After seeing patients and taking risks all year, Pa.’s private doctors have been left out of the vaccination process
Even physicians who are “on staff” with a hospital system — not on the facility’s payroll but able to access services and equipment for their patients — have largely been left out.
Editor’s Note: A previous version of this article failed to include context about the distribution efforts of The University of Pennsylvania’s health system. Penn, which includes Chester County Hospital, had distributed vaccine doses to health care workers who are not employees prior to the state’s order Wednesday. As of Thursday, Chester County Hospital had given about 450 doses to non-employees, 15% of all doses the hospital has received.
Doctors, nurses, and staff at private practices and clinics across Pennsylvania have been left guessing when they would get access to a COVID-19 vaccine, even as they regularly interact with patients infected with the coronavirus.
Even physicians who are “on staff” with a hospital system — not on the facility’s payroll but able to access services and equipment for their patients — have largely been left out as those institutions have had free rein to determine which of their employees can have access to limited vaccine doses.
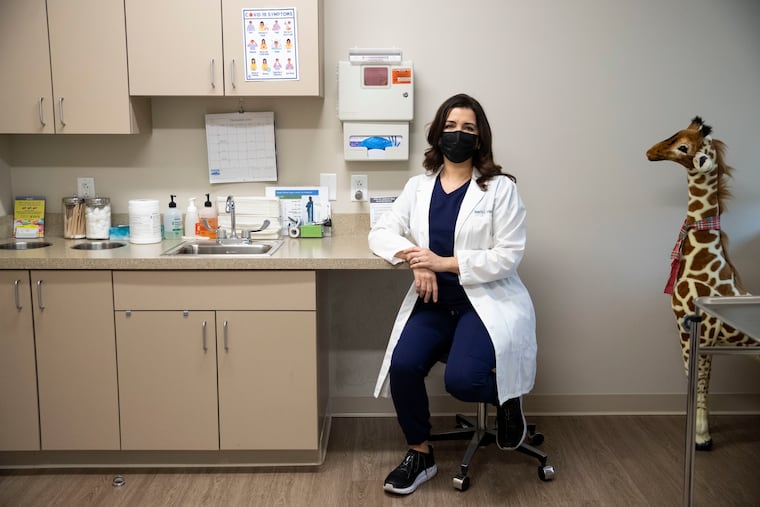
“They just kind of started doing their people without offering it to others,” said Rannette Schurtz, a physician who practices at Gateway Medical Associates in Downingtown and is on staff at Chester County Hospital. “I just assumed I would be one of those people.”
Rachel Levine, the state’s health secretary, issued the first guidance Wednesday for about 450,000 health-care workers in Pennsylvania not employed by hospital systems. The state will require hospitals, health systems and centers, and pharmacies to set aside 10% of all vaccine shipments delivered as of Jan. 6 for those workers. These institutions are being asked to develop a process to distribute doses beyond their own employees, a Health Department spokesperson said.
Along with doctors, nurses, and technicians, the order also applies to a swath of direct and indirect health-care providers including pharmacists, students, EMTs, and clinical workers at schools and detention facilities. Those workers are being asked to identify a place to obtain the vaccine if it’s not being provided through an employer.
The state’s response came after receiving a letter Monday to the governor and Levine from nine Pennsylvania physicians’ organizations criticizing the lack of information for clinics, small practices, and urgent cares.
“The current interim immunization plan does not clearly address where and how the providers and staff at these independent practices and clinics are to receive their COVID-19 vaccine,” the letter stated. “This is creating a two-tiered health care provider immunization system for COVID-19 — those who have large economic bargaining power and those who do not.”
» READ MORE: COVID-19 vaccinations begin for Pa., N.J. nursing home residents, but logistical hurdles still loom
The Health Department’s new order is a good start, said David Silbert, a Lancaster eye doctor and president of the Pennsylvania Academy of Ophthalmology, one of the letter’s signatories.
“It’s just making sure the hospitals work with the rest of the community,” he said.
Many physicians in private practice have relationships with hospitals, and the new order should ensure their hospitals provide doses for them. It is less certain whether the order will help health-care workers who do not maintain a regular relationship with a hospital system, Silbert said.
“There’s limited supply of vaccine — everything didn’t come in as everyone had hoped for — so the institutions got it,” said Mark Austerberry, executive director of the Philadelphia County Medical Society. “We’re concerned that [private] physicians should be right up there at the front of the line.”
Philadelphia‘s Public Health Department, which has its own vaccine allotment separate from the state, has asked health-care workers not primarily employed by a hospital to fill out a registration form to get instructions on how to make an appointment for vaccination in mid-January.
Silbert would like to see the state follow Philadelphia’s approach, also in place in Allegheny County, so nonaffiliated health-care workers are accounted for and get doses.
Vaccine distribution began in Pennsylvania this month with the first shots largely going to health-care workers and some long-term care facility residents, but already the logistics are tangled. President-elect Joe Biden said Tuesday that, at the current pace, vaccinating the country could take years. He committed to greater federal involvement in the distribution process to reach his goal of 100 million people vaccinated in the first 100 days of his presidency.
» READ MORE: Biden vows to accelerate vaccine rollout after data shows current pace would take 10 years
“I’m personally disappointed,” Gov. Tom Wolf said in a news conference Wednesday, “that the vaccine [wasn’t] rolled out faster and in a much more efficient manner than it has been.”
More than 117,000 vaccine doses have been distributed in Pennsylvania this month.
The federal government has left it to states to create their own vaccination plans, but those efforts have been stymied by a lack of basic information, such as uncertainty over how many doses will be available from week to week, health officials have said.
The pandemic has taken a toll on private practices and clinics, many of which are essentially small businesses without the financial resources of large health systems.
“We almost had to close at the beginning,” said Erik Soiferman, whose Horsham clinic, Liberty Urgent Care, sees 14,000 to 16,000 patients a year. “Urgent cares are not recognized as the important medical delivery system that they are.”
» READ MORE: COVID-19 vaccine could go to seniors over 75 in just weeks, leaving states with huge logistics problems
With the vaccine’s two-dose regimen necessary to provide the maximum immunity, Soiferman needs about 50 shots for his staff. Private medical offices have cut hours and reduced pay for staff, doctors said, but by staying open they have helped keep emergency rooms from being overwhelmed.
“People are afraid to go to the hospital right now, so they’ll come here,” said Dana Mincer, a doctor at Liberty Urgent Care. “Even if primary-care doctors tell them to go to the ER, they’ll still sometimes come here first.”
Staff there treat and interact with COVID-19 patients daily, typically swabbing 200 people a day for coronavirus tests, Mincer said.
Since health-care workers became eligible for vaccine doses, some private physicians have been left to call in favors or scramble to get inoculated. Schurtz, the Chester County physician, got a shot through Chester County Hospital, owned by Penn Medicine, this weekend, and thinks that’s because her practice sends considerable business to the hospital system’s labs.
» READ MORE: COVID-19 vaccine gives Philly health-care workers a glimpse of pandemic hope. Then it’s back to work.
“Because we’re such a large practice, our COO reached out to Penn and kind of nagged them,” she said.
A Gateway spokesperson disputed Schurtz’s account, saying the practice was contacted by Chester County Hospital on Dec. 24 about the opportunity to vaccinate staff.
Schurtz credited the system with making doses available Sunday, before the state health department issued its order.
“They were very generous to do that,” she said. “The thing is, the department of health gave the hospitals these vaccines and said give it to health care professionals and they didn’t really instruct how that should be done.”
Penn’s health system, which includes six hospitals in the region, has had a “proactive and robust plan” to distribute doses to health care workers with a relationship to their health care system prior to Levine’s request, a spokesperson said. As of Thursday, about 15% of the approximately 3,000 doses Chester County Hospital received have gone to health care workers who are not employees.
“We are grateful for the proactive offer from Chester County Hospital and relieved that many of our frontline staff are vaccinated,” a Gateway spokesperson said.
“There’s limited supply of vaccine — everything didn’t come in as everyone had hoped for — so the institutions got it. We’re concerned that [private] physicians should be right up there at the front of the line.”
Andrew Lubell, a pediatrician from Flourtown, made little headway in his efforts to get information from the state Health Department or Montgomery County.
“I’d basically hit a brick wall,” he said. “There was no plan in place.”
Then, at 5 p.m. Tuesday, he received a call from a Walgreen’s in Norristown with 200 doses left over after a vaccination clinic at a long-term care facility. The pharmacy had contacted Montgomery County’s Health Department, Lubell said, and the county recommended it contact his practice, Lockman & Lubell Pediatric Associates, of Fort Washington.
If he could get to the pharmacy before 8 p.m., he was told, he and most of his staff of 27 could be vaccinated that night. He rushed to the pharmacy and found himself behind 20 people who’d also scampered to take advantage of the last-minute availability.
“The good thing is they didn’t waste doses, thank God,” Lubell said. “If we had had a proper federal response and the military and the National Guard had been used properly as a chain of command, this could have been rolled out in a more sophisticated and equitable way.”
