by excluding people who would generate costly medical bills.
“It was just math: How can I make claims go away?” Pollitz said. “In a competitive market, when insurers are trying to keep premiums lower than the other guy, it doesn’t pay to be more lenient.”
For that reason, analysts say COVID-19 would likely be added to the list of preexisting conditions.
Hospitals are billing an average of $73,000 for COVID-19 treatment, with treatment for severe cases costing even more, according to FAIR Health, a data analysis company. Other factors make the virus additionally risky for insurers: Researchers are still learning about how to treat it, there’s no vaccine yet, and it appears to be associated with costly long-term effects on survivors' lungs and other organs.
Pollitz said it’s possible some plans could refuse to sell insurance plans to people who have recovered from a severe case of the virus, while plans being sold to healthy individuals could exclude coverage for any future COVID-19 treatment.
» READ MORE: The coronavirus is exposing America’s eye-popping health-care charges: One dad’s 10-day hospital stay cost $97,000
Threats to employer plans
People with employer plans shouldn’t ignore the threat of losing the ACA’s protections, just because they don’t use Medicaid or the individual marketplace.
Employer-sponsored health plans, the most common type of insurance for Americans under age 65, have not been allowed to deny coverage entirely because of a preexisting condition since the 1990s, but could refuse to cover a particular condition for up to one year. The ACA banned such delays. People who changed jobs were guaranteed coverage for their preexisting condition under their new employer’s health plan, so long as they didn’t have a gap in coverage of more than two months.
But as the pandemic has proved, prolonged stints of unemployment can come up unexpectedly.
“Most of us are, at some point, going to have the need for individual health insurance,” Pollitz said.
» READ MORE: Unemployed and uninsured because of coronavirus? You may be eligible for Medicaid.
Millions of people lost their jobs due to pandemic lockdowns, which forced many to navigate the unemployment system and alternatives to employer health insurance for the first time in their careers.
A study by the Urban Institute and the Robert Wood Johnson Foundation found that a third of people who lost insurance due to a pandemic layoff have remained uninsured. While staggering, that number would have been higher, if not for the ACA’s marketplaces and Medicaid expansion.
Another third were able to regain coverage through a spouse’s health plan. And the remaining third signed up for an ACA marketplace plan or became newly eligible for Medicaid.
In states that expanded Medicaid, individuals with annual income up to 133% of the federal poverty level ($16,971 for an individual and $34,846 for a family of four in 2020) are eligible for coverage.
About 95,700 Pennsylvania residents gained Medicaid coverage between February and May, a 3% increase after years of flat enrollment, according to data analysis by the Kaiser Family Foundation.
