The COVID-19 rush never came to rural Pennsylvania, and empty hospitals are feeling the losses
A recent report estimated that Pennsylvania hospital revenue losses may exceed $10 billion as a result of the COVID-19 pandemic.
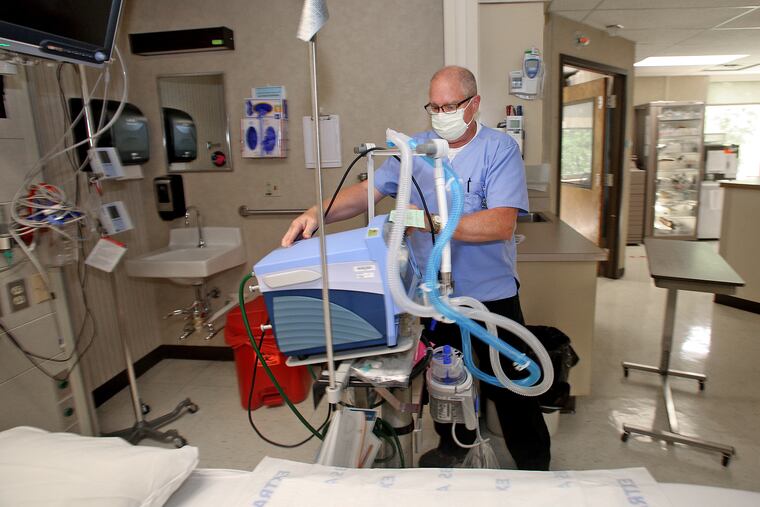
TYRONE, Pa. — The windows of the intensive care unit in this small Blair County town’s hospital look out to a forest’s edge. Whitetail deer often emerge to chew some grass, groundhogs to waddle along. There’s just no one there to see it.
The five-bed ICU was empty during a weekday afternoon earlier this month, and the rest of Tyrone Hospital felt a bit barren as well. The COVID-19 rush never hit Blair County, with just 49 confirmed cases among its 121,829 residents as of Friday. The hospital, 220 miles west of Philadelphia, has had one patient with COVID-19 during the pandemic, and that person was sent home. On some days, the 25-bed hospital saw only a handful of patients.
“It was quiet, but we kept the minimum staff we had to to make sure we were prepared,” said Anna Marie Anna, acting CEO of Tyrone Regional Health Network and its 160 employees.
Hospitals all over the country, like Tyrone, increased spending to stockpile personal protective equipment in preparation for that threatened rush of patients, while cutting back on outpatient services and elective surgeries. The result, three months later, is major revenue losses, and that could prove hard for rural and small-town hospitals like this one in Tyrone, population 5,194, to weather.
Anna said Tyrone’s emergency room outpatient business makes up 85% to 95% of yearly revenue. The hospital brings in about $5 million to $6 million a month, she said, and in April that revenue was down by three-quarters.
“That’s a big cut,” she said.
Statewide, COVID-related hospital losses could exceed $10 billion, according to a recent report from the Hospital and Healthsystem Association of Pennsylvania (HAP). Even with an expected $3.1 billion from the federal Coronavirus Aid, Relief, and Economic Security (CARES) Act, HAP said, the losses could still exceed $7 billion.
"Among hospitals large and small, and in every part of the state, preparing for and responding to COVID-19 has brought tremendous financial strain across the board,” Andy Carter, HAP’s president and CEO, said in a statement.
» READ MORE: In a Pennsylvania ‘green phase’ county, people head out for haircuts, spin class, and pints of beer
Spokespeople for Temple University Hospital and the University of Pennsylvania Health System did not return requests for comment on the HAP report, but Lisa Davis, director of Pennsylvania’s Office of Rural Health at Pennsylvania State University, said rural hospitals have traditionally operated on the margins.
“They don’t necessarily have the reserve to offset those losses,” Davis said.
Rural hospitals nationwide were endangered long before the pandemic touched down in March, as populations in their areas grew older and smaller. States that have not adopted expansion of Medicaid, like Texas, have suffered the worst. According to the U.S. Government Accountability Office (GAO), 64 rural hospitals across the country closed from 2013 through 2017 — more than twice the number in the prior five-year period. In 2019 alone, 18 were shuttered. In March, the University of Pittsburgh Medical Center’s Susquehanna Sunbury Hospital closed in Northumberland County. Two other hospitals have gone out of business in rural Pennsylvania since 2012.
In a recent virtual seminar on rural hospitals and COVID-19 hosted by the University of Pennsylvania’s Leonard Davis Institute of Health Economics, Lisa Davis and other panelists laid out the factors that make health care more difficult in less-populated areas. The workforce is smaller, the pool of potential replacements likewise. The population in rural counties is older, and according to the Centers for Disease Control and Prevention, rates of heart disease, cancer, chronic lower respiratory disease, and stroke are all higher than average there. Smoking rates are higher. Obesity, too.
“So, not only do rural hospitals have the burden of being challenged with a smaller or shorter ‘bench,’ but they also treat patients that are more vulnerable to COVID-19 because of their preexisting conditions,” said panelist Karen Murphy, executive vice president and chief innovation officer of the Geisinger Health System, based in Danville, Montour County.
Guthrie Health operates three hospitals in rural Bradford County, including one in Sayre. The three saw about 40 COVID-19 patients, said Dr. Joseph A. Scopelliti, president and CEO. Numbers have been going down.
» READ MORE: Pennsylvania racetracks idling, wondering whether COVID-19 restrictions will empty tanks
“I can tell you that this is the first time in 78 days that we don’t have a patient under investigation for COVID,” Scopelliti said on June 9. “The first cases were in April, and we’ve tapered down pretty quickly.”
Scopelliti said Guthrie’s operating revenue is about $85 million a month. “We’ve seen reductions of 50% to 60%,” he said.
Though Blair County, like Bradford, moved into the “green” phase of reopening last month, easing most stay-at-home restrictions on residents, Tyrone Hospital will still require all patients and visitors to wear masks and have their temperatures checked at the door. Patients for the most part have stayed away, Anna said.
“How do we get patients to want to come out and feel safe enough to come out, so we can recover our business? We want them to know it’s safe to come to the hospital if you need it,” Anna said. “And of course, we have to worry about the fall, if this comes back. What do you do then?”
» FAQ: Your coronavirus questions, answered.
Recent reports of possible “second waves” of COVID-19 cases have been reported, with both Texas and Florida seeing their highest number of confirmed cases in recent days. During the Penn seminar, panelists mentioned a trend that has worried officials in rural counties since the beginning of the pandemic: people fleeing populated areas for rural getaways, filling up hunting camps, vacation homes, and rentals. Rural real estate agents have told The Inquirer that interest in sales and rentals is higher than ever.
If those numbers do boomerang in rural Pennsylvania, hospitals like Tyrone, which has three ventilators, will be ready. Anna said that won’t change the revenue losses.
“We want to cover what we lost,” she said. “Or something close to it.”
